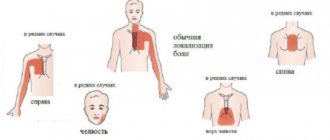
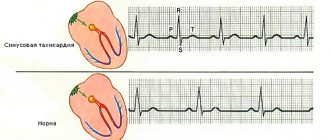
Some thyroid diseases are accompanied by the development of cardiac pathologies. One of them is tachycardia. The thyroid gland is one of the most important regulators of all processes occurring in the body, and malfunctions in its functioning negatively affect all organs and systems, but the heart muscle suffers the most.
Thyroid diseases are very common ailments in people of any gender and any age, and in order to prevent the development of severe pathologies, it is necessary to undergo a timely examination by a qualified specialist.
What can happen with hypothyroidism
The hormonal imbalance that characterizes hypothyroidism leads in almost every case to disruption of the autonomic nervous system. Almost all patients experience an increase in the tone of the vagus nerve, which is manifested by a change in the rhythm of the heartbeat. Indeed, in most cases, bradycardia develops, that is, the heart beats slower. A decrease in heart rate can lead to the development of pathology of the heart muscle, and the heart will no longer cope with its load. In this case, pain will appear in the heart area, and the heart rate will increase significantly. A feeling of lack of air, shortness of breath and heavy breathing also indicate that the internal organs do not have enough oxygen, because the blood flows to them in insufficient quantities.
Studies show that quite often patients with hypothyroidism develop hydropericardium, that is, serous effusion accumulates in the cavity of the heart sac. The frequency of its detection reaches 80% of clinical cases. This pathology aggravates the course of hypothyroidism, increases the risk of developing heart failure and in many cases leads to tachycardia.
Pain in the heart area can be caused by concomitant myocardial dystrophy, that is, a disorder of nutrition and metabolism in the tissues of the heart muscle. The main reason for this condition is the loss of sensitivity of certain groups of nerve cells to substances responsible for transmitting nerve impulses.
Against the background of hypothyroidism, the risk of developing atherosclerosis of the vessels supplying the heart and coronary disease increases. Both of these pathologies can cause pain in the projection of the heart and an increase in the rhythm of its beating.
Also, against the background of hypothyroidism, anemia often develops, that is, the number of red blood cells in the blood that transport oxygen decreases. This condition can also manifest itself as increased heart rate and a feeling of shortness of breath.
Hypothyroidism
Hypothyroidism - what it is, symptoms and treatment in women Hypothyroidism is considered the most common form of functional changes in the thyroid gland. This pathology develops due to a long-term stable deficiency of gland hormones or a decrease in their biological effectiveness at the cellular level.
The disease may not manifest itself for a long time. This is due to the fact that the process develops gradually. In mild to moderate degrees of the disease, the patient’s well-being may be satisfactory, and erased symptoms are considered to be depression, overwork, or pregnancy (if present).
In women of reproductive age, cases of the disease are 2%, in older women and men this figure increases to 10%. Thyroid hormone deficiency causes systemic disruptions in the functioning of the entire body.
What it is?
Hypothyroidism is a process that occurs due to a lack of thyroid hormones in the thyroid gland. This disease occurs in approximately one in a thousand men and nineteen in a thousand women.
There are often cases when the disease is difficult to detect, and for a long time. The reason for diagnostic difficulties is that the disease arises and develops slowly, and it is characterized by signs that make it difficult to recognize exactly hypothyroidism. Usually the symptoms are mistaken for simple fatigue, or in women for pregnancy or something else.
Causes
Hypothyroidism can be congenital, that is, the diagnosis is made to a child already in the neonatal period, sometimes before he reaches one year, and acquired - in 99% of cases.
Causes of acquired hypothyroidism:
- autoimmune thyroiditis of the chronic type (leads to irreversible hypothyroidism);
- Iatrogenic hypothyroidism - occurs during radioactive iodine therapy or when the thyroid gland is removed;
- taking thyreostatics for the treatment of diffuse toxic goiter;
- long-term acute iodine deficiency.
Congenital hypothyroidism is a consequence of congenital pathologies of the thyroid gland, disorders in the hypothalamus and pituitary gland, pathological breakdown of thyroid hormones and adverse effects on the fetus during intrauterine development - the use of various drugs by the expectant mother, the presence of autoimmune pathology.
An insufficient amount of thyroid hormones in congenital hypothyroidism leads to persistent disruption of the development of the child’s central nervous system, including the cerebral cortex, which causes mental retardation, abnormal structure of the musculoskeletal system and other important organs.
Statistics
Hypothyroidism in Russia occurs with a frequency of approximately 19 per 1000 in women and 1 per 1000 in men. Despite its prevalence, hypothyroidism is often detected late.
