Myocarditis - what kind of disease is it?
Myocarditis is a heart disease characterized by inflammation of its middle layer, the myocardium.
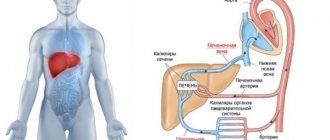
Myocardium is a cardiac muscle formed from a tight junction of muscle cells - cardiomyocytes. The myocardium is the middle layer of the heart, while its inner layer is called the endocardium and the outer layer is called the pericardium.
The myocardium performs the function of contracting and relaxing the heart, due to which one of its main functions is performed - blood circulation.
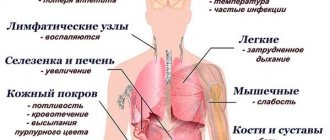
The main symptoms of myocarditis are discomfort and pain in the heart area, arrhythmias, shortness of breath, general malaise, and fever.
The main causes of myocarditis are infection, especially viruses, bacteria, fungi and protozoa. Very often, myocarditis is not an independent disease, but develops against the background of other diseases, mainly of an infectious, allergic and rheumatic nature.
Development of myocarditis
Several factors may be involved in the development of myocarditis, the most common of which are:
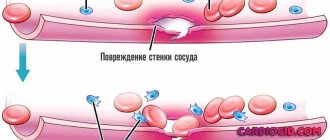
Infectious factor - the development of the disease is caused by infectious agents, which, when circulating in the blood vessels, reach the intracardiac chambers and valves, settle in them and, with an increase in their population, form an inflammatory focus. From infection of the body to the appearance of the first signs of inflammation, it can take from several days to a couple of weeks. In turn, inflammation of the heart valves and other manifestations of infectious damage to the endocardium contribute to the formation of blood clots and fibrous deposits, which, as they spread, can affect the myocardium, and in case of complications, reach the pericardium.
Immunopathological reaction during systemic infections (diphtheria, scarlet fever, influenza, meningitis and others) - specific cells (antigen-antibody reaction) T-lymphocytes and antibodies of humoral immunity in response to infection of the body and sedimentation of infection in “target organs”, for example in the myocardium, they begin to destroy cardiomyocytes. This is due to the fact that, for example, the Coxsackie virus is very similar to the cell membrane of cardiomyocytes, therefore, after inactivation of the virus, the process of producing antibodies to it continues further, damaging myocardial cells. Infection and immunopathological effects on myocardial cells lead to serious disturbances in their structure, as well as in the structure and function of interstitial tissue and blood circulation. An inflammatory process appears in the myocardium with an infiltrate consisting of lymphocytes, macrophages, eosinophils, neutrophils and other cells, which disrupts blood circulation and causes spasm of arterioles, paresis of veins and capillaries, congestion of microcirculatory vessels, impaired vascular permeability, dystrophies, fibrin microthrombi, erythrocytes appear. stasis, stromal edema, necrosis of cardiomyocytes, which are later replaced by fibrous tissue. At the same time, the energy metabolism of cardiomyocytes, the process of glucose utilization, β-oxidation of fatty acids, and the number of glycogen granules in myocardial cells are disrupted in the myocardium. Dystrophic changes in the myocardium are accompanied by a decrease in its contractility, a decrease in the systolic and diastolic functioning of the left ventricle, stagnation in blood circulation (usually the pulmonary circulation), and the appearance of blockades (atrioventricular and intraventricular). Prolonged inflammation of the myocardium, usually after the 14th day of the disease, contributes to the appearance of cardiosclerosis, often called myocardial cardiosclerosis.
Myocarditis – ICD
ICD-10: I09.0, I51.4; ICD-9: 391.2, 422, 429.0.
Kinds
In clinical practice, etiological variants of myocarditis are distinguished, which differ from each other in characteristic signs, course, and prognostic significance. Depending on the exciting factor, appropriate treatment tactics are used. It is worth considering the most common etiological types of myocarditis.
Diphtheria myocarditis
The underlying disease is complicated by CM in 8% of cases. If the course of the disease is severe, then the risk of developing myocarditis reaches 50%. This is due to the fact that diphtheria toxin has a high degree of cardiotoxicity, due to which heart cells quickly die and become foreign agents for the body, to which an immune reaction is developed.
Clinic . The course is severe, the symptoms of heart failure are quite pronounced (shortness of breath, heart pain, swelling). Arrhythmias and heart blocks may occur. The first signs of myocarditis against the background of diphtheria often appear on the 8-10th day from the onset of the disease; a more favorable course of the disease is observed with the development of myocardial infarction in the third or fourth week of the disease.
Salmonella myocarditis
Often accompanies severe salmonellosis. It mainly manifests itself in children, and increases the risk of death. Salmonella infection can contribute to the formation of abscesses in the myocardium, resulting in fatal cardiac tamponade (stop).
Clinic . Symptoms develop progressively. At first, pain in the heart area and fatigue may occur, but gradually signs of severe heart failure appear, which in severe cases is complicated by vascular thromboembolism. Still, in most cases, the clinical manifestations of MC in salmonellosis are not very pronounced, which is confirmed by nonspecific changes on the ECG.
Septic myocarditis
The modern use of highly active antibiotics has made it possible to reduce the number of MKs arising against the background of sepsis to 4% of the total number of myocarditis. In septic MK, Pseudomonas aeruginosa, staphylococci, E. coli and other pathogenic flora are most often detected.
Clinic . Sepsis itself is characterized by a pronounced and severe clinical picture, to which, in the case of myocarditis, is added paroxysmal tachycardia or atrial fibrillation. The patient may have tachycardia that does not correspond to body temperature, which is usually elevated in sepsis. As the pathological process continues, heart failure develops.
Viral myocarditis
It is most often diagnosed among various etiological forms of myocarditis, which is associated with the high cardiotropism of the Coxsackie B virus. The disease can develop at any age, but there is evidence of an increase in the incidence of pathology after 50 years, and men are more susceptible to it. Women are at increased risk of developing viral myocarditis during pregnancy or after childbirth. If a pregnant woman has MK, there is a risk of stillbirth or the development of myocarditis both in the fetus and in the first 8 months after birth.
