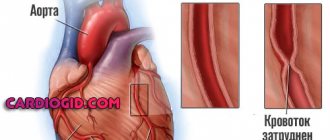
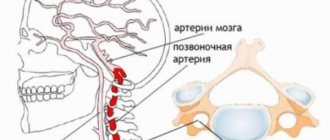
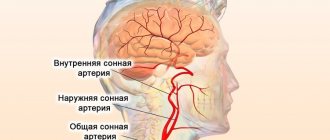
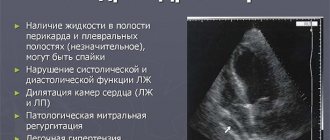
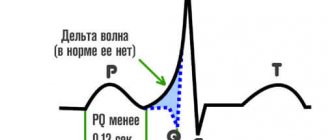
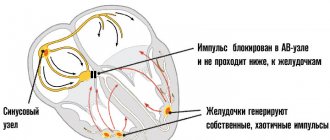
Leriche syndrome is a complex of clinical manifestations caused by narrowing or occlusion of the abdominal aorta at the site of its bifurcation, which leads to erectile dysfunction, cyanosis of the legs and other painful symptoms.
It is well known that the aorta is the largest blood artery. Approximately at the level of the navel, it bifurcates and goes through the small pelvis into the limbs. But if for one reason or another the diameter of the aorta or both iliac arteries decreases, this can lead to oxygen starvation. The conditional “affected area” is the organs of the genitourinary and reproductive systems, as well as the upper legs.
Such conditions in medicine are called aortoiliac occlusions, and the term itself - Leriche syndrome - has many synonyms (chronic obstruction of the aorta, atherosclerotic thrombosis of the abdominal aorta). The pathology has been known to medicine for quite some time, but it received its current name in honor of the French surgeon Rene Leriche (1879-1955), who in 1940 performed the world's first resection and lumbar sympathectomy of a blocked abdominal aorta.
The syndrome is considered an exclusively male pathology; they encounter it 10 times more often than women, and the conditional risk age group is considered to be the period from 40 to 60 years. But here it is important to understand that chronic blockage of the aorta is precisely a set of clinical manifestations, and not at all an independent disease. Consequently, treating the syndrome and ignoring the causes that caused it will achieve a visible improvement in the patient’s condition, but will not stop the destructive processes in the aorta.
Risk factors
Like any other disease, the appearance of the syndrome depends on a person’s lifestyle and heredity. Thus, the main risk factors for the occurrence of pathology include:
- Male gender;
- Genetic predisposition;
- Endocrine diseases;
- Metabolic disease;
- Adverse habits: smoking, alcoholism;
- Diabetes;
- Prolonged depression, stressful situations;
- Passive lifestyle;
- Poor diet with a predominance of fatty foods;
- Lack of rest, sleep;
- Regular increase in blood pressure.
Most often, Leriche syndrome appears due to atherosclerosis of the iliac arteries and aorta, nonspecific aortoarteritis and obliterating endarteritis, which can lead to thrombosis, atherosclerosis and impaired lumen patency.
narrowing and blocking of arteries
Usually, in the first stages of the anomaly, a narrowing of the blood vessels occurs, then the blood flow stops. In severe cases, a lack of oxygen occurs in the cells of the body, trophism is disrupted, and tissue death begins. The syndrome is accompanied by ischemia of the heart and cerebral vessels.
Symptoms
The symptoms of Leriche syndrome are as follows:
- The occurrence of parietal calcifications and blood clots.
- Excessive thickening of the walls of the aorta.
- The presence of severe soreness in the calf and gluteal muscles, which intensifies while walking or running.
- Presence of intermittent claudication.
- Pathology of distal blood flow.
- A feeling of chilliness in the extremities, and this is extremely rarely explained by an actual decrease in temperature in the environment.
- Increasing erectile dysfunction, sooner or later leading to complete impotence. It is worth noting that treatment of sexual impotence in this situation is completely useless. The symptoms of Leriche syndrome are quite unpleasant.