This is due to the fact that the symptoms of the disorder have a gradual onset and erased nonspecific forms.
Many doctors regard them as a result of overwork or a consequence of other diseases, or pregnancy, and do not refer the patient to analyze the level of thyroid-stimulating hormones in the blood.
Thyroid hormones regulate energy metabolism in the body, so all metabolic processes in hypothyroidism slow down somewhat.
Symptoms of hypothyroidism
Despite the large number of forms of the disease, the symptoms of hypothyroidism are fundamentally different only in two types: childhood (cretinism) and adults (myxedema). This is due to the action of thyroid hormones.
Their main function is to enhance the breakdown of glucose in the body and stimulate energy production. Not a single active human process can do without thyroxine and triiodothyronine.
Source: https://p-87.ru/m/gipotireoz/
Diagnostic methods
In order to determine the cause of your symptoms and choose the most effective treatment, you need to consult a specialist - a general practitioner or cardiologist. In most cases, they prescribe additional diagnostic procedures, the most common of which are electrocardiography (ECG) and ultrasound of the heart.
An ECG allows you to get an idea of the functional capabilities of the heart muscle. A cardiac ultrasound provides information about the condition of the heart muscle, the cavity surrounding the heart, and the main blood vessels.
Indicators of a laboratory blood test are also important, in which signs of anemia, an inflammatory reaction, or specific compounds indicating the presence of heart failure may be detected.
Based on the results of the examination, the doctor will be able to select symptomatic therapy or prescribe medications that improve the condition of the heart and blood vessels.
The relationship between the thyroid gland and the heart
The function of the heart is to provide blood supply to all organs and systems. It is part of the cardiovascular system and is located in the center of the chest.
The thyroid gland is located in the neck near the Adam's apple. Its function is the synthesis of triiodothyronine (T3) and thyroxine (T4). It is part of the endocrine system.
Organs belonging to different systems are connected to each other by common metabolic processes. How the thyroid gland affects the heart depends on the imbalance in the functioning of the organ and the ratio of hormones produced.
How does the thyroid gland affect the heart?
The speed of the heartbeat depends on the condition of the thyroid gland.
Hormones synthesized by the thyroid gland are vital. With their help, the functioning of the entire body is regulated, in particular, the provision of oxygen to all tissues. If a malfunction of the thyroid gland is suspected, an analysis is performed to determine the amount of hormones T3, T4, and thyroxine in the blood. With hypothyroidism, hormones are produced in insufficient quantities, which causes a person to become weak and the heartbeat to slow down.
With goiter, when the level of gland hormones is increased, the patient develops tachycardia - rapid heartbeat. High levels of hormones are detected during inflammatory processes in the thyroid gland or in the presence of neoplasms that actively synthesize hormones. Acceleration of metabolic processes in the body and contractions of the heart muscle create a state of constant stress in the body. As a result, the patient's risk of developing heart failure and sudden death increases.
What is hypothyroidism
Hypothyroidism is an endocrinological disease characterized by decreased functioning of the thyroid gland with insufficient production of its hormones.
The pathology can be asymptomatic for a long time; Sometimes nonspecific signs occur, such as weakness, fatigue, which are often attributed to overwork, poor emotional state, or pregnancy.
The prevalence of hypothyroidism in middle-aged women is 2%, in elderly women – up to 10%.
Diagnosis of tachycardia in the thyroid gland
To make a diagnosis and identify the cause of a rapid heartbeat, the following diagnostic methods are used:
- Anamnesis collection. The doctor asks the patient about the characteristics of his condition and any changes in sleep and mood.
- Monitoring pulse and blood pressure.
- ECG. Indicates the condition of the heart. It does not reveal any disturbances in the functioning of the endocrine system.
- EchoCG. With hyperthyroidism, the patient exhibits left ventricular hypertrophy.
- Ultrasound of the thyroid gland. Detects the presence of changes in the gland, inflammatory processes, and neoplasms.
- Blood test for the amount of thyroid hormones. Indicates a malfunction of the thyroid gland and explains the nature of the arrhythmia. Blood is taken for analysis in the evening, around 22:00–23:00, when the gland is most active. If blood is taken in the morning, the result will not be accurate, which may negatively affect treatment.
Return to contents
Diagnostics
To identify the causes and extent of the disease, as well as possible factors in the development of tachycardia, it is necessary to undergo a whole range of various examinations. As with any disease, the diagnosis of hypothyroidism includes clinical and additional methods.
