General information
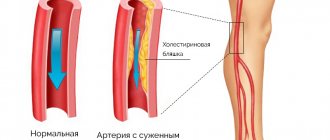
Diabetic angiopathy (abbr. DAP ) manifests itself in the form of impaired hemostasis and generalized damage to blood vessels, which are caused by diabetes mellitus and is its complication. If major large vessels are involved in the pathogenesis, then we speak of macroangiopathy , whereas in the case of disruption of the walls of the capillary network - small vessels, pathologies are usually called microangiopathy . Diabetes mellitus today affects more than 5% of the world's population; complications and generalized lesions of the cardiovascular system lead to disability due to the development of blindness, amputation of limbs, and even lead to “sudden death,” most often caused by acute coronary insufficiency or myocardial infarction .
The code for diabetic angiopathy according to ICD-10 is “I79.2. Diabetic peripheral angiopathy", diabetic retinopathy - "H36.0".
How does diabetic microangiopathy manifest in patients (symptoms)?
Manifestations of diabetic microangiopathy are varied. It all depends on the duration of the disease and the level of damage.
Symptoms of diabetic microangiopathy include:
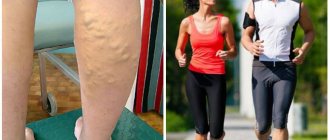
- pale skin, lack of hair growth on the extremities;
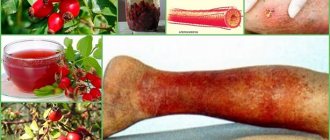
- the appearance of ulcerative defects (see photo above);
- coldness of the extremity;
- impaired sensitivity of the lower extremities;
- the appearance of pain in the limbs when walking;
- deep ulcerative defects on the skin of the extremities.
In the initial stages of the disease, the color of the skin changes and sensitivity is impaired. During the second stage, pain occurs in the extremities, cold temperatures, and worsening skin defects. During the third stage, deep ulcerative defects are formed, the blood supply to the lower extremities is disrupted, pain occurs when walking, and gangrene of the extremity forms.
The most severe complication of diabetic microangiopathy is the development of diabetic foot (photo above). It develops in 70% of cases and most often leads to the development of gangrene of the limb. Predisposing factors for the development of diabetic foot are:
- infection of ulcerative areas;
- fungal diseases of the feet:
- any damage to the skin;
- decreased immunity.
With the development of diabetic foot, there is a local change in temperature, absence of pulsation in the arteries, hyperemia of the skin, and swelling.
Pathogenesis
The pathogenesis is usually based on improper or ineffective treatment of hyperglycemia caused by diabetes mellitus. At the same time, patients develop shifts and severe metabolic disorders not only of carbohydrates, but also of proteins and fats; sharp changes in glucose levels are observed during the day - the difference can be over 6 mmol/l. All this leads to a deterioration in the supply of body tissues with oxygen and nutrients, vascular cells are also involved in pathogenesis, glycosylation of lipoproteins of the vascular wall occurs, deposition of cholesterol, triglycerides, sorbitol , which leads to thickening of the membranes, and glycosylation of proteins increases the immunogenicity of the vascular wall. Thus, the progression of atherosclerotic processes narrows blood vessels and disrupts blood flow in the capillary network. In addition, the permeability of the blood-retinal barrier increases and the inflammatory process develops in response to advanced glycation end products. The adverse effects are enhanced by hormonal imbalances - increased secretion of fluctuations in the bloodstream of somatotropic and adrenocorticotropic hormone , cortisol , aldosterone and catecholamines .
The process of development of angiopathy in diabetes is considered insufficiently studied, but it has been established that it usually begins with vasodilation and increased blood flow, resulting in damage to the endothelial layer and blockage of capillaries. Degenerative and disorganization processes, increased permeability of the vascular wall, impaired reactivity of autoregulatory function cause disruption of protective barriers and lead to the formation of microaneurysms , arteriovenous shunts , and causes neovascularization . Damage to the walls of blood vessels and microcirculation disorders are ultimately expressed in the form of hemorrhages.
Features of treatment
The basis of therapy is to maintain blood sugar levels within acceptable limits. The insulin-dependent type of diabetes mellitus requires injections of the pancreatic hormone (insulin) in accordance with a regimen developed by an endocrinologist. It is necessary to observe the injection time, dosage, and conduct self-monitoring using a glucometer.
For type 2 diabetes, hypoglycemic drugs are used:
Important! At the same time, you need to adhere to a low-carbohydrate diet by adjusting your diet.
Cholesterol-lowering agents
The drugs can be used both as part of therapy and to prevent the development of diabetic angiopathy of the lower extremities. Medicines should be taken with laboratory tests of biochemical blood parameters over time.
| Drug name | Active substance | Features of the action |
| Aterostat | Simvastatin | Reduces cholesterol and lipoprotein levels, contraindicated in renal failure, children, pregnant women |
| Zokor | Simvastatin | Normalizes the amount of triglycerides and total cholesterol levels. Take with caution in cases of liver or kidney pathology, increased levels of transaminases in the blood serum, or alcoholism. |
| Cardiostatin | Lovastatin | Reduces the liver's ability to form cholesterol, thus controlling its level in the blood |
| Lovasterol | Lovastatin | Analog of Cardiostatin. Not used during pregnancy, breastfeeding, severe renal failure |
| Liptonorm | Atorvastatin | Increases the protective mechanisms of the vascular wall, inactivates the process of cholesterol formation |
Antihypertensive drugs
Against the background of a decrease in blood pressure, vasodilation occurs, an antiarrhythmic effect. Blood circulation improves slightly. Products used:
- Nifedipine,
- Corinfar,
- Kordipin,
- Equator,
- Binelol,
- Nebilet.
Corinfar is a representative of a group of medications that lower blood pressure
The mechanism of vasodilation is based on the fact that receptors located in the walls of the arteries and heart are blocked. Some of the drugs can restore heart rhythm.
Angioprotectors
The action of this group of medications is aimed at improving blood supply to the tissues and cells of the body, as well as increasing the resistance of the walls of blood vessels.
- Pentoxifylline (Trental) - the drug helps to dilate blood vessels, improve blood supply, and increase the action of the protective mechanisms of the endothelium.
- Troxevasin – prevents lipid oxidation, has an anti-exudative effect, and stops the development of inflammatory processes.
- Niacin - by dilating blood vessels, the drug helps reduce total cholesterol levels.
- Bilobil - normalizes the permeability of vascular walls, participates in the restoration of metabolic processes.
Antiplatelet agents
Medical socks for diabetics
The drugs block the biochemical processes of thrombus formation, preventing blockage of the vascular lumen. The following representatives showed effectiveness:
- Aspirin,
- ReoPro,
- Tirofiban,
- Chime,
- Dipyridamole,
- Plavix.
Enzymes and vitamins
The drugs restore metabolic processes, participate in the normalization of the permeability of vascular walls, have an antioxidant effect, increase the level of glucose use by cells and tissues, thereby contributing to the process of its reduction in the blood. Solcoseryl, ATP, B vitamins, Ascorbic acid, Pyridoxine are used.