Clinic. Along with the characteristic symptoms of myocarditis, the patient may experience high fever and gastroenteritis syndrome, when nausea, vomiting, pain near the navel and in the upper abdomen appear. Additionally, inflammation of the testicles, enlargement of the spleen and lymph nodes can be diagnosed. There was a connection between the severity of the clinical picture of viral MK and the age of the patients. At 17-20 years of age, a more pronounced clinical picture is determined, with frequent manifestations of pleurisy or pericarditis, but everything ends in recovery. After 40 years, the clinical picture is less pronounced; there may be cardiac pain, mistaken for attacks of ischemic heart disease. Shortness of breath and palpitations also sometimes occur.
Myocarditis - symptoms
The appearance and course of the disease can occur with minimal symptoms, or even without them at all, which largely depends on the severity of systemic diseases, the localization of inflammation, the rate of progression, the person’s health status and various factors unfavorable to the body (for example, during a diet).
The first signs of myocarditis and the speed of their manifestation depend on the etiology of the disease. So, with an infectious and infectious-allergic nature, symptoms of inflammation appear after 10-14 days, with intoxication (food or drug poisoning) - 12-48 hours after taking the medicine.
The first signs of myocarditis
- Increased body temperature;
- General weakness and malaise;
- Skin rash, muscle and joint pain are also possible.
Main symptoms of myocarditis
- Violation of the contractile function of the heart muscle, accompanied by arrhythmias;
- Feelings of cardiac arrest;
- Pain in the heart area, which is paroxysmal or aching in nature;
- General malaise, soreness, weakness, increased fatigue;
- Shortness of breath, especially increasing with physical activity;
- Swelling of the legs;
- Decreased urine volume;
- Body temperature is normal, elevated or high, depending on the cause of the disease (for viral etiology - elevated and high, allergic and rheumatic - normal);
- Blood pressure is normal or low;
- Increased sweating;
- Pale skin, sometimes with a bluish tint, especially on the tips of the fingers, nose, ears;
- Uneven pulse;
- Additional symptoms that may accompany myocardial inflammation are a feeling of heaviness and pain in the right hypochondrium, muscle and joint pain, dilated veins in the neck (these are signs of heart failure).
Read also Arrhythmia. Causes, symptoms, types and treatment of arrhythmia
Infectious myocarditis: treatment, symptoms, prognosis, forms, complications, diagnosis, prevention
Inflammation of the heart muscle (myocardium) gives the name to such a disease as myocarditis, which in one form or another occurs in 5-10% of cases of diseases of the cardiovascular system. Cases of infectious diseases are becoming the most common causes of myocarditis. Today’s article is dedicated to him.
Features of the disease
The disease can develop in almost any age group of the population, but most often it affects people of “middle” age (30-40 years). At the same time, representatives of the fairer sex are at risk more often than men, although in the latter the inflammation has more severe forms.
Due to the sluggishness and lack of expression of symptoms, the diagnosis of myocarditis often does not occur at the initial stage of the disease.
It is customary to distinguish three types of myocarditis, including infectious and infectious-allergic, as well as rheumatic. The first one is one of the most common.
It occurs due to the entry of harmful microorganisms such as bacteria and viruses into the myocardium.
A specialist will talk about the features of the manifestation of infectious and other types of myocarditis in the following video:
Forms and types
As with most diseases, infectious myocarditis is usually divided into acute and chronic (active and persistent), as well as transient forms of the disease.
- Acute myocarditis. Manifests itself together with heart failure.
- Chronic myocarditis: Active. The patient develops cardiomyopathy, manifestations similar to the above forms are possible.
- Chronic. Active borderline myocarditis may occur; the left ventricle, however, functions normally. Heart failure may develop.
- Fleet myocarditis. Its manifestations are cardiogenic shock; destruction of heart cells (cardiomyocytes) is also common, as well as left ventricular dysfunction.
As for the clinical classification, infectious and infectious-allergic myocarditis, depending on the precursor disease, are divided into:
- Viral (eg influenza, polio)
- Bacterial/infectious (eg scarlet fever, typhoid fever)
- Parasitic (ex. Chagas disease)
- Rickettsial (ex. Q fever)
- Spirochetosis (ex. syphilis)
- Fungal (eg candidiasis).
Sometimes infectious myocarditis occurs in combination with toxic (occurs when taking certain pharmacological drugs).
Causes
As already mentioned, the main root cause of infectious type myocarditis is the introduction of parasites, bacteria and similar microorganisms into the heart muscle (myocardium). Most often it occurs due to the activity of pathogenic microorganisms that can destroy cardiomyocytes. They provoke damage to the upper respiratory tract.
To counteract the infected cells, the body begins to produce special antibodies, as a result of which all muscles are destroyed.
- The patient first experiences a breakdown of myocardial fibers and accumulation of mono- and plasma cells in this area.
- Next, the affected area is replaced by connective tissue, which, accordingly, leads to cardiosclerosis. Compensatory muscle hypertrophy also appears.
- Also, the pericardium may be involved in the development of the disease, as a result of which the patient begins to develop pericarditis (serous/serous-fibrous).
The bacterial type of myocarditis is characterized by the appearance of abscesses in which strepto- and staphylococci, as well as other similar microorganisms, “settle”. Next, we'll look at the specific symptoms and signs of infectious myocarditis.
Symptoms
As already mentioned, the symptoms of the disease are rarely pronounced at the very beginning, which creates problems on the way to diagnosing it. As the disease progresses, the patient may notice the following signs of a problem:
- increased sweating;
- fast fatiguability;
- general weakness and decreased performance;
- discomfort in the joints;
- rapid and arrhythmic pulse;
- low blood pressure;
- pallor, sometimes blueness of the skin;
- shortness of breath with minor physical exertion.