- The presence of cyanosis of the skin of the legs above the knee.
- Decreased lean body mass.
- The temperature of the affected limb is usually reduced by one to two degrees.
- The presence of ulcerations on the skin, which at the last stage can lead to necrosis. In this case, the lesion mainly affects the feet.
- Inability to detect pulsation of the femoral artery.
- Presence of systolic murmur in the groin area.
The main causes of the disease
Leriche syndrome can be congenital or acquired.
Congenital changes include genetically determined fibromuscular dysplasia and blockage of blood vessels.
Among the main acquired reasons are the following:
- Hypoplasia and aplasia of the aorta;
- Chronic arterial diseases;
- Embolism and thrombosis;
- Formation of blood clots in blood vessels;
- Inflammation of the aorta and interruption of its arch.
The main changes in the syndrome occur in the area of division of the aorta into 2 equal parts and in the area of the branch of the iliac aorta. With atherosclerosis, an accumulation of plaques is observed in this place.
As a result of arteritis, the vessels thicken and lose their elasticity. If therapy at this moment is absent or does not bring the desired effect, a narrowing of the aorta occurs, which leads to an accumulation of platelets. An insufficient amount of blood entering the pelvic organs and lower extremities leads to tissue hypoxia and metabolic disorders. Ischemia of various organs appears: at first during physical activity, and as the syndrome develops - even during rest.
Postoperative period and complications of Leriche syndrome
The first hours of the postoperative period are especially unfavorable in terms of thrombosis of the prosthesis and the resulting hemodynamic disturbances. The most important task of the anesthesiologist and the ward doctor is to maintain stable hemodynamic conditions after surgery, because the pressure is reduced below 100 mm Hg. Art. may cause shunt thrombosis. All failures during these operations occur in the first minutes and hours after the end of the operation. The percentage of late thrombosis in Leriche syndrome is very small. Typically, after a traumatic and lengthy operation and significant blood loss, when the shunt is inserted into the bloodstream, a drop in blood pressure occurs. This period requires the anesthesiologist to take appropriate measures. The introduction of vasoconstrictors (ephedrine, adrenaline, norepinephrine), increasing peripheral resistance, further complicates the work of the heart and leads to even greater depletion of the contractile resources of the myocardium. Therefore, such drugs should be prescribed in minimal doses.
The sometimes observed states of collapse with an uncontrollable drop in blood pressure are explained by exhaustion of the adrenal system and adrenal insufficiency. Therefore, before and during surgery, patients should be prescribed cortisone (50-75 mg hydrocortisone suspension 1-2 days before surgery), as well as for 2-4 days after surgery.
Instead of vasoconstrictors, when blood pressure drops in the postoperative period, it is rational to administer fast-acting cardiac drugs (strophanthin).
Another almost constant complication of the postoperative period with Leriche syndrome is severe intestinal paresis due to injury to the nervous system (primarily the plexus aorticus) and the inevitable formation of a hematoma in the retroperitoneal space. To combat this complication, it is necessary to ensure that the patient is given a sufficient amount of proteins (plasma transfusion) and, within 2-4 days after surgery, to carry out a set of measures to combat postoperative intestinal paresis (limit oral nutrition, prescribe pituitrin, hypertonic sodium chloride solution intravenously, enemas with hypertonic solution, gastric lavage, siphon enemas). Some doctors recommend inserting a thin catheter through the nose before the end of the operation, which is then passed into the intestines, through which the contents of the small intestine are evacuated in the postoperative period. To prevent intestinal paresis during surgery, novocaine blockade of the mesentery of the small intestine and retroperitoneal space should be performed.
Anticoagulant therapy after surgery is not recommended by many authors. Such treatment is carried out only if there is a threat of thrombosis (heparin intramuscularly in equal doses under the control of blood clotting time). After 2-3 days, heparin should be replaced with coumarin drugs.
