© Author: Ilya Vitalievich Soldatenkov, general practitioner, especially for SosudInfo.ru (about the authors)
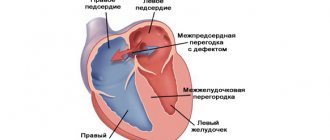
Ventricular septal defect (VSD) is a fairly common pathology, which is an intracardiac anomaly with a hole in the wall separating the ventricles of the heart.
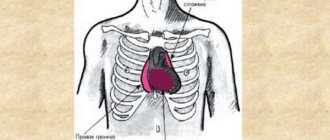
picture: ventricular septal defect (VSD)
Small defects practically do not cause complaints from patients and heal on their own with age. If there is a large hole in the myocardium, surgical correction is performed. Patients complain of frequent pneumonia, colds, and severe shortness of breath.
General information
This condition results in abnormal mixing (shunting) of blood. In cardiological practice, such a defect is the most common congenital heart pathology. Critical conditions with VSD develop with a frequency of twenty-one percent. Both male and female children are equally susceptible to this defect.
VSD in the fetus can be isolated (that is, the only existing anomaly in the body) or part of complex defects (atresia of the tricuspid valve, transposition of vessels, common arterial trunks, tetralogy of Fallot).
In some cases, the interventricular septum is completely absent; this defect is called a single ventricle of the heart.
Prognosis and quality of life
The operation is successful in 98-99% of cases.
The prognosis for recovery is favorable. The quality and life expectancy are unchanged. Patients are under the supervision of a surgeon and cardiologist until complete recovery, and after discharge they are subject to lifelong dispensary registration . There are no restrictions on diet or work, physical activity is selected individually.
Ventricular septal aneurysm is a rare anomaly that can be isolated or combined with other heart defects. Symptoms may be absent for a long time or for life. Pathology rarely affects the well-being and development of the child. When a diagnosis is made, the patient must register with a cardiologist and undergo dynamic monitoring. The treatment regimen and indications for surgery are determined individually in each case.
VSD Clinic
Symptoms of a ventricular septal defect often appear in the first days or months after the baby is born.
The most common manifestations of the defect include:
- shortness of breath;
- cyanosis of the skin (especially fingertips and lips);
- decreased appetite;
- cardiopalmus;
- fatigue;
- swelling in the abdomen, feet and legs.
VSD may be asymptomatic at birth if the defect is small enough, and appear only at a later date (six years or more). Symptoms directly depend on the size of the defect (hole), however, the doctor should be alert to noises heard during auscultation.
Ultrasound of the heart in infants
Ultrasound examination is not mandatory. In infants, indications for diagnosis include changes in the organ in question during intrauterine examination, transformation on an ECG, and noise during a heartbeat scan detected during auscultation. In the first case, the baby is examined immediately in the maternity hospital. In other situations, an ultrasound scan is performed on the child when abnormalities are detected.
There is no question about how often children can be diagnosed, since the ultrasound method does not cause harm at any age. But despite the absence of restrictions, ultrasound, like every examination of a child, must be justified.
VSD in the fetus: causes
Any congenital heart defects appear due to disturbances in the development of the organ in the early stages of embryogenesis. An important role in this case belongs to external environmental and genetic factors.
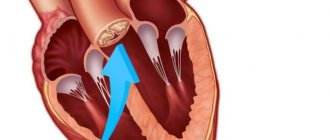
With VSD in the fetus, an opening is determined between the left and right ventricles. The muscle layer of the left ventricle is more developed than in the right, and therefore oxygen-rich blood from the cavity of the left ventricle penetrates into the right and mixes with oxygen-depleted blood. As a result, less oxygen reaches organs and tissues, which ultimately leads to chronic oxygen starvation of the body (hypoxia). In turn, the presence of additional blood volume in the right ventricle entails its dilatation (expansion), myocardial hypertrophy and, as a consequence, the occurrence of cardiac right ventricular failure and pulmonary hypertension.
Heart pathology
Minor anomalies in the development of this organ are architectural disorders that do not lead to functional and hemodynamic problems.
Patent foramen ovale (PFO) is a common finding in infants. This fetal communication is completed by one year, and sometimes later. The recorded blood discharge during CDK is small and, as a rule, insignificant for hemodynamics. However, many heart defects are accompanied by PFO.
It is also necessary to differentiate PFO from an atrial septal defect, which causes changes in hemodynamics. In case of ASD, diagnostic criteria are overload of the right parts (atrium enlargement), distortion of the septum in B-mode in at least two positions in the area of secondary location, discharge of blood during color circulation through the defect.