If the patient also has heart failure, then myocarditis may manifest itself in the form of swelling of the veins of the neck.
But the most important symptom is constant pain (pressing/stabbing) in the area of the apex of the heart, to the left of the sternum. In this case, the body temperature either remains normal or becomes low-grade.
Note! To distinguish myocarditis from angina attacks, it is necessary to take nitroglycerin. With inflammation, discomfort remains.
The difference between this type of myocarditis and rheumatic one is that the first begins to develop against the background or immediately after an infection.
Due to the latency of the manifestation of signs of the disease, usually about a third of the above symptoms are enough to start worrying and go for a diagnosis. Myocarditis is often accompanied by pericarditis.
These are the clinical signs of infectious myocarditis, now let’s look at the features of its diagnosis.
The video below will tell you more about the symptoms of infectious myocarditis, as well as about the viruses that cause the disease:
Diagnostics
The problems with diagnosing the disease consist, as already mentioned, in its often asymptomatic nature. Physical examination of the patient is therefore difficult. That is why, if inflammation of the heart muscle is suspected, the doctor prescribes a series of tests. They are:
- Electrocardiography. This non-invasive test will give the doctor a “picture” of the potential differences that occur as the heart pumps. The manifestations of atrial fibrillation and bundle branch block observed during the study indicate severe myocardial damage.
- Echography of the heart. This non-invasive test is performed using ultrasound waves. Helps identify different degrees of cardiac muscle dysfunction, as well as intracavitary blood clots.
- Chest X-ray. It will help to identify congestion in the lungs and expansion of the boundaries of the “motor”.
- Isotope study of the heart. Thanks to this method, it is possible to visualize the affected area and muscle necrosis.
- Endomyocardial biopsy. This study is carried out on the basis of the DDC (Dallas Diagnostic Criteria).
- Blood culture. Needed to confirm the viral etiology of myocarditis.
- Blood tests. A general and immunological analysis, as well as blood biochemistry, are performed.
- Probing of the cavities of the heart and its radioisotope study, as well as MRI, can also be performed.
- Outpatient treatment is indicated for patients with mild myocarditis.
- In case of moderate and severe forms of the disease, hospitalization cannot be avoided.
In a therapeutic way
There is currently no universal treatment method; the doctor usually insists on therapy to reduce inflammation or destroy its sources.
Also, the doctor, in the case of non-drug treatment, usually prescribes to the patient:
- limit consumption of table salt;
- minimize the consumption of alcoholic beverages;
- eat rationally and nutritiously;
- reduce the amount of physical activity;
- quit smoking.
Bed rest and oxygen inhalation are considered useful.
By medicinal method
It usually consists of taking three types of drugs:
- antihistamines;
- non-steroidal anti-inflammatory;
- immunosuppressive.
In severe cases, glucocorticoid hormones may be used.
Commonly used drugs:
- indomethacin,
- ibuprofen,
- glucocorticoids,
- prednisolone,
- voltaren.
In order to improve myocardial metabolism, the doctor prescribes potassium-containing medications such as asparkam, cocarboxylase, vitamin complexes and riboxin. Anticoagulants and antiplatelet agents may also be prescribed (to prevent thromboembolic complications). The average duration of treatment is 6 months.
A well-known TV presenter will talk about the features of preventing myocarditis in the following video:
Prevention of infectious myocarditis
People who have had infectious myocarditis should be examined by a cardiologist every 3 months.
Also, to prevent the development of myocarditis, you should:
- avoid parasite bites (especially ticks);
- limit communication with potential patients with infectious diseases;
- get vaccinated against diseases such as: Flu;
- Piggy;
- Measles;
- Rubella;
- Polio.
It is also worthwhile, under the supervision of a doctor, to sanitize foci of chronic infection in the body. Read on to learn about the possibility of complications and whether recurrent infectious myocarditis occurs.
Myocarditis - complications
- Myocardial cardiosclerosis;
- Myocardial infarction;
- Stroke;
- Heart failure;
- Arrhythmias (tachycardia, atrial fibrillation, extrasystole);
- Meningoencephalitis;
- Thrombosis and thromboembolic complications;
- Septic shock;
- Endocarditis, pericarditis;
- Death.
Basic concepts. Causes
Viral myocarditis is a pathological condition associated with damage to the heart muscle. As a result, some functions of the heart are disrupted: conductivity, excitability, contractility.
The disease occurs in 4-11% of cases among all cardiovascular diseases. Mostly people aged 30-40 years suffer.
The cause of viral myocarditis is viruses of various origins: Coxsackie, influenza, hepatitis, herpes, ECHO viruses, scarlet fever, sepsis, lupus erythematosus, HIV.
Coxsackievirus is the cause of viral myocarditis in 50% of cases.
The most severe form of viral myocarditis occurs due to infection with diphtheria, scarlet fever, and sepsis. Enterovirus infection poses a significant danger.
Signs of the disease are not always specific, which hinders the correct diagnosis. The acute form of the pathology leads to death in 1-7% of cases of the total number of patients. Sudden death occurs in 17-21% of affected young people.
Causes of myocarditis
The main causes of myocarditis:
Infection and diseases caused by it - viruses (influenza, measles, rubella, chickenpox, Coxsackie B, adenoviruses, arboviruses, cytomegaloviruses, hepatitis B (HBV) and C (HCV), polio, HIV, mononucleosis), bacteria (staphylococci, streptococci, pneumococci, meningococci, gonococci, salmonella, spirochetes, rickettsia, etc.), fungi (candida, actinomycetes, aspergillus, coccidioides), parasites (trichinella), protozoa (toxoplasmosis, trypanosomiasis, schistosomiasis).
The most common infectious diseases that further contribute to the development of myocarditis are influenza, measles, diphtheria, scarlet fever, chickenpox, polio, rubella, acute respiratory infections, pneumonia, Lyme disease, HIV infection, sepsis and others.