Have questions or something is unclear? Ask the article editor - .
Reconstructive operations for Leriche syndrome in more than 90% lead to successful results immediately after the intervention.
Long-term results are also very favorable. The possibility of repeated operations for Leriche syndrome further improves long-term results. The article was prepared and edited by: surgeon I.B. Pigovich.
Video:
Healthy:
Related articles:
- Takayasu syndrome Occlusion of the branches of the aortic arch – Takayasu syndrome is a blockage of the vessels extending from the aortic arch….
- Obliterating atherosclerosis of the arteries With obliterating atherosclerosis of the arteries, damage to the great vessels usually occurs in one area of the body, sometimes...
- PANDAS syndrome When assessing a child with clinical chorea, you should also remember about PANDAS syndrome (Pediatric Autoimmune Neurophsichiatric...
- Horner's syndrome after thyroidectomy Horner's syndrome, first described by Bernard (1853) and Horner (1869), includes a tetrad of symptoms: unilateral miosis, ptosis, ...
- Classification of aortic aneurysms Aortic aneurysms are divided: according to localization: a) thoracic region: sinus of Valsalva (A), ascending part (B), arch...
- Diagnosis of occlusive lesions of the abdominal aorta Diagnosis of occlusive lesions of the abdominal aorta. Angiographic semiotics of occlusive-stenotic lesions of the abdominal aorta is determined by the morphology and localization...
Symptoms of the disease
Already at the initial stages of the disease, Leriche syndrome is accompanied by:
- Numbness in the legs and their weakness;
- Tingling, burning sensation in the lower extremities;
- Pain in the calf muscles after a long walk.
Sometimes the disease may remain undetected until serious symptoms appear:
Impotence. Problems with sexual life in men appear due to decreased muscle tone and insufficient blood flow to the pelvic area.- Lameness. This symptom occurs due to pathologies of blood flow in the extremities. The lameness can be high or low, depending on the location of the narrowing of the blood vessels. In cases of low lameness, discomfort radiates to the feet. Sometimes when moving, the pain moves to the lumbar region.
- Decreased muscle tone in the legs.
- Absence of pulse in the arteries of the legs.
- Thrombosis and acute blood flow disorders.
Leriche syndrome can also be determined by the appearance of the lower extremities.
The skin of the legs first turns pale and then acquires a bluish tint. Hair begins to fall out, the nail plate breaks and stops growing. Bruises, trophic ulcers, and necrosis often appear. Ultimately, the patient faces gangrene and amputation of the limb.
Prognosis and life with Takayasu arteritis
Takayasu arteritis is a chronic condition and may require long-term treatment. Some patients have no symptoms or only mild signs of the disease, but others are disabling or require surgery more than once. Side effects from medications, mainly glucocorticoids, can be worrying. Patients taking immunosuppressants are at risk of infections.
Because Takayasu's arteritis can cause heart problems, high blood pressure, and stroke, patients with Takayasu's disease should talk to their doctor about ways to reduce the risk of these serious problems. Taking blood pressure in the arm is often incorrect because it will be falsely low due to blocked arteries, so the doctor may need to take blood pressure in the leg.
The disease may recur after treatment or may get worse unnoticed. It is often very difficult to know whether Takayasu syndrome has recurred. Thus, most patients require frequent doctor visits and angiograms.
Stages
The clinical picture of the disease involves 4 stages of the disease:
- The first stage is characterized by weakness, chilliness, numbness and burning in the legs, as well as the appearance of lameness after long walks.
- In the second stage, the lumen of the arteries decreases, trophic ulcers form, and the growth of hair and nails is disrupted.
- During the third, the muscles of the lower extremities weaken, pain occurs even at rest.
- The fourth is the most dangerous stage, which is accompanied by multiple ulcers, unbearable pain and necrosis of soft tissues. The patient cannot walk. Amputation is urgently required.