Sources
- https://SostavKrovi.ru/sosudy/bolezni/diabeticheskaya-angiopatiya-na-nogax.html
- https://glazaizrenie.ru/bolezni-glaz/angiopatiya-setchatki-kod-po-mkb-10-lechenie-tipy/
- https://diabetiko.ru/diabeticheskaya-angiopatiya-nizhnih-konechnostey
- https://nashdiabet.ru/oslozhneniya/simptomy-i-lechenie-diabeticheskoj-angiopatii.html
- https://diabet.guru/oslozhneniya-saharnogo-diabeta/diabeticheskaya-angiopatiya.html
Classification
Depending on the target organs, clinical and morphological differences, the following types of angiopathy are distinguished:
- macroangiopathy of neck vessels;
- micro- and macroangiopathy of the vessels of the lower extremities;
- microangiopathy of the stomach and duodenum;
- angiopathy of cerebral vessels;
- chronic ischemic heart disease
- diabetic angionephropathy;
- diabetic angioretinopathy.
Macroangiopathy
Macroangiopathy of the neck vessels is expressed in the form of obliterating atherosclerosis of the carotid artery system. This macroangiopathy causes certain diagnostic difficulties, since it is asymptomatic in the primary stages. A clear manifestation may be a stroke , which is usually preceded by cases of transient ischemic attack .
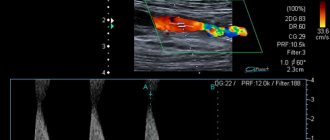
Results of angiographic study for stenosis of the internal and external carotid arteries
Diabetic angiopathy of the lower extremities
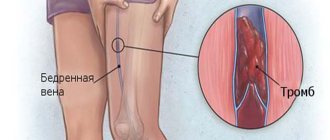
Typically, the pathogenesis involves large main and sometimes small vessels of the lower extremities - the femoral, tibial, popliteal arteries and arteries of the foot. They experience accelerated progression of obliterating atherosclerotic processes as a result of complex metabolic disorders. The most common is bilateral multiple localization of pathogenesis, occurring without specific symptoms. There are four stages of ischemia :
- preclinical;
- functional, expressed as intermittent claudication;
- organic , causing pain at rest and at night;
- ulcerative-necrotic, causing trophic disorders and gangrene directly.
Hypoxia and, as a consequence, necrosis and atrophy of the lower limb muscles in diabetic angiopathy are caused by morphological changes in the microvasculature - thickening of the basement membranes, proliferation of the endothelium and deposition of glycoproteins in the walls of capillaries, as well as the development of Mönckeberg mediacalcinosis , which is a pathology of the middle membranes of blood vessels and has a characteristic radiological and ultrasound picture.
Diabetic angiopathy of the lower extremities
Against the background of DAP, patients can also develop polyneuropathy , osteoartopathy and diabetic foot syndrome (DFS) . Patients experience a whole system of anatomical and functional changes in the vascular bed, disruption of autonomic and somatic innervation, deformation of the bones of the foot and even lower leg. Trophic and purulent-necrotic processes over time turn into gangrene of the foot, fingers, and legs and may require amputation or excision of necrotic tissue.
Angiopathy of cerebral vessels
Diabetic macroangiopathies of the brain cause apoplectic or ischemic disorders of cerebral circulation, as well as chronic cerebral circulatory failure. The main manifestations are dystonia , temporary reversible spasms and vascular paresis .
The clinical picture is most often caused by pronounced proliferation and hyperplasia of intimal connective tissue (thickening of the arterial wall), dystrophic changes and thinning of the muscular layer, deposits of cholesterol , calcium salts and the formation of plaques on the walls of blood vessels.
Microangiopathy
Thrombotic microangiopathy leads to narrowing of the lumen of arterioles and the formation of multiple ischemic foci of damage. Manifestations of microangiopathy can be acute (stroke) or chronic; they are usually caused by diffuse or focal organic changes of vascular origin. Cerebral microangiopathy of the brain causes chronic cerebral circulatory failure.
Microangiopathy of the brain - what is it? Unfortunately, it has been established that the disease is a complication of diabetes, which is characterized by rapid progression of atherosclerosis and microcirculation disorders, which are practically asymptomatic. The first alarm bells may be attacks of dizziness, lethargy, deterioration of memory and attention, but most often the pathology is detected in the later stages, when the processes are already irreversible.
Microangionephropathy
Another type of microangiopathy is diabetic angionephropathy, which disrupts the structure of the walls of the blood capillaries of the nephron glomeruli and nephroangiosclerosis , which causes a slowdown in glomerular filtration, a deterioration in the concentration and filtration function of the kidneys. In the process of diabetic glomerulosclerosis , nodular, diffuse or exudative, caused by impaired carbohydrate and lipid metabolism in the kidney tissues, all arteries and arterioles of the glomeruli and even the renal tubules take part.
This type of microangiopathy occurs in 75% of patients with diabetes. In addition, it can be combined with the development of pyelonephritis , necrotizing renal papillitis and necronephrosis .
Diabetic angioretinopathy
Angioretinopathy also refers to microangiopathies, because the network of retinal vessels is involved in the pathogenesis. It occurs in 9 out of 10 diabetics and causes such severe disorders as rubeous glaucoma , edema and detachment , and retinal hemorrhages , which significantly reduce vision and lead to blindness.
Depending on the developing vascular lesions (lipohyaline arteriosclerosis, expansion and deformation, dilatation, increased permeability, local blockage of capillaries) and complications, the following may occur:
- non-proliferative (disturbances cause the development of microaneurysms and hemorrhages);
- preproliferative (venous anomalies are detected);
- proliferative (in addition to preretinal hemorrhages, neovascularization of the optic nerve head and various parts of the eyeball, as well as proliferation of fibrous tissue, is observed).
Diabetic macroangiopathy :: Symptoms, causes, treatment and code according to ICD-10
Title: Diabetic macroangiopathy.
Diabetic macroangiopathy
Diabetic macroangiopathy.
Generalized atherosclerotic changes developing in medium- and large-caliber arteries against the background of long-term diabetes mellitus.
Diabetic macroangiopathy leads to the occurrence of ischemic heart disease, arterial hypertension, cerebrovascular accidents, and occlusive lesions of peripheral arteries.
Diagnosis of diabetic macroangiopathy includes the study of lipid metabolism, ultrasound examination of the arteries of the extremities, cerebral vessels, kidneys, ECG, echocardiography, etc. The main principles of treatment of diabetic macroangiopathy are correction of hyperglycemia, dyslipidemia, blood pressure control, improvement of rheological properties of blood.
Diabetic macroangiopathy is a complication of diabetes mellitus, leading to primary damage to the cerebral, coronary, renal and peripheral arteries.
Clinically, diabetic macroangiopathy is expressed in the development of angina, myocardial infarction, ischemic strokes, renovascular hypertension, and diabetic gangrene.
Diffuse vascular damage is of decisive importance in the prognosis of diabetes mellitus, increasing the risk of stroke and coronary artery disease by 2-3 times; gangrene of the limbs - 20 times. Vascular atherosclerosis, which develops in diabetes mellitus, has a number of specific features.