Allergic and infectious-allergic causes - when inflammation of the myocardium is promoted by the body's immune response to a particular pathogen or pathological factor. For example, the use of certain medications (antibiotics, sulfonamides, oral contraceptives, vaccines and serums), burns, organ transplantation, certain diseases (rheumatism, vasculitis, bronchial asthma, Lyell's syndrome).
Toxic-allergic causes - the disease develops due to the ingestion or presence of a toxic substance in the body, for example, alcohol, drugs, tobacco smoke, uremia, hyperthyroidism (thyrotoxicosis - the production of an increased amount of hormones by the thyroid gland).
Ideopathic causes , for example, the cause of Abramov-Fiedler myocarditis has not yet been clarified.
Great physical exertion on the body, hypothermia, stress, hypovitaminosis, dehydration and other similar factors increase the possibility of developing myocarditis, or aggravating the course of this disease.
Treatment
Depends on the stage of development of myocarditis and the etiological cause. There is a specific treatment regimen for patients with myocarditis:
- First of all, etiotropic drugs are prescribed, groups of antibacterial or antiviral agents are selected.
- Anti-inflammatory drugs are needed to relieve tissue swelling and improve local blood supply.
- Antihistamines - help reduce the severity of the immune reaction.
- Anticoagulants are mandatory for patients over the age of 50 due to the increased risk of thromboembolism.
Depending on the indications, diuretics, beta-blockers, and ACE inhibitors can be used. The last two groups are indicated if the patient has arrhythmia.
The end of etiotropic therapy does not mean stopping treatment. Most often, it continues due to prescribed antioxidants and vaccination.
The first results of treatment of myocarditis are assessed after six months, for which a number of studies are carried out to determine changes in the concentration of cardioselective enzymes and the autoimmune reaction. Repeated cardiac monitoring using ECG and cardiac ultrasound is important.
Treatment of patients with myocarditis is most often inpatient, after which, if necessary, a conclusion is made about the patient’s professional suitability.
Can myocarditis recur? Yes, and when symptoms of the disease appear, re-treatment with etiotropic drugs is carried out along with metabolic agents.
Types of myocarditis
Myocarditis is classified as follows:
With the flow
- Acute myocarditis with mild or severe course;
- Subacute myocarditis;
- Recurrent myocarditis;
- Latent myocarditis – a course with minimal signs of an inflammatory process;
- Chronic myocarditis - inflammatory and non-inflammatory chronic processes are called cardiomyopathy.
By etiology:
— Infectious myocarditis:
- Viral;
- Bacterial;
- Fungal;
- Parasitic;
- Unspecified;
— Chronic myocarditis (cardiomyopathies) are divided into:
- Specific cardiomyopathies: ischemic, dilated, restrictive, hypertrophic and endocardial fibroblastosis;
- Nonspecific cardiomyopathies: alcoholic, drug, metabolic, external factors, food, infectious or parasitic.
According to the pathogenetic variant:
- Infectious;
- Infectious-toxic;
- Allergic (immunological);
- Infectious-allergic;
- Toxic-allergic.
According to the prevalence of inflammation:
- Focal;
- Diffuse.
According to the nature of the inflammatory process:
- Exudative-proliferative - dystrophic, vascular, inflammatory-infiltrative and mixed;
- Alternative (dystrophic-necrobiotic).
- Pathogenetic phases of infectious myocarditis:
- Infectious-toxic;
- Immunological;
- Dystrophic;
- Myocardiosclerotic.
Stages of development
Acute viral myocarditis develops as a result of one or more pathological processes:
- Direct damage to cardiomyocytes . Viruses, having penetrated a cell, rearrange its genetic structure and lead to the production (replication) of viral bodies. Some of the affected myocytes die, and the remaining ones become autoantigens for the immune system.
- Mobilization of the immune system through multiple defense mechanisms leads to the destruction of infected myocardial cells. In this case, a massive release of toxins and inflammatory mediators occurs. Vessels are damaged, microcirculation is disrupted, and necrosis of cardiomyocytes occurs.
- After two weeks the viruses disappear . Immune damage to the myocardium comes to the fore due to the production of anticardiac antibodies in response to the presence of autoantigens. This marks the transformation of acute myocarditis into an autoimmune disease.
Histology and immunohistology of acute myocarditis (A, B) and chronic myocarditis (C, D).
In acute myocarditis, numerous necrotic myocytes (A, arrows) are associated with mononuclear cell infiltrates, including CD3 + T cells (B), whereas in chronic myocarditis, inflammatory cells such as CD68 + macrophages (D) are mainly present in areas with fibrosis (C, Blue color). (E, F) Radioactive in situ hybridization reveals PVB19 nucleic acid in arteriole endothelial cells from a patient with chronic myocarditis (E), whereas enteroviral ribonucleic acid is detected in several myocytes (F). Thus, the disease is characterized by a sequential change of several stages:
- initial (viremia),
- autoimmune (high period),
- outcome.
Diagnosis of myocarditis
Diagnosis of myocarditis includes:
- History, visual examination of the patient;
- General blood analysis;
- Blood chemistry;
- PCR reaction reaction;
- Electrocardiography (ECG);
- Echocardiography (EchoCG);
- Radiography (X-ray);
- Magnetic resonance therapy (MRI);
- Computed tomography (CT);
- Ultrasound examination (ultrasound);
- Endomyocardial biopsy.
Diagnostics
Viral myocarditis is difficult to diagnose, and errors in its recognition are a common occurrence in everyday practice. Patients come when the infection has already been forgotten, and the observed clinical picture is similar to other heart diseases. It is legitimate to talk about viral myocarditis if the existing cardiac symptoms are confirmed by the following criteria:
- viral infection “the beginning of everything”;
- The ECG reflects repolarization disturbances, deterioration of AV conduction, and unfavorable changes in heart rate;
- the level of cardiac-specific proteins, enzymes and biological markers increased significantly;
- X-ray and echocardiography reveal dilatation and cardiomegaly;
- hypertension and stagnation in the circulatory system;
- characteristic transformation of certain immunological parameters.