Atrial septal defect
Abnormally located chords and trabeculae of the left ventricle (LVARCH) are the most common MAS, which becomes the main cause of systolic murmur and the appointment of cardiac ultrasound performed at 1 month of age in a child. The examination reveals hyperechoic linear formations connecting the walls of the left ventricle.
Prolapse of the mitral valve leaflets (MVP) is their sagging into the left atrium. This type of MAS is practically not detected in one-year-old children, but appears closer to puberty.
Risk factors
The exact causes of VSD in the fetus are unknown, but an important factor is family history (that is, the presence of a similar defect in close relatives).
In addition, factors that are present during pregnancy also play a huge role:
- Rubella. It is a viral disease. If during a real pregnancy (especially in the first trimester) a woman has suffered from rubella, then the risk of various anomalies of internal organs (including VSD) in the fetus is very high.
- Alcohol and some drugs. Taking such drugs and alcohol (especially in the first weeks of pregnancy) significantly increases the risk of developing various abnormalities in the fetus.
- Inadequate treatment of diabetes mellitus. Uncorrected glucose levels in a pregnant woman lead to fetal hyperglycemia, which can ultimately lead to a variety of congenital anomalies.
Classification
There are several options for the location of the VSD:
- Conoventricular, membranous, perimembranous VSD in the fetus. It is the most common location of the defect and accounts for approximately eighty percent of all such defects. A defect is detected on the membranous part of the septum between the ventricles with probable spread to the outlet, septal and inlet sections; under the aortic valve and the tricuspid valve (its septal leaflet). Quite often, aneurysms occur in the membranous part of the septum, which subsequently leads to closure (complete or partial) of the defect.
- Trabecular, muscular VSD in the fetus. It is found in 15-20% of all such cases. The defect is completely surrounded by muscles and can be located in any part of the muscular part of the septum between the ventricles. Several such pathological holes can be observed. Most often, such VSDs in the fetus close spontaneously spontaneously.
- Subpulmonary, subarterial, infundibular, and crestal openings of the outflow tract account for approximately 5% of all such cases. The defect is localized under the valves (semilunar) of the outlet or cone-shaped sections of the septum. Quite often, this VSD due to prolapse of the right aortic valve leaflet is combined with aortic insufficiency;
- Defects in the area of the afferent tract. The hole is located in the area of the inlet septum, directly under the area of attachment of the ventricular-atrial valves. Most often, the pathology accompanies Down syndrome.
Most often single defects are found, but multiple defects in the septum are also found. VSD can be involved in combined cardiac defects, such as tetralogy of Fallot, transposition of the vessels and others.
According to size, the following defects are distinguished:
- small (symptoms are not expressed);
- average (the clinic appears in the first months after childbirth);
- large (usually decompensated, with vivid symptoms, severe course and complications, which can lead to death).
Clinical manifestations of asynergia and methods for its diagnosis
The human brain is a complex structure, consisting of different sections that are interconnected anatomically and functionally and are responsible for performing certain types of activities in the human body.
One of the most important parts of the brain, in particular its posterior part, is the cerebellum.
It is responsible for the coordination of movements, regulates muscle tone, without it it is impossible to ensure normal balance of the human body in space.
In addition, the involvement of the cerebellum in mental functions has been proven. That is why pathology in this part of the brain attracts the attention of not only neurologists, but also psychiatrists.
What happens when the cerebellum is damaged?
For various reasons (tumor, trauma, abscess, hemorrhage, hereditary degenerative diseases, demyelinating diseases, alcoholic degeneration), the cerebellum ceases to function normally, which is manifested by various symptoms of movement disorders.
The most important of them are atony (or hypotension), ataxia and its manifestation asynergy. The latter is expressed in a person’s inability to symmetrically make complex movements, to perform actions that require the simultaneous participation of different parts of the body, that is, each movement will be performed as a sequence of individual simple reactions, and not as a whole combination.
There are static ataxia (inability to maintain balance in an upright position of the body) and dynamic (discoordination disorders when walking, unsteady gait with legs set wide apart). All three of the above symptoms appear when any part of the cerebellum is damaged, but their severity depends on the location of the pathological focus and its size.
In addition, characteristic manifestations of cerebellar disorders are:
- the appearance of tremor and nystagmus;
- hypermetry (inconsistency of movements with the distance to a certain point, for example, a sick person misses further than the nose during a finger-nose test);
- speech disorders;
- adiadochokinesis (impossibility of correct alternation with opposite actions).