In diabetics, it occurs 10-15 years earlier than in people who do not suffer from impaired carbohydrate metabolism, and progresses faster. Diabetic macroangiopathy typically involves generalized damage to most arteries (coronary, cerebral, visceral, peripheral). In this regard, the prevention and correction of diabetic macroangiopathy is of paramount importance in endocrinology.
Diabetic macroangiopathy
With diabetic macroangiopathy, thickening of the basement membrane of medium- and large-caliber arteries occurs with the formation of atherosclerotic plaques on it.
Their subsequent calcification, ulceration and necrosis contribute to the local formation of blood clots and occlusion of the lumen of blood vessels, which leads to impaired circulation in certain areas.
Specific risk factors for the development of diabetic macroangiopathy in diabetes mellitus include hyperglycemia, dyslipidemia, insulin resistance, obesity (especially abdominal type), arterial hypertension, increased blood coagulation, endothelial dysfunction, oxidative stress, systemic inflammation. Traditional risk factors for atherosclerosis are smoking, occupational intoxication, physical inactivity, age (in men over 45 years old, in women over 55 years old), and heredity.
Diabetic angiopathy is a collective concept that includes damage to small vessels - capillaries and precapillary arterioles (microangiopathy), medium and large arteries (macroangiopathy).
Diabetic angiopathy refers to late complications of diabetes mellitus, developing on average 10-15 years after the manifestation of the disease.
Diabetic macroangiopathy can manifest itself in a number of syndromes: atherosclerosis of the coronary arteries and aorta, atherosclerosis of the cerebral arteries and atherosclerosis of the peripheral arteries. Diabetic microangiopathy may include retinopathy, nephropathy, microangiopathy of the lower extremities.
Also, vascular damage can occur in the form of universal angiopathy, combining macro- and microangiopathy. In turn, endoneurial microangiopathy contributes to dysfunction of peripheral nerves, i.e., the development of diabetic neuropathy.
Diagnosis of diabetic macroangiopathy is designed to determine the extent of damage to the coronary, cerebral and peripheral vessels. To determine the examination algorithm, consultations with an endocrinologist, diabetologist, cardiologist, vascular surgeon, cardiac surgeon, and neurologist are organized. The study of the biochemical profile of the blood includes determining the level of glycemia (blood glucose), lipid spectrum indicators (cholesterol, triglycerides, lipoproteins), platelets, and coagulogram. Examination of the cardiovascular system in diabetic macroangiopathy includes ECG registration, 24-hour ECG and blood pressure monitoring, stress tests (treadmill test, bicycle ergometry), echocardiography, ultrasound of the aorta, myocardial perfusion scintigraphy (to detect hidden ischemia), coronary angiography, CT angiography.
The neurological status is clarified using ultrasound and duplex scanning of cerebral vessels, angiography of cerebral vessels. To assess the condition of the peripheral vascular bed in diabetic macroangiopathy, ultrasound and duplex scanning of the vessels of the extremities, peripheral arteriography, rheovasography, capillaroscopy, and arterial oscillography are performed.
Treatment of diabetic macroangiopathy is aimed at slowing the progression of dangerous vascular complications that threaten the patient with disability or death. The basic principles of treatment for diabetic macroangiopathy are the correction of the syndromes of hyperglycemia, dyslipidemia, hypercoagulation, and arterial hypertension. In order to achieve compensation for carbohydrate metabolism, patients with diabetic macroangiopathy are prescribed insulin therapy under the control of blood glucose levels. Correction of carbohydrate metabolism disorders is achieved through the prescription of lipid-lowering drugs (statins, antioxidants, fibrates), as well as a diet that limits the intake of animal fats. With an increased risk of thromboembolic complications, it is advisable to prescribe antiplatelet drugs (acetylsalicylic acid, dipyridamole, pentoxifylline, heparin, etc.). The goal of antihypertensive therapy for diabetic macroangiopathy is to achieve and maintain a target blood pressure level of 130/85 mm. For this, it is preferable to prescribe ACE inhibitors (captopril), diuretics (furosemide, spironolactone, hydrochlorothiazide); patients who have had a heart attack - beta-blockers (atenolol, etc.).
Treatment of trophic ulcers of the extremities is carried out under the supervision of a surgeon. In case of acute vascular accidents, appropriate intensive therapy is carried out. According to indications, surgical treatment is performed (CABG, surgical treatment of cerebrovascular insufficiency, endarterectomy, limb amputation, etc.).
Mortality from cardiovascular complications in patients with diabetes reaches 35-75%. Of these, in approximately half of the cases death occurs from myocardial infarction, in 15% from acute cerebral ischemia.
The key to preventing diabetic macroangiopathy is maintaining optimal blood glucose and blood pressure levels, following a diet, controlling weight, giving up bad habits, and following all medical recommendations.
42a96bb5c8a2ac07fc866444b97bf1 Content moderator: Vasin A.S.
Source: https://kiberis.ru/?p=33726
Causes
The pathogenesis of diabetic angiopathy is quite complex and scientists put forward several theories of damage to small and large vessels in diabetes mellitus. The underlying etiology may be:
- metabolic disorder ;
- hemodynamic changes;
- immune factors;
- genetic predisposition.
People at risk for developing angiopathy are usually:
- male;
- with a hereditary history of hypertension ;
- obese ; _
- with diabetes mellitus experience of more than 5 years;
- manifestation of diabetes mellitus occurred before the age of 20;
- suffering from retinopathy or hyperlipidemia ;
- smokers
Causes of diabetic microangiopathy
The causes of diabetic microangiopathy can be:
- diabetes mellitus, which is characterized by frequent increases in blood glucose. As the disease progresses, the walls of small vessels are destroyed. Thinning, thickening and deformation of blood vessels occurs. All these processes disrupt normal blood flow and, as a result, ischemia develops, which leads to hypoxia of organs and tissues of the body. Prolonged hypoxia disrupts metabolic processes;
- heart rhythm disturbances. When diabetes mellitus is combined with cardiac arrhythmia, thrombosis of small vessels occurs, including coronary ones;
- age over 50 years. Metabolic disorders in the body can develop as we age. The older the patient is, the higher the risk of developing diabetes mellitus, especially if there is a hereditary predisposition. With age, cholesterol plaques are deposited in the walls of blood vessels, and atherosclerosis occurs. Such changes may contribute to the development of microangiopathy;
- lipid metabolism disorder. Lipid metabolism directly affects the maintenance of normal blood flow. If the level of low-density lipids increases in the body, atherosclerosis occurs. Atherosclerosis closes the lumen of blood vessels, which causes microangiopathy.
Provoking factors for the development of the disease:
- genetic predisposition to the development of diabetes mellitus;
- consumption of alcoholic beverages. Alcoholic drinks contribute to the thinning of the walls of blood vessels, which leads to a violation of their integrity. As a result, their permeability increases and blood clots appear. Vascular thrombosis leads to microangiopathy ;
- smoking. Due to the influence of a large number of carcinogens on the vascular wall, its destruction occurs. It becomes thinner and becomes easily permeable to external influences, including infectious agents. The formation of blood clots is a protective factor in case of damage to the vessel wall. However, it should be remembered that long-term smoking causes chronic damage to the vascular wall, which leads to the development of microangiopathy;
- arterial hypertension. Arterial hypertension contributes to increased pressure in the vascular bed. High pressure thins the vessel wall, which is a predisposing factor for the development of deposits in it, which lead to impaired blood flow.