Clinical
Clinical diagnosis includes the simplest methods carried out by the attending physician. During the conversation and examination, primary information is collected about the nature of the disease and the general condition of the patient.
| Basic Research | Methods | Information |
| Survey | Collection of complaints | Worrying symptoms are identified:
|
| History of the disease | Information about the disease is collected:
| |
| Anamnesis of life | Information about the nature of the lifestyle is obtained:
| |
| Inspection | General inspection | An assessment is being carried out:
|
| Assessment of body systems | Assessment of the functioning of body systems:
|
Additional
This section of diagnostics includes laboratory and instrumental methods. Let's take a closer look at what tests and studies are prescribed for hypothyroidism.
Laboratory
Laboratory diagnostics includes analyzes of biological fluids of the body. For hypothyroidism, various blood tests are of diagnostic value.
List of required tests
To diagnose thyroid pathology, the following tests are prescribed:
- Clinical blood test - the level of red blood cells, white blood cells, hemoglobin and ESR is of great importance;
- Biochemical blood test - the level of AST, ALT, bilirubin, urea and creatinine, cholesterol is examined;
- Blood test for thyroid hormones - the level of TSH, T3 and T4 is determined;
- Anti-TPO antibody test is a study of the level of antibodies to thyroid peroxidase (an enzyme involved in the synthesis of iodine-containing hormones).
Tests are also taken to measure the level of serum iron, prothrombin and fibrinogen; a coagulogram and a general urine test are prescribed. But they are used mainly to identify concomitant pathologies and do not carry important diagnostic information.
Preparing for the study
To obtain reliable blood test results, the following rules must be observed:
- Any blood test is taken on an empty stomach - this means that before the test it is forbidden to eat for at least 8 hours;
- 48 hours before the test, it is recommended to exclude fried, fatty foods, as well as alcohol-containing drinks from the diet;
- It is necessary to donate blood for analysis in the morning (no later than 10 a.m.);
- On the eve of the test, it is necessary to exclude excessive physical activity and emotional stress;
- It is not recommended to undergo any instrumental examinations or physical procedures before donating blood.
Unreliable blood test results can be caused by medications. Their use should be avoided 1.5-2 weeks before the study. If you are receiving ongoing therapy, discontinuation of medications must be agreed with your doctor.
Interpretation of analyzes
After blood tests, their results may have different numbers. Let's take a closer look at what these or other deviations in the analyzes mean.
A general or clinical blood test reflects the level of its main molecules:
- Reduced levels of red blood cells and hemoglobin mean that a person is anemic; the stage of the disease depends on the degree of deviation of these indicators;
- An increased level of leukocytes and ESR indicates the presence of an inflammatory process in the body.
A biochemical blood test mainly allows us to judge the functioning of the liver and kidneys:
- ALT is an enzyme found in the liver, kidneys, and to a lesser extent the heart and pancreas;
- An increase in this indicator indicates damage to the relevant organs;
- An increase in urea and creatinine indicates insufficient kidney function, and, to a lesser extent, a pathology of the endocrine system;
- An increase in cholesterol levels means a high risk of developing atherosclerosis.
The results of blood tests for thyroid hormones also vary. The following changes may be observed:
- An increase in TSH levels and normal T3 and T4 levels indicate a subclinical (asymptomatic) course of hypothyroidism; to prevent the transition to the clinical stage, it is necessary to begin therapy;
- An increase in TSH and a decrease in T4 indicate the development of a primary form of hypothyroidism;
- Reduced or normal TSH and decreased T4 diagnose the secondary form of the disease;
- A significant decrease in TSH and an increase in T3 and T4 indicate thyrotoxicosis.
Hypo- or hyperthyroidism cannot be diagnosed based on changes in the level of antibodies to TPO. Their increase indicates an autoimmune lesion of the thyroid gland.
Instrumental
Instrumental methods make it possible to obtain information about the condition of organs and make a final diagnosis. The following studies are prescribed:
- Ultrasound of the adrenal glands, heart and thyroid gland - allows you to judge the structural changes in organs and their diseases;
- ECG, Holter monitoring - studies of the electrical activity of the heart (prescribed for disorders of the conduction system of the heart, for the diagnosis of coronary artery disease);
- Thyroid scintigraphy is a radioisotope study that diagnoses structural changes in the organ; often used to determine the dynamics of treatment for both hypo- and hyperthyroidism.
To diagnose a hemorrhage or tumor of the thyroid gland, computed tomography or magnetic resonance imaging (CT or MRI) is prescribed.
Treatment of pathology
The goal of treating tachycardia in hyperthyroidism is to restore normal functioning of the thyroid gland and eliminate the cause of the arrhythmia.