Clinical manifestations of asynergia
This pathology was described by the French scientist Babinsky, according to his ideas there are:
- frontal asynergia (with pathology of the corresponding lobes of the brain) - disturbances when walking are manifested by the fact that the legs lag behind the body, which gradually leans back, and the person falls on his back due to a shift in the center of gravity of the body;
- cerebellar type 1 - a person experiences difficulty when trying to get up from a horizontal position without the help of hands (with arms crossed on the chest), due to the lack of symmetrical contraction of the muscles of the buttocks, the pelvis and legs are not pressed against the support, but rise upward when standing up. Cases of unilateral violation - hemiasynergy - have been described.
- cerebellar asynergia type 2 - pathology of the cerebellar vermis - the patient, when throwing his head back and trying to bend, falls, losing balance, on his back, since there is no symmetrical muscle contraction and flexion of the legs at the knees and extension at the hip joints.
It should be noted that the rapidly growing clinical picture of ataxia and asynergia is characteristic of acute situations (cerebral hemorrhage, cerebellar infarction), and a rapidly developing symptom complex with a tumor, brain abscess, and alcoholism.
Episodic manifestations of incoordination may occur when certain medications (anticonvulsants) enter the body or with hereditary pathology. Ataxia and asynergia slowly progress in idiopathic lesions and degenerative forms of diseases, multiple sclerosis.
Complications of VSD
If the size of the defect is small, clinical manifestations may not occur at all, or the holes may spontaneously close immediately after birth.
For larger defects, the following serious complications may occur:
- Eisenmenger syndrome. Characterized by the development of irreversible changes in the lungs as a result of pulmonary hypertension. This complication can develop in both young and older children. In this condition, part of the blood moves from the right to the left ventricle through a hole in the septum, because due to hypertrophy of the myocardium of the right ventricle, it turns out to be “stronger” than the left. Therefore, oxygen-depleted blood reaches the organs and tissues, and, as a result, chronic hypoxia develops, manifested by a bluish tint (cyanosis) of the nail phalanges, lips and skin in general.
- Heart failure.
- Endocarditis.
- Stroke. It can develop with large septal defects due to turbulent blood flow. Blood clots may form, which can subsequently clog the blood vessels of the brain.
- Other heart pathologies. Arrhythmias and valve pathologies may occur.
Symptoms of blocked meibomian glands
The complicated form of the disease has characteristic symptoms that are most often observed in childhood. In adults, the symptoms are slightly blurred. Meibomian gland dysfunction is characterized by:
- redness;
- edema;
- painful movement of the eyelids;
- feeling of particles getting into the eyes;
- burning and heat;
- increased tearfulness.
As a result of the development of the disease, yellow crusts appear between the eyelashes and in the corners of the eyes. There is pain when touching the eyelids. When you carefully turn the eyelid inside out, you can find a yellow abscess, which is located on the cartilaginous tissue.
This abscess matures within several days and, when opened, exits through the cartilage of the eyelid or the main excretory duct of the inflamed gland. A small retracted scar appears at the site of the breakthrough. If the purulent formation matures for a long time, surgery may be necessary.
VSD in the fetus: what to do?
Most often, such heart defects are detected during a second routine ultrasound. However, there is no need to panic.
- You need to lead a normal life and not be nervous.
- The attending physician should carefully monitor the pregnant woman.
- If the defect is detected during the second planned ultrasound, the doctor will recommend waiting for the third examination (at 30-34 weeks).
- If a defect is detected on the third ultrasound, another examination is prescribed before birth.
- Small (for example, VSD 1 mm in the fetus) openings can close spontaneously before or after birth.
- Consultation with a neonatologist and fetal ECHO may be required.
Diagnostics
The presence of a defect can be suspected by auscultation of the heart and examination of the child. However, in most cases, parents learn about the presence of such a defect even before the baby is born, during routine ultrasound examinations. Quite large defects (for example, a 4 mm VSD in a fetus) are usually detected in the second or third trimester. Small ones can be detected after birth by chance or when clinical symptoms appear.
A diagnosis of VSD in a newborn or older child or adult can be made based on:
- Patient's complaints. This pathology is accompanied by shortness of breath, weakness, heart pain, and pale skin.
- History of the disease (time of appearance of the first symptoms and their relationship with stress).
- Life history (complicated heredity, maternal illnesses during pregnancy, and so on).
- General examination (weight, height, age-appropriate development, skin tone, etc.).
- Auscultation (murmurs) and percussion (expansion of the boundaries of the heart).
- Blood and urine examination.
- ECG data (signs of ventricular hypertrophy, conduction and rhythm disturbances).
- X-ray examination (changed shape of the heart).
- Vetriculography and angiography.
- EchoCG (i.e. ultrasound of the heart). This study makes it possible to determine the location and size of the defect, and with Doppler measurements (which can be carried out in the prenatal period) - the volume and direction of blood through the hole (even if the congenital heart disease - VSD in the fetus is 2 mm in diameter).