The clinical diagnosis must be confirmed by highly sensitive instrumental studies that can detect interstitial edema:
- Endomyocardial biopsy followed by microscopic examination of at least three myocardial samples. The sensitivity of the method is 80%.
- Radioisotope scintigraphy tracking the migration of labeled leukocytes and radiopharmacological drugs into the site of inflammation. The accuracy of the study is 85%.
- Cardiovascular MRI with myocardial contrast. The technique is 75% error-free.
Cardiac magnetic resonance imaging (MRI) of a young patient with acute chest pain syndrome caused by acute myocarditis. Red arrows indicate areas of focal edema of the heart muscle.
Treatment of myocarditis
How to treat myocarditis? Treatment, treatment tactics and the choice of medications used depend on the cause, stage, course and concomitant diseases of the inflammatory process.
Without an accurate diagnosis, it is almost impossible to achieve effective therapy, except for the intervention of the Almighty! Treatment for myocarditis includes:
1. Mode 2. Drug treatment (conservative treatment); 3. Diet 4. Surgical treatment; 5. Prevention of complications of the disease.
Important! If infectious myocarditis is suspected, the patient must be hospitalized, and if the patient’s condition normalizes and there is a stable period of remission without complications for 1-2 weeks, the patient is discharged for further treatment at home.
Mode
Patients with signs of myocardial inflammation need to limit physical activity, and also avoid stress, hypothermia, and unauthorized use of medications.
Bed rest is recommended.
Drug treatment of myocarditis
With minimal signs of myocarditis, specific treatment is usually not advisable.
Thus, treatment of a mild course of the disease usually includes restriction of physical activity, restorative and detoxification therapy. If necessary, the course of treatment can be supplemented with antihistamines.
In the absence of special indications, antibacterial drugs are not used, since in cases of autoimmune and allergic forms of the disease they can cause a number of complications.
Treatment of severe acute myocarditis, accompanied by congestive heart failure, cardiomegaly and severe autoimmune disorders is aimed at treating the underlying disease, treating and preventing arrhythmia, thromboembolic complications, correction of the immune status, immunopathological reactions and hemodynamic disorders.
Important! Before using medications, be sure to consult your doctor!
2.1. Antimicrobial therapy
Upon admission of the patient, a series of tests are immediately taken to determine whether the disease is of an infectious nature, as well as to identify the specific causative agent of myocarditis.
If the infectious nature of the inflammation is established, as well as the type of infection is determined, one or another antimicrobial agent is prescribed.
Read also Mastopathy - symptoms, causes, types and treatment of mastopathy
Before prescribing antimicrobial drugs, it is necessary to normalize metabolism.
Prescribed - "Riboxin", Adenosine triphosphate (ATP), potassium preparations ("Asparkam", "Panangin", "Potassium orotate").
Antiviral drugs for myocarditis are prescribed if the cause of the disease is a virus.
It is worth clarifying that some types of viruses do not imply the use of an antiviral agent, since their treatment consists of stimulating the immune system, restorative therapy, suppressing complications of the disease and treatment with the prevention of arrhythmias and complications.
Antiviral drugs include Viferon, Rimantadine, Acyclovir, Interferon, Anaferon, Ganciclovir, Neovir, and Foscarnet.
Antibiotics for myocarditis - are prescribed if the cause of the disease is bacteria. It is very important to remember that antibiotics do not help fight viral and fungal infections.
Among the antibiotics for myocarditis can be identified - for streptococci (Ampicillin, Gentamicin, Ceftriaxone), staphylococci (Vancomycin, Cefazolin, Oxacillin), pneumococci (Levofloxacin, Cefotaxime), enterococci (“Ampicillin”, “Benzylpenicillin”, “Gentamicin”), Pseudomonas aeruginosa (“Ceftazidime”), rickettsia and chlamydia (“Doxycycline”).
In general, in the acute form of the disease, preference is given to cephalosporins (Cefotaxime, Ceftriaxone, Cefixime). In the chronic form, a second course of antibiotic therapy can be prescribed, only drugs are already used from the groups of fluoroquinolones (Ofloxacin, Ciprofloxacin, Levofloxacin) and macrolides (Erythromycin, Clarithromycin, Roxithromycin).
A repeated course of antibiotics is usually prescribed in combination with antiviral drugs - exogenous interferons, inducers of endogenous interferon, as well as antiviral immunoglobulins.
If necessary, your doctor may prescribe a combination of several antibiotics.
Antifungal drugs are prescribed if fungi are the cause of the disease.
Antifungal drugs for myocarditis include Amikacin, Meropenem, Amphotericin B, and Flucytosine.
When the patient’s condition returns to normal, stable remission without complications is observed, the ESR is normalized, and tests for infectious microflora are normal, the course of antimicrobial therapy is stopped.
2.2. Anti-inflammatory therapy
To relieve inflammation in the myocardium, anti-inflammatory drugs from the NSAID group are used (for a short course - Diclofenac, Metindol), antihistamines (Suprastin, Tavegil), and long-term use of the drug Delagil.
If an autoimmune factor predominates in myocardial inflammation, the patient is prescribed steroid hormones - Dexamethasone, Prednisolone.
After anti-inflammatory therapy, the person’s health usually improves, the heart rate stabilizes, and swelling is relieved.
However, it is worth remembering that the use of hormones can cause a number of complications, which the attending physician must remember and monitor the patient’s condition.
2.3. Normalization of blood circulation
Many heart diseases are accompanied by impaired blood circulation. In this regard, patients with myocarditis are also prescribed several groups of different drugs, united by one name - disaggregants, or antiplatelet drugs.
Antiplatelet drugs are drugs that, by thinning the blood, improve blood circulation, prevent the formation of blood clots, reduce the processes of gluing and sticking (adhesion) of platelets with red blood cells to the vascular endothelium (the inner wall of blood vessels), prevent the development of coronary heart disease (CHD) and the occurrence of myocardial infarction .
Antiplatelet agents include Aspirin-Cardio, Alprostadil, Clopidogrel, Trental, Pentoxifylline, Cardioxipine.