It is not difficult to treat tachycardia in diseases of the thyroid gland; the main thing is to determine and then restore the level of thyroid hormones in the blood. Medicines are selected by the doctor individually, taking into account the results of the analysis and existing concomitant pathologies. Therapy is based on drugs that inhibit the function of the gland. They should be taken only as prescribed by a doctor, in strictly prescribed doses. To eliminate symptoms, the patient is prescribed medications that normalize the pulse to relieve stress on the heart muscle, and sedatives.
Folk remedies
To eliminate tachycardia caused by thyroid pathology, it is recommended to include walnuts in the diet (at least 3-4 nuts per day with 1 teaspoon of honey). During treatment, you should switch to a diet with a minimum content of animal products. Restoration of thyroid function and normalization of heart rate is ensured by infusions of hawthorn and valerian. You can prepare them yourself or purchase them at the pharmacy.
Features of treatment of tachycardia
If tachycardia is caused by a disease of the thyroid gland, then the goal of treatment is to eliminate the primary disease or relieve its manifestations.
Drug therapy
Treatment with drugs is prescribed based on the results of a hormone test. Medicines are needed to suppress organ function in order to normalize the production of hormones. In some cases, treatment is required for life.
Drugs that suppress thyroid function are prescribed exclusively by a specialist. The dosage is determined individually and calculated depending on the level of hormones in a particular patient.
A feature of the treatment of tachycardia in hyperthyroidism is a weak reaction to taking cardiac glycosides, although in the treatment of arrhythmia and the development of heart failure such drugs are included in the main drug complex.
To reduce heart rate and myocardial contractility, beta-blockers are used. More often, treatment is performed with Propranolol, Anaprilin, Inderal. These drugs are non-selective β-blockers. Such drug therapy is prescribed taking into account individual sensitivity to drugs and the results of physiological tests (performed under the control of an electrocardiogram).
In case of tachycardia due to thyroid disease, it is necessary to improve the functioning of the heart muscle. For these purposes, they resort to sedatives. A good effect is provided by herbal preparations: motherwort tincture, valerian preparations, Persen, Novo-Passit.
If tachycardia due to pathologies of the thyroid gland is accompanied by arterial hypertension, then it is advisable to prescribe calcium antagonists. Such drugs, like beta-blockers, are classified as antiarrhythmic drugs. Among the calcium antagonists, Isoptin, Finoptin, and Corinfar are most often used.
Lifestyle correction
When tachycardia occurs against the background of thyroid pathologies, it is necessary to adhere to a certain lifestyle. Several recommendations should be followed:
- eat regularly and balanced;
- overeating is prohibited, portions should be small;
- give up caffeine and strong tea;
- reduce the level of table salt in the diet;
- eliminate alcohol and smoking;
- avoid emotional overload and stress.
Rest and proper routine are important for the patient. Even light loads and overwork can trigger an attack of pathology.
Some diseases of the thyroid gland can lead to the development of tachycardia. The mechanisms of development of disorders may vary, but in any case, the patient requires competent treatment. The features of therapy can be determined only after a full diagnosis of the state of the endocrine and cardiovascular systems.
General information about the disease
Hashimoto's thyroiditis was named after the physician-scientist who described the hormonal pathology and identified its triggering factors. AIT often leads to hypothyroidism, when the thyroid gland is not able to synthesize thyroid hormones in sufficient quantities for the body. At the same time, metabolic processes are disrupted and the cardiovascular system suffers.
With the development of inflammation in tissues, as a result of autoimmune changes, the disease becomes chronic. It will not be possible to completely cure the disease, but after consultation with an endocrinologist, the patient will be prescribed treatment that can help replenish the lack of hormones and protect the body.
Risk factors for developing hypothyroidism
Theoretically, anyone can develop hypothyroidism. However, the risk of developing the disease increases if a person has precipitating factors. So, people with the following factors are at risk:
- Female;
- Age over 60-70 years;
- Family history (people who have relatives with hypothyroidism);
- A history of autoimmune pathologies (rheumatoid arthritis, systemic lupus erythematosus);
- Receiving thyreostatic therapy or treatment with radioactive iodine;
- Previous surgical interventions on the thyroid gland.
People who have an increased risk of developing hypothyroidism are recommended to undergo annual testing to determine the level of thyroid hormones in the blood.
Types of pathology
Autoimmune thyroiditis of the thyroid gland is characterized by several forms:
- Chronic . The development of this type of disease (the most commonly diagnosed) is caused by a high number of T-lymphocytes. Hypothyroidism often occurs against the background of autoimmune thyroiditis.
- During pregnancy or postpartum . It is formed during hormonal fluctuations and due to changes in the structure of a woman’s body, which is preparing for childbirth. Recovery occurs very quickly, the functions of the gland are completely restored.