- Catheterization of the cardiac cavities. That is, inserting a catheter and using it to determine the pressure in the vessels and cavities of the heart. According to the data, a decision is made on further tactics of patient management.
- MRI. Prescribed in cases where Echo CG is uninformative.
Symptoms
cyanosis is a symptom characteristic of all “blue” heart defects
A VSD does not cause problems to the fetus and does not interfere with its development. The first symptoms of the pathology appear after the birth of the child: acrocyanosis, lack of appetite, shortness of breath, weakness, swelling of the abdomen and limbs, tachycardia, slow psychophysical development.
Children with signs of VSD often develop severe forms of pneumonia that are difficult to treat. A doctor, examining and examining a sick child, discovers an enlarged heart, systolic murmur, and hepatosplenomegaly.
- If there is a small VSD, the development of children does not change significantly . There are no complaints, shortness of breath and slight fatigue occur only after physical activity. The main symptoms of the pathology are systolic murmur, which is found in newborns, spreads in both directions and is clearly audible on the back. For a long time it remains the only symptom of the pathology. In more rare cases, you may feel a slight vibration or trembling when you place your palm on your chest. In this case, there are no symptoms of heart failure.
- A pronounced defect manifests itself acutely in children from the first days of life . Children are born with malnutrition. They eat poorly, become restless, pale, develop hyperhidrosis, cyanosis, and shortness of breath, first while eating and then at rest. Over time, breathing becomes rapid and difficult, a paroxysmal cough appears, and a heart hump forms. Moist wheezing appears in the lungs, the liver enlarges. Older children complain of palpitations and cardialgia, shortness of breath, frequent nosebleeds and fainting. They are significantly behind their peers in development.
If a child gets tired quickly, cries often, eats poorly, refuses to breastfeed, does not gain weight, has shortness of breath and cyanosis, you should consult a doctor as soon as possible. If shortness of breath and swelling of the extremities occur suddenly, and the heartbeat becomes fast and irregular, an ambulance should be called.
Stages of disease development:
- The first stage of the pathology is manifested by an increase in the size of the heart and stagnation of blood in the pulmonary vessels. In the absence of adequate and timely therapy, pulmonary edema or pneumonia may develop.
- The second stage of the disease is characterized by spasm of the pulmonary and coronary vessels in response to their overstretching.
- In the absence of timely treatment for congenital heart disease, irreversible sclerosis develops in the pulmonary vessels. At this stage of the disease, the main pathological signs appear, and cardiac surgeons refuse to perform the operation.
disorders with VSD
Downstream, there are 2 types of VSD:
- An asymptomatic course is detected by noise . It is characterized by an increase in the size of the heart and an increase in the pulmonary component of the 2nd tone. These signs indicate the presence of a small VSD. Medical supervision is required for 1 year. If the noise disappears and there are no other symptoms, spontaneous closure of the defect occurs. If the noise remains, long-term observation and consultation with a cardiologist are required, and surgery is possible. Small defects occur in 5% of newborns and close on their own by 12 months.
- A large VSD is symptomatic and manifests itself with signs of heart failure . Echocardiography data indicate the presence or absence of associated defects. Conservative treatment in some cases gives satisfactory results. If drug therapy is ineffective, surgery is indicated.
Treatment
When a VSD is detected in the fetus, a wait-and-see approach is followed, since the defect can spontaneously close before birth or immediately after birth. Subsequently, if the diagnosis is maintained, such a patient is managed by cardiologists.
If the defect does not interfere with the patient’s blood circulation and general condition, he is simply monitored. In case of large holes that interfere with the quality of life, a decision is made to perform surgery.
Surgical interventions for VSD can be of two types: palliative (restriction of pulmonary blood flow in the presence of combined defects) and radical (complete closure of the opening).
Operation methods:
- On an open heart (for example, with tetralogy of Fallot).
- Cardiac catheterization with controlled application of a patch to the defect.
Prevention of ventricular septal defect
There are no specific preventive measures for VSD in the fetus, however, in order to prevent congenital heart disease, it is necessary:
- Contact an antenatal clinic before twelve weeks of pregnancy.
- Visit the residential complex regularly: once a month for the first three months, once every three weeks in the second trimester, and then once every ten days in the third.
- Follow a routine and adhere to proper nutrition.
- Limit the influence of harmful factors.
- Avoid smoking and alcohol.
- Take medications strictly as prescribed by your doctor.
- Get vaccinated against rubella at least six months before your planned pregnancy.
- If there is a family history, carefully monitor the fetus for the earliest possible detection of congenital heart disease.