When diabetic microangiopathy occurs, damage most often occurs to the lower extremities and heart muscle, blood vessels of the eyes, brain, and kidney vessels. This occurs due to the fact that the vessels of these organs carry out the greatest load. The vascular network of the fundus is sensitive to changes in metabolic processes in the body. Therefore, the first symptom of diabetic microangiopathy is visual impairment.
The pathological process in the vessels of the heart and lower extremities accelerates due to increased load. Damage to the renal vasculature may also be common. This pathology is called diabetic nephropathy. Damage to cerebral vessels in diabetes mellitus leads to diabetic encephalopathy. Such damage occurs in 65% of patients and most often in type 1 diabetes.
With the development of diabetic microangiopathy, complications often arise that can lead to death. Strokes, heart attacks and hemorrhages in internal organs develop. Diabetic microangiopathy is a serious disease associated with metabolic disorders that occurs with long-term diabetes mellitus.
Symptoms
Despite the fact that patients most often pay attention to the symptoms caused by diabetes mellitus - polyuria, thirst, itching, hyperkeratosis, etc., angiopathy developing against the background can provoke:
- swelling;
- arterial hypertension;
- ulcerative necrotic lesions on the feet;
- sensitivity disorders;
- pain syndrome;
- convulsions;
- fatigue and pain in the legs when walking;
- cold and bluish extremities, decreased sensitivity;
- poor wound healing, the presence of trophic ulcers and degenerative skin changes;
- dysfunction or chronic renal failure ;
- blurred vision and possibly even blindness.
Vascular angiopathy of the lower extremities: treatment, prevention, symptoms, causes - About Blood
- July 9, 2018
- Neurology
- EgorHas
Angiopathy of the lower extremities is a disease not only of the veins and capillaries, but also of the arteries.
Diabetic angiopathy is its complication, the occurrence of which is more prone to people suffering from diabetes.
Against the background of the disease, blood vessels and capillaries decompose, after which blood stagnates.
Forms of the disease
To date, experts have divided diabetic angiopathy into two types:
- Macroangiopathy. This form affects the heart and blood vessels of the lower extremities. It causes blood clots and lipids to accumulate in blood vessels, sticking to the walls and blocking blood flow.
- Microangiopathy. This form causes damage to the kidneys and eyes. The walls of the blood vessels weaken and bleed, causing protein to leak.
Code I79.2 was assigned to angiopathy of the lower extremities (ICD-10). This disease develops in 6 stages:
- There are no serious deviations, but kidney function is disrupted, arterial hypertension and proteinuria appear, which is quite difficult to diagnose. To ensure that the disease is progressing, a kidney biopsy is required.
- The skin on the legs turns pale, the lower extremities themselves become cold, red ulcers gradually appear, but no pain is felt.
- The ulcers become painful and discomfort appears.
- The ulcers become black and red in color, the area around them swells, and hyperemia of the skin progresses. At this stage, osteomyelitis may occur, which affects the bone elements, as well as the bone marrow. In most cases, abscesses, ulcers and abscesses occur.
- Tissues die, affecting nearby areas.
- The disease spreads to the entire foot (necrosis).
In diabetes, angiopathy of the lower extremities (diabetic macroangiopathy) goes through 5 stages:
- There are no deviations from the norm, there is increased leg fatigue, a feeling of tingling or numbness. If you undergo a full medical examination, atherosclerosis, as well as arterial hypertension, can be detected.
- You feel tired, uncomfortable and very weak. The legs and feet become numb, and the lower extremities often become cold and sweaty. The feet and toes atrophy, and intermittent claudication appears.
- There is severe pain in the lower extremities. Pain sensations become more acute when a person changes a horizontal position to a vertical one. Cramps appear more and more often, pain intensifies at night, the skin of the legs turns pale and peels.
- Single or multiple ulcers with signs of necrosis are formed.
- Fingers die, body temperature rises, the patient suffers from fever, gangrene and chills.
Medicines
The treatment process for vascular angiopathy of the lower extremities will be determined depending on the severity of the infectious infection, as well as the presence of infections that threaten the patient’s life (sepsis, osteomyelitis, gangrene, and so on). Quite often used in treatment:
- antioxidants;
- antibiotics to fight infected ulcers;
- B vitamins;
- statins that lower cholesterol;
- blood thinners;
- metabolic drugs that can improve energy supply to tissues;
- angioprotectors that help reduce vascular swelling and normalize metabolism.
In most cases, doctors prescribe the following medications to their patients:
- "Pentoxifylline" (180 rubles). The product perfectly accelerates microcirculation and eliminates vascular edema. One tablet is taken a couple of times a day, and the entire course of treatment is 4 weeks.
- "Cardiomagnyl" (300 rubles). This drug is intended to thin the blood. It must be taken less often - only 1 tablet per day. The duration of the appointment is prescribed by the doctor.
- "Venoruton" (700 rubles). The product allows you to improve blood circulation, as well as relieve swelling and pain. You need to take it 3 times a day, 1 capsule. The course of treatment is 3 months.
Surgical intervention
Treatment of the disease with the help of a surgeon is indicated only for progressive forms. Depending on the patient's condition, arterial reconstruction, sympathectomy, and thromboembolectomy may be performed.
A forced measure is amputation of the lower limbs. They turn to her only if the disease reaches the final stage.
Preventive measures
Prevention includes actions such as:
- wound treatment;
- reduction of friction and pressure;
- treatment of any infections;
- restoration of normal blood flow;
- reduction of glucose levels and its careful control.
Diet and sport
In case of diabetic damage to the blood vessels of the lower extremities, the following foods should be excluded from the diet:
- red meat;
- simple carbohydrates;
- hot and overly spicy seasonings;
- sour, fried and salty dishes.
Despite this, a healthy diet when sick involves eating tasty foods, which include:
- vegetables;
- fish;
- fruits;
- beans;
- whole grains;
- rice;
- buckwheat;
- quinoa;
- dietary meat.
During the treatment period, you should not neglect vitamins, especially vitamins B and D. They play an important role in the healthy state of the nervous system.
At the same time, it is recommended to regularly engage in simple sports that are accessible to everyone. These include: yoga, cycling, brisk walking. The most basic physical exercises will do, but it is very important to do them every day.
Source:
Diabetic angiopathy of the lower extremities
Due to the widespread prevalence of diabetes mellitus and the increase in disability due to diabetes-related causes, increasing importance is being attached to the prevention and treatment of complications of this disease. One of the most common and serious complications is diabetic angiopathy. Let's take a closer look at this problem.
Diabetic angiopathy is vascular damage associated with diabetes mellitus. As a rule, angiopathy develops 10–15 years after the onset of the disease, however, it can occur earlier if blood glucose levels are high for a long time or often “jump” from high to low numbers.