Angiotensin-converting enzyme (ACE) inhibitors prevent the conversion of inactive angiotensin I to angiotensin II and then to renin, which cause vasoconstriction. In addition, ACE inhibitors slow down the process of replacement of myocardial tissue with fibrin, lower blood pressure, and reduce proteinuria.
Among the ACE inhibitors are Captopril, Epsitron, Potensin, Lisinopril, Enalapril, Prestarium, Amprilan.
Beta blockers - block beta receptors involved in the release of angiotensin II and renin, which cause constriction of blood vessels. This reduces the risk of developing heart failure. This group of drugs is used in monotherapy for no more than a month, after which it is combined with diuretics and calcium channel blockers.
Among the beta-blockers we can highlight: Atenolol, Bisoprolol, Cordinorm, Metoprolol, Vasocardin, Carvenal, Recardium.
2.4. Detoxification therapy
Detoxification therapy is aimed at removing from the body toxic substances - waste products of infection, as well as the pathogens themselves, which died when exposed to antiviral, antibacterial, antifungal and other drugs used depending on the identified pathogen.
Detoxification therapy includes:
- Drink plenty of water (only outside the acute stage of the disease) - at least 1.5-2 liters of water per day;
- The use of detoxification drugs – “Atoxil”, “Albumin”.
- In difficult situations, plasma transfusion and hemosorption may be prescribed.
It is also advisable to prescribe aldosterone antagonists, which, by blocking aldosterone receptors, help remove metabolic products of chlorine, sodium, water from the body, as well as reduce the leaching of potassium and urea in the kidneys. Other beneficial properties of aldosterone antagonists are diuretic and antihypertensive.
Among the aldosterone antagonists we can highlight Veroshpiron and Aldactone.
2.5. Symptomatic therapy
To normalize the functioning of the immune system, immunocorrective therapy is prescribed, which includes plasmapheresis, pulse therapy of interferon inducers and glucocorticoids.
To normalize heart function, relieve arrhythmia and prevent the development of heart failure, cardiac glycosides - herbal medicines - are prescribed. However, it is not recommended to use them yourself, since an incorrectly calculated dosage can be harmful to health, because the drugs are based on plant poisons for the body.
Read also: Catarrhal tonsillitis - symptoms and treatment
Cardiac glycosides can be distinguished - “Adonizide”, “Cordigitit”, “Korglykon”, “Celanid”, “Digoxin”, tincture of lily of the valley, infusion of the herb adonis.
To relieve swelling, diuretics (diuretics) are used, which increase the rate of removal of fluid from body tissues - Furosemide, Dichlorothiazide, Diacarb.
For persistent high body temperature, anti-inflammatory drugs are prescribed - Paracetamol, Nimesil, Ibuprofen.
An elevated temperature (up to 38.5 °C) is not brought down, since this is the body’s immune response to an infection - an elevated temperature actually “burns out” the infection, especially in the case of a viral nature of the disease.
Diet for myocarditis
Diet for myocarditis is an integral part of the treatment of myocardial inflammation.
So, in the diet it is necessary to limit the consumption of table salt.
In addition, the consumption of hot, spicy, salty, smoked, fatty and fried foods, and instant foods is prohibited.
For diseases of the cardiovascular system, therapeutic nutrition developed by M.I. Pevzner is usually used - diet No. 10 and 10a.
You need to focus on eating food that contains vitamins and protein.
The goal of the diet is to reduce the load on the heart and prevent the deposition of atherosclerotic plaques (atherosclerosis) on the walls of blood vessels.
Surgery
Surgical treatment of myocarditis is used if a danger to human life is identified, as well as a number of complications of the disease.
Indications for the operation are:
- Lack of positive results from drug treatment;
- Increasing symptoms despite conservative treatment methods;
- The appearance of signs of heart failure;
- The appearance of pus in the heart area.
To gain access for heart surgery, an opening of the chest (thoractomy) is performed.
Features of diagnosis and treatment of infectious myocarditis
Myocarditis is an inflammatory process that occurs in the lining of the heart muscle. Often the disease is rheumatic, infectious or allergic in nature. The disease occurs in both acute and chronic forms. The first is accompanied by shortness of breath, swelling in the lower extremities, enlarged veins in the neck and other symptoms. In the second, the signs are not so pronounced.
Often, infectious myocarditis develops after a sore throat, acute respiratory viral infection, diphtheria and other infections. In the absence of correct and timely treatment, complications and relapse may develop in adults and children.
This article will describe the symptoms of the disease in children and the older generation, the qualifications of the disease, its treatment and preventive methods. The reader will also receive information about the prognosis for myocarditis.
As you read, questions may arise - please address them via the online form to the portal specialists.
Consultations are provided free of charge around the clock.
general information
Myocarditis is a common disease, which, due to late diagnosis, can occur in either a mild or acute form. Signs of the disease are detected in almost 10% by a pathologist. According to statistics, up to 7% of patients die from this disease annually, and in 20% of people of working age the disease causes sudden death.
Against the background of myocarditis, cardiac organ failure develops, rhythm disturbances and, as a result, death. The disease most often affects people under 40 years of age, however, it can develop at any age - even in children. Regarding gender, myocarditis is diagnosed more often in women, but the male population is susceptible to severe forms of the disease.
Causal relationship
Myocarditis is included in the list of diseases that develop against the background of an inflammatory process in the heart muscle, which affects the functionality of the myocardium.
The most common causes of the disease are (see figure below):
- viral infectious diseases;
- bacteria;
- fungus;
- parasites.
Main causes of myocarditis
A severe type of myocarditis develops against the background of diphtheria, sepsis, and more. The disease is also provoked by various cardiotropic viruses, chronic diseases in connective tissues and allergies. You should not ignore the effects of toxins on the body, which include medications, alcohol-containing drinks and ion radiation.
The disease is often accompanied by endocarditis and pericarditis. In rare cases, inflammation develops only in the myocardium.