- Painless . It is considered unpredictable, the course of the disease is difficult to determine, and there are no hormonal disturbances at the initial stage. To identify pathology, regular examinations are needed.
- Cytokine-induced . It develops while taking medications intended to treat liver and blood disorders. Therapy is quite complex and lengthy.
Tachycardia due to the thyroid gland: symptoms, treatment and prevention
Some thyroid diseases are accompanied by the development of cardiac pathologies. One of them is tachycardia. The thyroid gland is one of the most important regulators of all processes occurring in the body, and malfunctions in its functioning negatively affect all organs and systems, but the heart muscle suffers the most.
Tachycardia and the thyroid gland: connection and treatment methods
Thyroid diseases are very common ailments in people of any gender and any age, and in order to prevent the development of severe pathologies, it is necessary to undergo a timely examination by a qualified specialist.
How does it affect the heart?
The connection between the work of the thyroid gland and heart contractions is obvious - the speed of the heartbeat depends on its work. The thyroid gland produces hormones that are very important for the balanced functioning of the body.
With the help of thyroid hormones, not only all vital systems of the body are regulated, but also the organs are provided with oxygen.
In this regard, if there are disorders in the thyroid gland and it works at a reduced rhythm, thyroid hormones are synthesized in insufficient quantities, which provokes weakness and decreased heart rate. Conversely, when a goiter develops and the gland works at an accelerated pace, the pulse quickens, that is, tachycardia occurs.
Increased synthesis of hormones also occurs during inflammation in the gland, as well as in the presence of various formations that are hormone-dependent and produce hormones.
In a person with problems in the functioning of this endocrine organ with a rapid heartbeat, the body is constantly in a stressful state, which increases the risk of developing dangerous cardiac pathologies that can lead to death.
Increased heart rate and thyroid function are linked in this way.
The heart muscle contracts under the influence of impulses, but with thyroid diseases (in particular hyperthyroidism), hormones that are produced in large quantities generate these impulses in a random order, which naturally affects the heart. So it starts beating faster. With hypothyroidism, bradycardia develops, that is, the heart rate decreases.
It must be said that the treatment of both tachycardia and bradycardia developing against the background of thyroid diseases is not complicated, but it is important that it is prescribed by an experienced doctor.
General symptoms of thyroid dysfunction
Symptoms that may indicate a malfunction of an important endocrine organ are the following:
- increase or decrease in body weight with a normal diet and constant physical activity;
- elevated cholesterol levels;
- chilliness or excessive sweating;
- intolerance to high or low temperatures;
- rapid or decreased heartbeat;
- muscle pain;
- diarrhea or constipation;
- insomnia;
- irregularities in the menstrual cycle;
- nervousness;
- depressed and lethargic state;
- swelling;
- dry skin and hair loss.
All these symptoms are common, and it is impossible to make a correct diagnosis based on their presence alone.
There are many thyroid diseases, and each of them has its own individual symptoms. For example, with oncological processes in the gland, a person develops hoarseness in his voice, the lymph nodes become enlarged, patients complain of difficulty swallowing and pain in the throat.
With hypothyroidism, symptoms depend on the patient’s age, the degree of hormonal deficiency and the duration of the disease. In newborns, symptoms of hypothyroidism may be completely absent, and in children under 2 years of age, a clear symptom of thyroid hormone deficiency is short stature, mental retardation and learning difficulties.
Adults with hypothyroidism complain of excess weight, constipation, hair loss, a constant feeling of cold and dry skin. Women may experience reproductive dysfunction and disruptions in the menstrual cycle.
If a woman with hypothyroidism becomes pregnant, she has an increased risk of miscarriage, anemia, increased blood pressure, and possible premature birth. A child born to a woman with hypothyroidism may be delayed in mental and physical development and be underweight at birth.
As for older people, hypothyroidism is accompanied by deterioration of hearing and memory, and depression is possible. Many people mistake these symptoms for age-related changes.
The symptoms of hyperthyroidism also largely depend on the age and duration of the disease. In this case, patients develop tachycardia, nervousness, sharp weight loss, shortness of breath and sweating. In older people, hyperthyroidism is accompanied by arrhythmia and heart failure, and frequent attacks of angina are possible.
With inflammatory processes in the gland, patients experience weight gain, drowsiness, deepening of the voice and a sensation of the presence of a foreign body in the throat. As the disease progresses, hair loss, chilliness, constipation and dry skin may appear.
A goiter or an increase in the size of the gland is accompanied by difficulty breathing or problems with swallowing; patients can visually see an increase in the volume of the neck.