What is angiopathy?
There are two types of angiopathy, depending on which vessels are affected:
- Microangiopathies - small vessels and capillaries are affected. Microangiopathies are divided into:
- Retinopathy is damage to the blood vessels of the eyes.
- Nephropathy is damage to the blood vessels of the kidneys.
- Macroangiopathies – large vessels, arteries and veins are affected:
- Cardiac ischemia.
- Cerebrovascular disease.
- Peripheral angiopathy.
Microangiopathies
With diabetic retinopathy, hemorrhages occur in the retina, the vessels dilate, thicken, and the retina ceases to receive enough oxygen. New vessels grow into it, leading to damage to the optic nerve and retinal detachment. If treatment, including laser coagulation, is not carried out, complete loss of vision is possible.
Source: https://igl-clinic.ru/krovotecheniya/angiopatiya-sosudov-nizhnih-konechnostej-lechenie-profilaktika-simptomy-prichiny.html
Tests and diagnostics
Diabetic microangiopathy is characterized by an asymptomatic course, which leads to delayed diagnosis, therefore all individuals suffering from diabetes undergo annual screening, including:
- serological studies ( CBC, concentration of glucose, creatinine, urea, cholesterol, lipoproteins, glycosylated hemoglobin , etc.);
- detailed urine tests to assess albuminuria , glomerular filtration rate;
- measuring blood pressure at different levels of the limbs;
- ophthalmological examination;
- performing computer video capillaroscopy and contrast angiography with various modifications - RCAG, CTA or MRA .
Diagnostics
Timely diagnosis of the disease is extremely important, because the prognosis and outcome of the disease, as well as the treatment initiated, will depend on this.
Diagnosis of diabetic microangiopathy includes:
- arteriography. This method involves visualizing the arteries by injecting a contrast agent into the femoral artery. Arteriography is highly informative;
- Ultrasound examination of the arteries of the lower extremities. This method is relatively inexpensive and easy to equip. Ultrasound allows you to determine the thickness of the artery wall and identify their obstruction. And also, using ultrasound, you can evaluate blood flow in the arteries and veins of the lower extremities;
- Dopplerography. It also measures the speed of blood flow and the consistency of the valve apparatus of the veins. Most often, this method is used in the presence of trophic ulcers in the patient;
- KBC, BAC, OAM, determination of blood glucose levels.
With the development of nephropathy, blood tests may not reveal anything, however, a urine test in this case may be the only reliable method of detection. With nephropathy in the urine, an increase in urea and creatinine levels, as well as a decrease in glomerular filtration, can be detected.
If retinopathy develops, an examination by an ophthalmologist is necessary. Examination of the condition of the fundus is especially important.
If the arteries of the lower extremities are affected, ultrasound may reveal thickening or, conversely, thinning of the vascular wall. With the development of atherosclerosis of the vessels of the lower extremities, cholesterol plaques are found in the wall of the arteries, which interfere with normal blood flow. This can also be confirmed by Doppler ultrasound. A change in blood flow will be detected. Arteriography will confirm the nature and level of the lesion.
If any symptoms of the disease occur, you must immediately visit an endocrinologist, surgeon, therapist, or ophthalmologist . Only after a thorough examination can specialized treatment be prescribed. You should not self-medicate.
Treatment of diabetic angiopathy
In the treatment of diabetic angiopathy, an important role is played by the selection of an adequate dosage regimen and the use of insulin with hypoglycemic drugs, as well as:
- normalization of arterial blood pressure;
- resumption of main blood flow;
- diet therapy to restore lipid metabolism;
- prescription of antiplatelet agents (most often it is recommended to take acetylsalicylic acid ) and angioprojectors , for example: Anginin ( Prodectin ), Dicinon , Doxium , as well as such vitamin complexes that provide the body with the daily requirement of vitamins C, P, E, group B (note taken in courses 1 month at least 3-4 times a year).
Treatment of diabetic angiopathy of the lower extremities
To improve the patency of the vessels of the lower extremities, it is of great importance to eliminate the main risk factors for atherosclerosis - hyperlipidemia , hyperglycemia , excess body weight, smoking. This gives a preventive and therapeutic effect at any stage of diabetic macroangiopathies.
Patients, even with asymptomatic atherosclerosis of the arteries of the extremities, are prescribed lipid-lowering, antihypertensive and hypoglycemic drugs, a strict diet, training walking and exercise therapy. Antiplatelet and vasoactive drugs are also effective; their use increases the walking distance without pain symptoms several times.
Treatment of cerebral microangiopathy
Treatment of cerebral microangiopathy is most often carried out with nootropics and antiplatelet agents. Statins may also be prescribed to slow the progression of microangiopathy and reduce the risk of stroke .
However, the prevention and treatment of cerebral complications require changes in lifestyle and eating habits - combating smoking, obesity , physical inactivity , limiting the consumption of alcohol, salt and animal fats.
The doctors
Medicines
- Reopoliglucin is a drug that has detoxification, improves microcirculation, antiaggregation, antishock and plasma-substituting effects. Recommended for disorders of capillary blood flow. The course of treatment is 7-10 days.
- Reomacrodex is an effective remedy for normalizing arterial and venous circulation, reducing blood viscosity and restoring blood flow in the capillary network. Initial infusions are administered intravenously at 500–1000 ml over 30 minutes, 1 time per day.
- Curantil is a vasodilating agent with additional immunomodulatory, angioprotective and antiaggregation effects. It should be taken for a long period of 8-10 weeks, the maximum daily dose should not exceed 600 mg.
- Trental is an antiplatelet agent, angioprotector and microcirculation corrector. Taking the drug helps normalize the rheological properties of the blood and dilate blood vessels. Available in tablets, take 1-2 per day.
Procedures and operations
- Laser photocoagulation - the procedure allows for coagulation of abnormal blood vessels and restoration of detached layers of the retina; it is indicated for preproliferative and proliferative angioretinopathy.
- For diabetic macroangiopathies, arterial reconstruction may be indicated - transluminal angioplasty in case of iliac artery stenosis , dilatation of the arteries of the femoral-popliteal segment, standard bypass operations.
How to deal with the diagnosis of “diabetic angiopathy” - symptoms and treatment
Diabetic angiopathy is the general name for several pathologies that occur in diabetes.
The disease affects the blood vessels of various organs.
All types of vessels are affected.
In case of mass lesions in small ones, the disease is characterized as microangiopathy, in large ones – macroangiopathy.
The disease is classified into three areas: heart, brain and legs.
Causes
Problems with blood vessels occur with prolonged high levels of glucose in the blood. Proper treatment of diabetes helps prevent the disease.
In addition to the main cause, there are several factors that can cause angiopathy:
- Age. Older people are susceptible to cardiovascular problems;
- High blood cholesterol levels;
- Slow or impaired metabolism.
Pathology begins to develop with thinning and gradual changes in the walls of blood vessels. Rebuilt tissues do not allow fluid to pass through, which leads to metabolic disorders and the accumulation of toxic products in the body.
In parallel with the blood vessels, the nerves begin to suffer. The patient gradually loses sensitivity, and symptoms begin due to impaired brain function.