The provoking factor is:
- chronic foci of infectious diseases;
- underdeveloped immune system;
- abuse of alcoholic beverages, drugs and toxins.
When the immune system fails, myocarditis affects all levels from cellular to phagocytosis. Bacteria provoke damage that changes the composition of muscle fibers and leads to the development of exudative reactions.
Due to the impact of the disease on the body, the connective tissue grows, which leads to cardiosclerosis.
It is worth noting that with myocarditis, the pumping function of the heart decreases and in frequent cases this process is irreversible.
Conclusion: if the disease is not treated, insufficiency in the blood supply, disruption of the heart rhythm, poor conductivity and death may occur. In 90%, patients with this diagnosis receive a disability group.
Types and stages of development of myocarditis
The classification of the disease directly depends on the causes of its occurrence. In cardiology, the disease is divided into the following subtypes:
- infectious;
- infectious-toxic;
- infectious allergic myocarditis;
- allergic-toxic;
- idiopathic.
Myocarditis develops sequentially in four stages:
- toxic-infectious;
- immune;
- dystrophy;
- myocardial sclerosis.
The disease is also divided according to symptoms:
- low manifestation of signs of illness;
- pain syndrome;
- disruption of the blood supply to the heart muscle;
- arrhythmia;
- thrombus formation;
- pseudovalvular symptom;
- manifestation of symptoms in a complex.
The disease is distinguished by its prevalence, i.e. foci or diffuse course. It can occur in acute, subacute, chronic form. The degree of severity is not the least important in the classification of myocarditis. There are light, medium and severe forms.
Symptomatic picture
The first symptoms make themselves felt already in the first week of the disease. However, these signs are not specific and are often attributed to other diseases.
- cardiopalmus;
- high fatigue during normal daily routine;
- intense sweating;
- pain in the sternum;
- dyspnea;
- joint pain;
- the skin turns pale;
- febrile conditions.
As myocarditis develops in adults, symptoms such as:
- insomnia;
- nervous overexcitation;
- change of mood;
- tearfulness.
Further, the disease manifests itself in severe pain that does not depend on physical activity or exertion. It is becoming increasingly difficult to ignore irregularities in the heart rhythm, and tachycardia becomes a life companion. In the final stages of myocarditis, decompensation of the left chamber ventricle occurs.
Infectious-allergic form of the disease
Infectious allergic myocarditis is most often diagnosed in children and able-bodied individuals under 40 years of age. Many cardiologists believe that the idiopathic form of myocarditis according to Abramov-Fidper is highly dangerous. This is due to the fact that this type occurs not only in connective tissues, but also in the lining of the heart organ.
Infectious allergic myocarditis has the following symptoms:
- general malaise of the body;
- pain in muscles and joints;
- dull, aching and squeezing pain in the chest cavity;
- dyspnea;
- cardiopalmus.
Myocarditis also has variable symptoms, which manifest themselves in arrhythmia, bracardia, hypotension, conduction failure and other symptoms.
There are no symptoms of heart failure in this type of myocarditis.
On average, in a third of patients, the disease is asymptomatic or has mild symptoms. The disease can only be diagnosed using modern medical equipment.
Signs of myocarditis in children
The infectious type of myocarditis in pediatric cardiology is divided into two groups:
- congenital form of the disease;
- acquired.
The first group in children develops during childbirth, because a child is born with a pathologically enlarged heart. The first symptoms begin to linger for about six months and are as follows:
- pale skin;
- the child’s health is sluggish;
- fatigue;
- poor weight gain;
- tachycardia.
The acquired disease in children has several forms, which occur in different ways: acute, subacute and chronic. Before the age of three, children are more often diagnosed with viral, bacterial or fungal myocarditis. As an adult, the child may suffer from an infectious allergic type.
The acute form of the disease is the consequences of previous colds. If a child develops symptoms such as insomnia, night sickness, shortness of breath, bluish skin color, nausea, systematic loss of consciousness and cold hands and feet, it is recommended to urgently visit a cardiologist’s office.
If the disease is not treated in a timely manner, it takes on an advanced form. The consequences of this attitude to the child’s health are a “hump” on the heart, in which a bulge forms in the sternum, which is diagnosed with the naked eye.
The subacute and chronic type of the disease in children most often develops less noticeably, and the first symptoms may appear after several years. Lack of proper treatment - early disability, dysfunction of the pumping activity of the heart organ and disruption of blood circulation.
Due to the high danger for children and adults, cardiologists advise undergoing an annual preventive examination. This will allow us to identify the disease at an early stage and develop the correct treatment strategy.
Diagnostic methods
There is one problem in diagnosing this disease – the absence of symptoms at the primary stage. Therefore, to confirm or refute the diagnosis, a number of examinations are carried out:
- An ECG, as a non-invasive test, can reveal a malfunction in the functionality of the heart.
- Echocardiography is carried out using ultrasound radiation. Due to this type of diagnosis, it is possible to identify thrombus formations inside cavities.
- A chest x-ray looks for congestion in the lung airways and may reveal an enlarged heart.
- An isotope test allows you to visually assess lesions.
- A biopsy is necessary to study DDC.
- A blood draw can detect the presence of viruses.
- A complete blood test is performed to study the immune system.
- MRI;
- Examination of the cavities of the heart organ with a probe.
Treatment for patients with primary (mild) form of myocarditis is carried out on an outpatient basis. Hospitalization is necessary for moderate and advanced forms of the disease.
Treatment methods
Myocarditis is treated in two ways - therapeutic and medicinal. Let's consider both directions in detail.
Therapy
The therapeutic method is universal. The development of an individual strategy in therapy is not provided. Therefore, the doctor treats the inflammatory process and eliminates its foci.
The doctor's main instructions are:
- reduce the amount of salt you consume;
- refusal to drink alcoholic beverages;
- a complete diet;
- decreased physical activity;
- quitting tobacco.
Bed rest is also a positive factor in therapy. Oxygen inhalation procedures are prescribed depending on the form of the disease.