Diagnosis of the syndrome
If you suspect Leriche syndrome, you should immediately contact a specialist to prevent complications from occurring.
First of all, the doctor should feel the pulse in the arteries of the lower extremities and examine them: the legs should not be pale and cold.
Leriche's syndrome in the picture
You should undergo a coagulogram and laboratory tests to determine glucose, lipid spectrum and glycosylated hemoglobin.
To identify the stage of the disease and the location of the lesion, it is necessary to perform computed aortography and angiography with the introduction of a contrast agent. To check the condition of the arteries, the patient is asked to perform a series of exercises on a treadmill.
Thanks to screening, it is possible to perform ultrasound of blood vessels with additional Doppler ultrasound. An examination of the condition of the cerebral and coronary arteries is mandatory.
How is Takayasu syndrome diagnosed?
Doctors most often detect Takayasu's disease by performing an angiogram , which shows how well blood flows in the arteries. A doctor will often order an angiogram when a patient has symptoms and abnormal physical examination findings. Signs include loss of pulse or low blood pressure in the arm, or abnormal sounds ("bruits") heard in the large arteries with a stethoscope .
There are different types of angiograms, including standard ones, which involve injecting dye directly into the artery during an X-ray examination. Less invasive types of angiography use a different imaging technique, such as a CT scan, and are called CT angiography or CTA . When MRI is used - magnetic resonance imaging - it is called magnetic resonance angiography or MR angiography, MRA .
Treatment
Treatment of the disease must be comprehensive. If therapy began on time, conservative treatment in combination with other physiotherapeutic procedures and traditional medicine will be quite sufficient. Surgical intervention will be required in the final stages of the disease.
Conservative therapy
Before starting to use various medications, you should undergo a complete examination of the body and make sure that the patient really has Leriche syndrome at its first or second stage. In this case, the main goal of treatment is to dilate the affected vessels and increase the functioning of the auxiliary arteries. To do this, doctors use:
- Agents that dilate blood vessels: “Papaverine”, “Phentolamine”;
- Ganglioblockers: “Mydocalm”, “Vasculat”;
- Anticholinergic drugs: “Dibazol”, “Andekalin”;
- Painkillers: “Spazmolgon”, “Pentoxifylline”;
- Medicines that reduce blood thickness: Thrombo-Ass, Anopyrin, Warfarin.
Only the attending physician should prescribe medications and set the required dosage. Also, you should not change or cancel the course of therapy on your own. If any side effects occur, you should definitely consult a specialist.
Together with drug treatment, physiotherapeutic effects can be used: Bernard currents, oxygenation, massage. Patients are recommended to rest in sanatoriums. Mud applications, hydrogen sulfide and radon baths will also have a positive effect.
Surgery
It is possible to help a patient with Leriche syndrome in the final stages only through reconstructive surgery. There are several types of intervention:
- Prosthetics. In this case, the affected area of the artery is removed, and a synthetic prosthesis or autovein is installed instead.
- Endarterectomy. Specialists remove the atherosclerotic plaque and sutured the vessel, replacing it with synthetic material.
- Stenting. A special frame is installed in the damaged vessel through which blood can move. This method is especially suitable for people with brain and heart diseases.
- Aortofemoral bypass surgery. During surgery, an anastomosis is performed on the affected area. If there is a bifurcation, specialists use a prosthesis.
1 – aortofemoral bypass surgery, 2 – stenting
After the operation, complete restoration of vascular patency occurs. Patients return to normal life, but they should still avoid heavy physical activity. Patients are recommended to take antiplatelet drugs: Clopidogrel, Aspirin. Sometimes such treatment becomes lifelong, just like taking antiplatelet drugs. Vascular medications should be taken in a course.
If restoration of blood flow becomes impossible or gangrene begins to develop, the only option is to amputate the limb to the area of healthy blood flow.
Also, do not forget that any operation has its contraindications. In this case, they include:
- Recent stroke;
- Cirrhosis of the liver;
- Acute and subacute stages of myocardial infarction;
- Kidney or heart failure.