Patients at risk
Different categories of people are vulnerable to angiopathy of various parts of the body:
- Patients over 50 years old;
- Patients with bad habits, poor diet, impaired metabolism;
- Heart patients with arterial hypertension, high cholesterol, arrhythmia.
- Angiopathy can occur due to hereditary characteristics.
Diabetic angiopathy affects patients with diabetes of any type.
Pathology develops faster when:
- Hyperglycemia – increased glucose levels;
- Excessive use of insulin;
- Insulin resistance;
- Improper functioning of the kidneys;
- Diabetes lasting more than ten years.
Vulnerable internal organs
Diabetic angiopathy affects the blood vessels, which affects the health of all organs. Each specific case is independent, so it is very difficult to predict the path of development of angiopathy.
The most vulnerable are:
- Heart;
- Brain;
- Eyeballs;
- Kidneys and lungs;
Separately, it is worth noting the lower limbs and the retina of the eyes. These are not internal organs. The chance of damage to the legs is very high and threatens the loss of the ability to move independently. Retinal angiopathy, due to the small size of the vessels, leads to partial or complete loss of vision.
Symptoms
Each affected area of the body causes a unique reaction in the body, although there are common symptoms.
In case of heart damage
Lack of energy caused by obstructed blood flow disrupts various processes.
A lack of substances provokes pain in the chest area and swelling of the limbs.
The pain is characterized as acute pressing. Symptoms are much stronger with physical activity .
An advanced disease causes the same phenomena when at rest.
Angiopathy is characterized by provoking shortness of breath with light exertion; progressive one also causes arrhythmia, detected using an electrocardiogram.
You may notice an increase in blood pressure. The most serious complication is necrosis - tissue death.
Brain damage
The brain suffers from a lack of nutrients along with the heart, but also loses its functionality due to the death of nerve endings. Brain angiopathy in diabetes mellitus Symptoms caused by diabetic brain angiopathy affect the emotional state and motor activity:
- In mild stages of the disease, memory is partially impaired, a headache occurs, which goes away when taking glucose-containing products, and dizziness is possible;
- A developed disease causes severe migraines, speech is impaired, the abilities of coordination in space, critical thinking, and acquiring new knowledge are lost;
- Severe illness is accompanied by impaired attention, convulsions, and necrosis. Possible stroke and coma.
Leg lesions
Angiopathy of the lower extremities causes changes in structure, tissue, and the occurrence of ulcers.
The symptoms are:
- Changes in the structure of nails;
- Change in skin color;
- The appearance of deep ulcers, swelling;
- In advanced cases, necrosis begins, and sometimes gangrene occurs. In this case, the limb is amputated to protect the remaining parts of the body.
For prevention during diabetes, you need to monitor the condition of visible parts of the body and perform hygiene procedures.
Diagnosis of angiopathy
The patient should contribute to establishing a diagnosis - monitor their health, well-being, and try not to use harmful substances. The initial survey should help the doctor understand what he is dealing with.
Upon examination, additional clinical examinations may be prescribed:
- General blood analysis. Plasma analysis for glucose and cholesterol levels;
- Urine analysis for protein composition, the presence of ketone bodies;
- Electrocardiogram if cardiac arrhythmia or hypertension is suspected;
- Ultrasound examination of blood vessels using contrast in various parts of the body;
- Daily monitoring of blood pressure and sugar.
Based on the results of the analysis, the doctor may ask to consult with his colleagues: a surgeon, ophthalmologist, cardiologist, neurologist, endocrinologist.
Possible complications and consequences of angiopathy
- Excess glucose in the body leads to disruption and damage to blood vessels due to a decrease in wall thickness;
- Macroangiopathy occurs more often in type 1 diabetics, and microangiopathy in those who are not dependent on insulin;
- A person's advanced age worsens symptoms and accelerates the development of pathology.
Reduced blood flow leads to general anemia. Decreased nutrition of a particular organ impairs its performance.
Starving tissues stop generating new cells, which, together with the death of old ones, causes direct harm to the body. Toxic substances also remain in the body because the elimination pathway is blocked.
Together, the factors lead to necrosis - the death of a part of the body. Necrosis is irreversible, but can be prevented, slowed, or stopped by amputation of the dead part of the body.
Angiopathy of the heart leads to spasm of the arteries, increased pressure in a vain attempt to bring energy to the desired point. Angina occurs. As the blood thickens, it forms blood clots and blocks the flow of fluids. Necrosis of structures close to the heart leads to myocardial infarction.
Angiopathy of the brain provokes acute migraine, loss of various higher abilities - coordination and fine motor skills, and in the last stage causes stroke, convulsions, paralysis, coma.
Pathology of the legs deprives a person of the ability to move calmly, and in severe cases leads to disability.
Pregnant women with angiopathy are at risk of miscarriage or early birth. The child may be susceptible to pathology - development will slow down, heart problems will appear.
Treatment
Diabetic angiopathy can be slowed down, stopped, and in some cases the body can be restored - it all depends on the severity, characteristics of the body and the patient’s desire to get better.
Based on examinations and in consultation with relevant specialists, the doctor suggests:
Medicines serve the conservative treatment of the disease - preventing its development. Taking into account the patient’s characteristics, the following are prescribed:
- Drugs that reduce blood clotting and increase its generation;
- Drugs that dilate blood vessels, promoting blood flow;
- Medicines to lower blood pressure;
- Antidepressants to relieve emotional stress on the body;
- Medicines to promote weight loss.
In severe cases, the use of surgical intervention methods to solve the problem is considered. In case of tissue necrosis, immediate removal of dead areas should be done to prevent expansion of the affected area.
If gangrene occurs, the limb must be amputated. Shunt surgery is used to improve blood flow. When treating pregnant women, medications are not allowed because they can harm the fetus.
Source: https://diabet.guru/oslozhneniya-saharnogo-diabeta/diabeticheskaya-angiopatiya.html
Diet for diabetic angiopathy
Diet 9th table
- Efficacy: therapeutic effect after 14 days
- Timing: constantly
- Cost of products: 1400 - 1500 rubles per week
A huge role in normalizing the condition of blood vessels in diabetes is played by diet therapy, which helps normalize the state of all types of metabolism and hormonal balance. The main techniques are:
- limiting the consumption of simple carbohydrates, but at the same time ensuring sufficient daily calorie intake according to height, weight, physical activity, etc.;
- replacing animal fats with vegetable ones;
- compliance with the drinking regime;
- control the consumption of table salt - no more than 5 g per day;
- if nephropathy is suspected, switch to a low-protein diet;
- increasing the consumption of lipotropic substances, mostly found in cottage cheese, fish, and oatmeal;
- the presence of plant foods in the diet - fruits and vegetables.
Description
Damage to the vascular network can occur in any part of the body, but the lower extremities are most often affected by angiopathy. During the onset of the disease, the microcirculation of the bed, which is an extensive plexus, changes. Sometimes ANC is detected even in clinically healthy people, and there are reasons for this.
Angiopathy is a general term for disease of the blood vessels (arteries, veins and capillaries).