Diagnosis of diseases
It is imperative to understand that tachycardia can be not only a concomitant symptom of functional thyroid disorders, but also an independent and very dangerous disease. For the diagnosis to be correct, the following methods are necessary:
- Oral inquiry. The doctor asks questions about the symptoms and determines the presence of disturbances not only in the functioning of the heart, but also nervousness, weakness and psychological disorders.
- ECG. If tachycardia is caused by disturbances in the functioning of the thyroid gland, then in most cases this analysis does not reveal pathologies in the heart (in the early stages of the disease, of course).
- EchoCG. If a patient is suspected of having hyperthyroidism, this test shows the presence of left ventricular hypertrophy.
- Ultrasound of the endocrine organ can visualize the presence of formations in the gland, inflammation or other pathological changes.
- Laboratory blood tests for thyroid hormones indicate malfunctions of the organ and explain the reasons for the development of tachycardia. In this case, it is advisable to donate blood after 10 pm, since it is at this time that the gland is most active.
Traditional therapy
First of all, in case of tachycardia caused by disorders in the thyroid gland, you should give up coffee, strong tea, smoking, fatty foods, salty and spicy foods. Meals should be regular, balanced and healthy.
Overeating must be avoided, as this phenomenon can provoke unwanted attacks. It is useful to include natural honey, bran, fruits and vegetables in your diet.
It is very important to stop being nervous and experiencing emotional overload.
To lower your heart rate, you can use non-traditional treatment methods. Oatmeal juice is a very effective remedy. You need to squeeze the juice from the above-ground part of the plant and drink it half a glass 2-3 times a day. This remedy is especially indicated for those whose tachycardia is regularly accompanied by high blood pressure.
https://www.youtube.com/watch?v=hd6em9ouaqg
Hawthorn is a well-known remedy for treating heart ailments. For tachycardia caused by a malfunction of the thyroid gland, it is very useful to drink tea with these fruits. In addition, it is useful to add motherwort herb to tea.
Blue cornflower also copes well with tachycardia. For a glass of boiling water, you need to take a teaspoon of flowers, leave for an hour, then filter and drink half a glass several times a day.
Source: https://gb2zlat74.ru/zabolevaniya/tahikardiya-iz-za-shhitovidnoj-zhelezy-simptomy-lechenie-i-profilaktika.html
Symptomatic manifestations
Symptoms of the pathology vary depending on which hormone is missing. In most cases, the disease is asymptomatic and is discovered completely by chance during a routine examination.
But still, certain symptoms can be indicated:
- lethargy, depression, apathy;
- rapid loss or, on the contrary, weight gain;
- hair loss and thinning, up to alopecia;
- dry skin;
- soreness, feeling of a foreign body in the throat;
- increase in gland size;
- memory problems;
- tremor of the limbs;
- development of tachycardia, increase in heart rate even at rest;
- fatigue even after prolonged sleep or rest.
If you have several of these symptoms, it is better to consult a doctor and get the necessary tests. This will make it possible to prevent the development of the disease and begin its treatment.
Prerequisites for the development of the disease
Taking into account the fact that the hormonal system has not yet been fully studied, diseases of autoimmune origin are quite difficult to treat. But provoking factors contributing to the development of pathology are already known, these include:
- inflammation that occurs in the tissues of the gland;
- chronic infections in the body;
- uncontrolled use of medications (especially iodine in any form); it is important to understand that both excess and deficiency of iodine are dangerous;
- irradiation;
- frequent ARVI, influenza;
- the period of gestation during which the likelihood of developing the disease increases by approximately 20%.
The genetic factor is considered the main reason for the development of hypothyroidism of autoimmune origin. Therefore, if any of your close relatives have diagnosed thyroid pathologies, it is important to regularly monitor your health.
Autoimmune hypothyroidism: diagnosis
The diagnosis is made based on test results, taking into account clinical manifestations and identifying pathologies in the thyroid gland.
What research will be required:
- Blood test (T4 and TSH levels are determined). In the early stages of pathology, hormone levels may be normal, and high levels of antibodies to thyroid peroxidase and, in rare cases, to thyroglobulin may be noted. What is ATPO, you can find out from the article.
- Immunogram.
- Study of the level of autoantibodies (thyroid type).
- Ultrasonography of the gland. Prescribed if the patient has palpable nodes.
- Ultrasound of the thyroid gland.
- Biopsy.
After studying all the data, the specialist selects the most effective method of therapy.
How does the thyroid gland affect the heart?
For some thyroid diseases, the endocrinologist prescribes a consultation with a cardiologist for the patient. Many people ignore these recommendations, not knowing how the thyroid gland affects the heart. In the future, patients have to deal with pathologies of the cardiovascular system. They can be prevented by timely prevention and examinations. Diagnostics reveals abnormalities caused by defects of the thyroid gland in the early stages.