Non-drug treatment
To make the therapy easier and faster, and to avoid any complications, you should use non-drug treatment methods:
- Laser and ultraviolet irradiation of blood;
- Hyperbaric oxygenation – a procedure that helps increase lymphatic drainage;
- Physiotherapeutic effects: electrophoresis and UHF.
Traditional medicine
Therapy with traditional medicine alone will not bring relief to the patient. It will only help if conservative treatment is carried out in parallel. Before starting to use folk remedies, you should definitely consult with your doctor.
To enhance the vasodilating effect of medications, get rid of swelling and unpleasant pain in the limbs and boost a person’s immunity, you can use the following recipes:
- To dilate blood vessels, prepare an infusion of 30 g of cornflower flowers, 40 g of bearberry leaves and 30 g of licorice root. The mixture must be brewed with a glass of hot water, left for 15-20 minutes and strained. During the day you need to drink 1 tablespoon 3 times.
- Due to the high content of potassium and vitamin C, lemon is also a good blood thinner. It can be eaten with other foods or added to drinks.
- Greens and parsley root need to be chopped in a meat grinder. The amount of the resulting mixture should be approximately two glasses. It needs to be transferred to a deep bowl, poured with a liter of hot boiled water, wrapped and left in a dark place for 7-8 hours. Afterwards, the infusion must be filtered, squeezed and mixed with freshly squeezed juice of one lemon. The resulting mixture is divided into 2 days and each part is drunk in 3 doses. The procedure is repeated every 3 days.
- To strengthen the blood vessels in the legs, you need to take baths with nettle decoction every 1-2 days.
- To prepare an alcoholic tincture of chestnut, pour 50 g of the peel into 0.5 liters of vodka and leave in a dark place for 2 weeks. For the first 10 days, you need to take the drink twice a day, 30 minutes before meals, half a teaspoon, then - a full teaspoon until the end of the thirty-day course. Then take a break for 7 days and repeat the treatment.
- To prevent the formation of blood clots and trophic ulcers, you need to regularly drink ginger tea, adding a small piece of lemon and a teaspoon of honey. Fresh ginger can be added to salads and soups.
- To boost your immunity and mood, you should prepare a drink of honey, lemon and garlic. It must be stored in the refrigerator. Take a teaspoon 5 minutes before meals.
How is Takayasu syndrome treated?
Rheumatologists are typically the experts with the greatest scope and knowledge of the disease. Consequently, they manage the entire treatment process for these patients, especially those patients who require immunosuppressive drugs. Other doctors patients may need include a cardiologist and a vascular surgeon. A team approach may offer the best care for patients with this disease.
Takayasu's disease most often requires treatment to prevent further narrowing of the affected arteries. However, narrowing that has already occurred often does not improve, even with medication. Glucocorticoids (Prednisone, Prednisolone or other similar drugs) , often called "steroids", are an important part of therapy. The dose and duration of treatment depend on how severe the illness is and how long the patient has had it. However, these drugs may have long-term side effects.
Doctors sometimes prescribe immune suppressant drugs because their side effects may be less severe than those of glucocorticoids. This is called "steroid-sparing" treatment. These medications include methotrexate, azathioprine, mycophenolate mofetil, cyclophosphamide, and medications that block tumor necrosis factor (such as etanercept, adalimumab, or infliximab) and other biologic drugs such as tocilizumab.
Doctors often prescribe these drugs to treat other rheumatic diseases, but they also use them to treat Takayasu syndrome. There is insufficient evidence that these drugs are definitively effective in treating nonspecific aortoarteritis. Research continues, scientists are constantly looking for new drugs to treat nonspecific aortoarteritis.
Some experts advise routine use of low-dose aspirin . This is supposed to help prevent blood clots from forming in damaged arteries. Treatment for Takayasu syndrome also includes screening for high blood pressure and high cholesterol, and treatment if these problems are present.