Accordingly, ICD-10 angiopathy was assigned code 179.2. There are also two large subgroups based on the extent of damage to vascular formations:
- Microangiopathies - small vessels of various internal organs (kidneys, retina, etc.) are involved in the pathological process.
- Macroangiopathy - changes mainly affect large arteries, therefore this form of angiopathy is characteristic of diseases of the lower extremities.
The long course of angiopathy is characterized by a gradual decrease in vascular tone and a decrease in their lumen, as a result of which blood begins to flow less intensively through the altered areas. The emergence of ANC may be associated with the following development mechanisms:
- Damage to the muscle layer of the vessel wall
- Changes in nervous regulation
Regardless of the true cause of the development of ANC, the affected vessels spasm, their lumen decreases, and the blood flow through them decreases. Against the background of such changes, characteristic clinical signs arise, and in severe cases, serious complications.
Prevention
When a person is found to be suffering from lower extremity angiopathy, it is important to regulate blood pressure, blood glucose or cholesterol levels. Therefore, to prevent ANC, you need to follow a number of recommendations:
- Limit consumption of foods high in sugar and carbohydrates. Instead, a moderate-fat, high-protein diet is recommended.
- You need to take vitamin supplements and medications to improve nerve conduction and blood flow.
- To improve blood circulation, you need to do moderate exercise. Care should be taken that exercise does not cause fatigue, as this may cause cardiac arrest or stroke.
- It is necessary to regularly check your health, in particular it is necessary to determine the level of glucose and cholesterol in the blood.
- Regular examination by an ophthalmologist to prevent retinal damage.
- Proper foot care is essential. In particular, cuts and wounds should be avoided, as they are difficult to heal and can easily become infected.
- Maintaining blood pressure within acceptable limits is important in preventing ANC.
Retinal angiopathy ICD code 10. What is retinal angiopathy, and what is the disease code according to ICD 10,
Angiopathy is a change in the condition of the vessels of the retina, which can lead to the development of dystrophic changes (retinal dystrophy), myopia, optic nerve atrophy, etc.
Retinal vascular angiopathy is not a disease and ophthalmologists often focus on this, but a condition that can occur against the background of other diseases.
Pathological changes in blood vessels appear during injuries and damage, and are also observed in diabetes mellitus. What kind of disease is this and what its ICD-10 code is, you will learn from the article.
ICD-10 code
Angiopathy does not have a code according to the international classification, since it is not considered an independent disease. The code is assigned to the disease that led to the development of the pathological condition.
This is what retinal angiopathy looks like
What it is?
Angiopathy is a condition of retinal vessels in which capillary circulation changes due to disturbances in their nervous innervation. This occurs due to low blood filling of the vessels or their prolonged spasm.
Medicine does not distinguish angiopathy as an independent disease; modern scientific approaches classify it as one of the manifestations of the underlying disease.
Such a symptom complex can be a consequence of metabolic or hormonal disorders, injuries and intoxications, as well as the consequences of such bad habits as smoking or drug addiction.
Most often, angiopathy is diagnosed in the adult population (over 30 years of age); a small percentage occurs in childhood and adolescent forms of the pathology.
This condition, if detected and treated in a timely manner, is reversible. Only in advanced cases does the disease lead to serious complications:
- development of dystrophy and atrophy of the retina and optic nerve;
- decreased acuity and narrowing of visual fields.
Stages of retinal angiopathy
Treatment of angiopathy is prescribed by an ophthalmologist after a thorough examination. The success of therapy directly depends on procedures aimed at getting rid of the underlying disease.
Description of symptoms
Angiopathy has a number of specific signs that a person can notice, but leave without proper attention. Attributing the condition to stress or fatigue.
In most cases, patients complain:
- For the appearance of “flies” in the eyes.
- To reduce visual acuity.
- The appearance of flashes or fog before the eyes.
- For pain or colic in the eyeball area.
- For rapid fatigue of the visual organs.
- For the appearance of pinpoint hemorrhages or burst red blood vessels in the area of proteins.
It is necessary to pay attention to decreased visual acuity, the appearance of floaters or lightning before the eyes. Temporary, but complete or partial loss of vision. When, when getting out of bed or during heavy physical exertion, there is a sharp clouding in the eyes, an acute attack of dizziness.
This indicates that the person has problems with blood circulation in the brain, hypoxia or high intracranial pressure. Against the background of these pathologies, retinal angiopathy develops.
Symptoms may change and occur periodically (only when blood pressure levels increase), but these signs should not be ignored. If alarming symptoms appear, you should consult a doctor as soon as possible.
Source: https://alternativa-mc.ru/glaza-bolezni/angiopatiya-setchatki-mkb-10.html
Retinal angiopathy - treatment, symptoms - Moscow State Budgetary Institution Polyclinic No. 2
Today we will discuss a concomitant symptom that is often encountered in medical practice - retinal angiopathy, we will analyze what this means for human health, what signs and symptoms can indicate a problem, we will talk on alter-zdrav.ru about the causes, types and stages, diagnosis and treatment of this ocular pathology.
Retinal angiopathy - what is it, what does it mean, photo
Retinal angiopathy is a pathology that occurs as a consequence of other diseases of various nature and is manifested by a functional change in the blood vessels, leading, if left untreated, to a significant deterioration in vision or blindness.
This pathology cannot occur on its own, therefore in scientific medical circles it is called not a disease, but a symptom.
The mechanism of action of the disease is the gradual thinning of the walls of the blood vessels that penetrate the bottom of the eye. Over time, necrosis covers the affected tissue. The nutrition of the tissues of the eye membranes deteriorates and oxygen starvation occurs.
Dead cells or a detached portion of the retina cannot be returned to its original healthy state. But with proper treatment and prevention, it is possible to stop the process, preventing it from spreading. During the examination, the ophthalmologist sees that the vessels are narrowed or dilated, tortuous or wrapped in loops. It depends on the underlying cause of eye angiopathy.
Causes of retinal vascular angiopathy
The modern rhythm of life steadily leads to the development of various diseases of the cardiovascular system. Basically, they are the precursors of fundus vascular angiopathy.
- The presence or tendency to thrombosis.
- Low or high blood or intracranial pressure.
- Vasculitis (inflammation of blood vessels).
- Diabetes.
- Postural distortions.
- High cholesterol content, leading to clogging of the lumen of blood vessels with atherosclerotic plaques.
- Hereditary heart or vascular diseases.
- Natural changes observed in older or younger people. In the latter, angiopathy occurs due to hormonal changes and changes in all body systems.
- Eye injury, traumatic brain injury, or sudden strong compression of the chest area.
- Obesity.
- Pregnancy period.
- Cervical osteochondrosis.
Predisposing factors
- In addition to the reasons due to various injuries and diseases, there are a number of factors that increase the chance of developing pathology.
- These include work in hazardous industries, radiation, severe environmental pollution, regular excessive load on the organs of vision, long-term use of certain medications that have a toxic effect on blood vessels, and smoking.
- This category of the population should regularly undergo preventive examinations by an ophthalmologist in order to identify angiopathy at an early stage.