Treatment
AIT therapy takes quite a long time. Of course, it is impossible to completely cure the disease, but it is possible to stabilize the condition and control it.
Treatment is as follows:
- If the pathology is provoked by hyperfunction of the gland, beta blockers , which can prevent the development of cardiac pathologies.
- For hypothyroidism, treatment is based on taking artificial thyroid (L-Thyroxine). The dosage is constantly being adjusted; for this purpose, a TSH test is scheduled regularly (once every 3 months, in some cases the timing varies depending on the patient’s condition and hormone levels).
- To control the autoimmune system, immunomodulating correction , namely, special vaccinations (for example, against influenza) that can strengthen the immune response.
- It is possible to prescribe anti-inflammatory components .
- A specialist may prescribe glucocorticoids to stop the development of the pathology.
- When thyroid tissue grows, the tumor may become malignant. In this case, it is recommended to perform an operation to remove the entire gland or part of it .
It is important to pay attention to nutrition. For the normal functioning of the thyroid gland, 150 mcg of iodine per day is sufficient, so you need to limit foods containing it. In most cases, the patient is prescribed lifelong HRT, with only dosage adjustments.
Prevention
It is impossible to completely prevent the development of hypothyroidism. However, you can significantly reduce the risk of its occurrence using simple rules:
- Create a balanced diet enriched with minerals and vitamins, as well as iodine-containing foods;
- Avoid trauma to the thyroid gland, irradiation of the neck and upper chest;
- Promptly treat diseases that provoke hypothyroidism (obesity, endemic goiter);
- Avoid excessive physical and emotional stress.
It is recommended to undergo annual preventive medical examinations and regularly take tests for thyroid hormone levels.
What does a thyroid cough mean?
Cough with thyroid disease is mainly of a reflex nature. The thyroid gland begins to increase in size, which causes difficulty breathing and swallowing. The patient's condition worsens when he has a goiter, which puts a lot of pressure on the trachea. The body's reaction to this is a cough. This is a reflex reaction, thus clearing the airways of the presence of foreign particles. The difference is that if the cause of the cough is goiter, the condition does not improve. The person coughs constantly, the condition gradually worsens. Cough due to thyroid disease cannot be treated using conventional methods.
The role of the thyroid gland in the body
This organ performs a lot of important functions in the body, these include:
- The thyroid gland changes in size under the influence of various factors.
- It is the thyroid gland that is responsible for the body's immunity.
- When it functions normally, the proper hormones are produced.
- The state of health as a whole depends on its functioning.
Read also: Tachycardia, rapid heartbeat
Our readers recommend!
“Monastic tea” will help to effectively cure the thyroid gland in a short time and most importantly. This product contains only natural ingredients that have a comprehensive effect on the source of the disease, perfectly relieve inflammation and normalize the production of vital hormones. As a result, all metabolic processes in the body will work correctly. Thanks to the unique composition of Monastic Tea, it is completely safe for health and very pleasant to the taste.
Its functioning is directly related to the functioning of the intestines. Problems with the intestines can stimulate the growth of the thyroid gland.
What stimulates the growth of the thyroid gland?
Diagnosis of a disease caused by thyroid dysfunction is a difficult task. Sometimes this takes more than a month, since the symptoms associated with this organ can often be confused with signs of diseases of other organ systems.
- Hereditary factor.
- Body susceptibility.
- Defective processing of iodine by the intestines or its incomplete entry into the thyroid gland.
- Iodine deficiency in the body, associated with its small amount in the daily diet.
- In recent years, iodine has been added to table salt, which has had a positive effect on solving the problem. But each body has its own standards, and some may need more significant doses of iodine for the thyroid gland to function properly.
Diseases accompanied by cough are manifested by a number of symptoms
The main symptoms are described by the following list:
- A lump in the larynx itself.
- There are difficulties when swallowing food, sometimes food gets stuck.
- Attacks of severe suffocation.
Cough with an enlarged thyroid gland gradually worsens, the process is accompanied by the following symptoms:
- At the beginning of the disease, when the gland is still in the stage of change, coughing is rare, the patient does not feel any noticeable changes.
- Over time, the disease develops, leading to a significant enlargement of the thyroid gland. The cough becomes persistent, and the person notices difficulty swallowing. Some patients experience a lump in the larynx, food getting stuck when swallowing, and paroxysmal asphyxia.
- In certain cases, the enlargement of the gland becomes noticeable visually, for example, with the growth of a goiter, when the neck is deformed, the throat below becomes enlarged, as if bulging out. The cough begins to change in character, this is due to the activity of the goiter.