Medicines
Three options for drug therapy are prescribed:
- antihistamines;
- non-steroidal anti-inflammatory drugs;
- medications of the immunosuppressive group.
In severe cases of myocarditis, hormones of the glucocorticoid category are prescribed. Medicines such as Voltaren, Indomethacin, Prednisolone and others are often used.
To improve metabolism in the myocardium, potassium-based medications are prescribed (Asparkam, vitamins, Riboxin, etc.). Anticoagulants for preventive purposes - have a positive effect in the fight against the disease.
The duration of treatment is about six months.
Preventive measures and prognosis
The inflammatory process in the myocardium is often a consequence of infectious diseases or allergies. In view of this, the main methods of prevention are to prevent the diseases described above and treat them in a timely manner for both adults and children.
Modern medicine has developed a number of vaccines aimed at preventing diseases such as measles, rubella, influenza, fungal diseases and more. Increased importance in cardiology is given to the prevention of inflammation of the maxillary sinuses, caries and tonsillitis.
If there are blood relatives in the family who suffer from myocarditis, the remaining family members must be examined every year by a cardiologist using ECG diagnostics.
As for forecasts, it depends on many circumstances. For example: general health, reasons for the development of the disease, timely contact with doctors. On average, 50% of patients are successfully cured of the disease without complications.
In the rest, myocarditis is severe, often developing relapses and complications in the form of heart failure.
It should be understood that in severe form, this disease can lead to surgery, and in some cases, replacement of the heart organ is necessary.
Source: https://cardiologiya.com/bolezni/miokard/infekcionnyj-miokardit.html
Treatment of myocarditis with folk remedies
Important!
Before using folk remedies against myocarditis, be sure to consult your doctor! Rose hip. Pour 500 ml of boiling water over a handful of fresh rosehip flowers, leave the product for 16 minutes, strain and take 1 tbsp. spoon of infusion 3 times a day, 30 minutes before meals. The course of treatment is 1 month.
To prepare another recipe, you need 1 tbsp. pour a spoonful of chopped rosehip root into 1 cup of boiling water, put on low heat and boil for 5 minutes. Strain and drink semi-hot as tea, 3 glasses per day for 2 weeks.
Hawthorn. 1 tbsp. Pour a glass of boiling water over a spoonful of dried hawthorn fruits, let the product brew for 2 hours, then strain and take 2 tbsp. spoons of the product 3-4 times a day, 15 minutes before meals.
Honey. Consume 1 teaspoon daily, 2-3 times a day, of flower honey, adding milk, cottage cheese and fruit to it. It is not recommended to drink honey with tea.
Symptoms
Viral myocarditis has no characteristic symptoms. The clinic is diverse and corresponds to disorders of the cardiovascular system. At the onset of the disease there is acute intoxication. Hyperthermia, joint and muscle pain, weakness, gastrointestinal disorders, and mild shortness of breath occur. Then cardiac disorders come to the fore:
- prolonged chest pain not associated with exercise and not relieved by taking nitroglycerin;
- shortness of breath, weakness, feeling tired from light work;
- rhythm disturbances: tachycardia, arrhythmias, extrasystoles, ventricular fibrillation;
- decreased systolic and increased diastolic blood pressure, circulatory failure, the appearance of edema, fainting.
Symptoms range from mild malaise to severe cardiac pathology. Hemodynamics suffer from a decrease in left ventricular cardiac output. As the atrioventricular and sinus nodes become involved in the pathological process, AV blockades, arrhythmias, and extrasystoles begin to disturb. The division of myocarditis by severity is based on polymorphism and the scale of pathological processes.
| Severity | Short description |
| Lightweight | There are no functional disorders of the heart or an increase in its size. Conduction and heart rate are normal. |
| Medium-heavy | X-ray reveals an enlarged heart. Echocardiography shows the presence of functional failure of the left ventricle. There is a threat of 1st degree AV block and blockade of one of the branches of the His bundle. |
| Heavy | Cardiovascular failure increases, which can be complicated by the development of cardiogenic shock. The ECG shows signs of focal changes in the myocardium, 2-3 degree AV block and blockade of two or three branches of the His bundle. Severe extrasystoles with fainting are observed. The phenomena of stagnation in both circles of blood circulation are pronounced. |
Manifestations in children
Viral myocarditis in children is characterized by rapid development. The first manifestations may be gastrointestinal disorders, hyperthermia, central nervous system depression with
restless sleep and increased fatigue.
With intrauterine infection, children appear with congenital viral myocarditis. These newborns are different:
- pale gray tint of the skin;
- weak cry, lethargy;
- fatigue during feeding and poor weight gain;
- the presence of facial edema.
Prevention of myocarditis
Prevention of myocarditis includes:
- Eating mainly foods enriched with vitamins and microelements, as well as avoiding unhealthy foods;
- Timely seeking help from a doctor for heart pain, as well as timely treatment of various diseases so that they do not become chronic;
- Compliance with the rules for the prevention of acute respiratory diseases (ARI);
- Avoiding hypothermia;
- Avoiding stress;
- Use medications only after consulting a doctor, especially antibiotics.
Viral myocarditis: treatment of the disease
Although the cause of infectious myocarditis can be identified, etiological therapy is rarely used. This is explained by the fact that the pathogen has penetrated the cells and damage to the heart has already occurred. Therefore, treatment of viral myocarditis is aimed at the pathogenesis of the disease. To improve the patient's condition and stop the development of pathology, non-steroidal anti-inflammatory drugs are prescribed. Among them are the medications Indomethacin and Diclofenac. They not only eliminate inflammation, but are also pain relievers. As the disease progresses, small doses of hormones are used. These include the drug Prednisolone.
Treatment of chronic viral myocarditis is aimed at combating heart failure. For this purpose, cardioprotectors are prescribed, for example the drug Preductal. Vitamins for the heart and antiplatelet agents are also needed. For edema syndrome, the use of diuretics is indicated. Severe rhythm disturbances require the installation of a pacemaker.