Kinds
Depending on the condition causing angiopathy, seven main types of pathology are distinguished.
- Hypertensive angiopathy is observed in patients suffering from high blood pressure. Often the disease develops when hypertension is not treated. During the examination, the doctor sees noticeable arterial narrowing and venous expansion. If, under the influence of hypertensive crises, blood vessels rupture, then we are talking about hypertensive retinopathy.
- Hypotonic, respectively, with chronic low blood pressure. Blood vessels take on a convoluted shape. There is pulsation of veins, dizziness, and dependence of well-being on the weather.
- Diabetic retinopathy is typical for people with an existing diagnosis of diabetes mellitus. Changes in blood vessels occur due to their “poisoning” with metabolites of excess glucose. This type includes two subtypes - microangiopathic (damage to capillaries) and macroangiopathic (large vessels). Diabetics are 20 times more likely to go blind than those without this endocrine pathology.
- The traumatic type of pathology is a consequence of various injuries.
- Juvenile angiopathy (ILPA disease) is detected before the age of 30 years and occurs due to past infections. For example, toxoplasmosis, tuberculosis, rheumatism and others. Eye injuries, curvature of the spine, existing kidney disease, diabetes mellitus and hypertension contribute to the development of angiopathy in childhood and adolescence.
- In premature babies. Both eyes may be affected. The pathology is caused by trauma received at birth or unfavorable factors in the prenatal period.
- Angiopathy in pregnant women during pregnancy. In the first trimester, the disease is detected extremely rarely. The cause is often hypertension, gestosis, exacerbation of chronic diseases or the acquisition of new ones. If the symptom manifests itself in a mild form, it does not require therapy and goes away on its own after successful delivery within 2-3 months. If angiopathy rapidly progresses, then it is even recommended to terminate the pregnancy for medical reasons; in the later stages, a cesarean section is indicated for the safe extraction of the fetus and to preserve the mother’s vision.
Symptoms of angiopathy
People usually seek help with retinal angiopathy in the later stages. Since at the beginning of the disease a person either does not feel the manifestations of the disease at all, or writes them off as banal fatigue after a working day.
- Severe or mild frequent headaches.
- Sore eyes.
- Discomfort in the eyeballs, a feeling of pressure on them, pain, tingling, pulsation.
- Deterioration of vision, manifested in weakening of lateral vision, blurriness, loss of certain zones, objects located at a long distance become difficult to distinguish.
- The appearance of bright or white spots, circles, flashes and floaters.
- Nosebleeds.
- Sensation of enlargement of the eyeball.
- Some patients experience hematuria and pain in the lower extremities.
Clinical manifestations are observed both regularly and periodically. It depends on the degree of neglect of the disease and individual characteristics.
Stages of symptom development
At the stage of development, pathology caused by hypertension is divided. It is impossible to determine the degree by external examination of the eyeball. This can only be done by an ophthalmologist when examining the fundus.
- Blood vessels acquire tortuosity and noticeable differences from each other - some become narrowed, while others become dilated. The diameter of the blood vessel along its entire length is not the same.
- The fundus turns pale, and vascular damage progresses, their tortuosity increases significantly.
- The diameter tapers so much that it resembles a copper wire. Blood clots and hemorrhages are observed.
- The most severe condition is angiopathy. White spots are visible on the fundus. The optic nerve is swollen, the retina is covered with a network of hemorrhages.
Diagnosis of angiopathy, code according to ICD 10
To make this diagnosis it is necessary:
- Anamnesis collection.
- Visual and instrumental examination of the fundus by an ophthalmologist under a microscope. Drops are pre-dripped for permanent expansion of the icon.
- Ultrasound scanning combined with Doppler or duplex examination of blood vessels, measuring blood flow velocity.
- X-ray using a contrast agent to detect vascular patency.
- MRI.
ICD 10 code for retinal angiopathy is H35.
For greater success of treatment, it is necessary to identify the main cause of the described symptom and simultaneously treat this disease.
Treatment of retinal angiopathy in adults and children
Treatment of angiopathy involves an individual approach to each patient. Therapy is prescribed taking into account personal characteristics and is initially aimed at eliminating the factors that caused this complication. That is why not only an ophthalmologist, but also other necessary specialists take part in the treatment of a patient.
Drug therapy
- Agents that improve blood flow, increase microcirculation, strengthen the membranes of blood vessels and reduce their permeability. Actovegin, Cavinton, Parmidine, Vazonit, Pentoxifylline, Piracetam, Arbiflex, Calcium Dobesilate.
- Vitamin complexes with a high content of B, E, P, C.
- Drugs that reduce the risk of thrombosis. Lospirin, Dipyridamole, Ticlopidine, Acetylsalicylic acid.
- Medicines in the form of eye drops prescribed to supplement vitamins or improve blood microcirculation and strengthen blood vessels. Taufon, Anthocyan forte, Emoxipin.
- Mandatory treatment of injuries, increased or decreased blood pressure, osteochondrosis, diabetes, normalization of weight and other initial causes.
- A course of drug treatment is usually carried out at least a couple of times a year, but according to individual indications, more frequent medication use is possible.
- Physiotherapy.
- Acupuncture.
- Laser.
- Magnetic therapy.
Treatment of angiopathy with folk remedies
Alternative therapy, traditional medicine, is quite active in the treatment of angiopathy and, due to this, is widely used. Medicinal herbs are used in the form of infusions and decoctions. But before using a specific product, it is recommended to consult with your doctor to prevent the condition from worsening.
Herbal tea infusions are used:
Cornflower. Bird knotweed. Birch buds. Dill and caraway seeds. Immortelle. Valerian. Melissa.
- Horsetail
- Yarrow.
- Rowan.
- It is also very important for diabetes mellitus, hypertension - the most common causes of ophthalmological pathology, to follow a diet with reduced carbohydrates, control over blood sugar, and extra pounds.
Chamomile. Hawthorn. Currant. St. John's wort.
Treatment of retinal angiopathy with laser
The use of laser is quite widespread in the treatment of eye diseases. Laser coagulation involves two types - panretinal and focal.
- Panretinal involves applying up to two thousand special dots to the retina (with the exception of the yellow area). Thanks to this, the retina becomes less in demand for oxygen, and vessels damaged by the disease do not lead to its detachment. At the same time, oxygen supply to the macula increases, and the patient’s vision improves.
- Focal is used for more severe damage to the organs of vision, when macular edema is observed. The essence of the method is to seal damaged vessels.
How to treat retinal angiopathy with injections
Injections of drugs into the eye area are the preferred method, thanks to which angiopathy in some forms can be cured. Thanks to modern techniques, this procedure is characterized by minimal trauma and painlessness.
Dexamethasone and Ranibizumab are injected into the vitreous. They eliminate swelling and create favorable conditions for the formation of new blood vessels.
Retinal angiopathy can irreversibly leave a person without the ability to see; if left untreated, it leads to the development of cataracts and glaucoma, but with timely seeking help from medical specialists, it is possible to eliminate all unpleasant symptoms and completely restore vision.
Source: https://gp2.su/zdorove/angiopatiya-setchatki-glaza-lechenie-simptomy.html