Iodine levels can be determined with a simple home test. The skin area should be densely smeared with iodine and absorption activity monitored. You can learn about the features of cough in thyroid diseases and the reasons for its development here:
Thyroid problems are often accompanied by indicators of heart disease. The patient feels:
- stitching pain in the region of the heart;
- tachycardia;
- arrhythmia;
- increased temper and nervousness.
The following symptoms are also characteristic:
- weakness, a person gets tired very quickly;
- frequent headaches;
- difficulties in overcoming any load.
The diagnosis can be made using an ultrasound. However, this study does not provide a complete picture of the disease, and therefore the puncture method is often used. An accurate diagnosis can only be made after a group of studies.
How is medication treatment carried out?
The first thing to do is stabilize the thyroid gland. Treatment should be focused on reducing its magnitude and killing reflexive cough. The size of the gland can be adjusted in the absence of a goiter.
An enlarged thyroid gland can also be a temporary trend, associated with some diseases. Treatment must be carried out carefully and carefully. To reduce the size and restore the natural state of the thyroid gland, the following is prescribed:
In autoimmune conditions, in which case the body begins to eliminate its cells, medications and hormones are injected into the thyroid gland (replacement therapy). The gland can secrete extremely many or few hormones. The goal of proper treatment is to restore the state of normal functioning of the organ. It is better to achieve results with the help of medications than to use replacement therapy. With this treatment, obvious symptoms and the root of the disease are eliminated.
Codeine-based medications are prescribed to suppress cough. The medicine and its derivatives are dispensed as prescribed by a doctor. Codeine is an exceptional medicine that can suppress the focus of cough to the point of complete oppression.
How to improve your health using folk remedies?
Help to relieve a cough at home:
- Milk with honey or figs.
- Radish with honey.
- Homemade lollipops made from medicinal herbs.
How dangerous is a disease accompanied by a cough?
If changes in the size of the thyroid gland are not kept in a timely manner or, if necessary, it is removed, it will occupy the entire clearing in the larynx and the person will experience asphyxia. In the case of progressive goiter, malignant changes may begin.
You cannot ignore the cough, otherwise it will flutter. Sometimes even treatment does not provide the desired result. The use of hormones can cause flatulence, weight changes, and affect the production of important enzymes. A cough is a warning sign that a person is experiencing serious changes in hormonal levels. The thyroid gland is a vital organ and efforts should be made to keep it healthy and functioning properly.
Read also: Physical therapy for tachycardia
Tachycardia with thyrotoxicosis how to treat
Version: MedElement Disease Directory
Classification
I. Severity of thyrotoxicosis
1. Light: - heart rate (HR) 80-120 per minute; - no atrial fibrillation; - no sudden weight loss; — performance is slightly reduced;
- weak hand tremors.
2. Average: - Heart rate 100-120 per minute; - increase in pulse pressure; - no atrial fibrillation; — weight loss up to 10 kg;
- performance is reduced.
3. Severe: - Heart rate more than 120 per minute; - atrial fibrillation; - thyrotoxic psychosis; — dystrophic changes in parenchymal organs; - body weight is sharply reduced;
- ability to work is lost.
It is obvious to any clinician that, using such criteria, it is quite difficult to determine the severity of thyrotoxicosis in a particular patient. For example, what is the severity of thyrotoxicosis if the heart rate is -100 beats/min, the patient has lost 15 kg, and has lost the ability to work. Another classification option, although not without drawbacks, seems to be more specific.
II. Severity of thyrotoxicosis
1. Subclinical (mild): it is established mainly on the basis of hormonal studies with a mild clinical picture.
2. Manifest (moderate): there is a detailed clinical picture of the disease.
3. Complicated (severe course). Complications: - atrial fibrillation; - heart failure; - thyrogenic relative adrenal insufficiency; — dystrophic changes in parenchymal organs; - psychosis;
- severe body weight deficiency.
Etiology and pathogenesis
The development of drug-induced thyrotoxicosis is caused by taking thyroid drugs in higher doses compared to the physiological secretion of the hormone. In clinical practice, thyroid medications are used to treat hypothyroidism, as a method of suppressive therapy for thyroid cancer or benign nodules, and, more and more recently, in the fight against obesity.
During hormone replacement therapy in the treatment of hypothyroidism, thyroid medications provide the body with the thyroid hormones it lacks. In case of goiter, they strive to achieve such a concentration of iodothyronines in the blood that would inhibit the increased secretion of TSH and thus reduce hyperplasia of thyroid tissue.
In other cases, the therapeutic effect is associated with the direct effect of thyroid drugs on the intensity of metabolic processes, which helps to reduce fat depots and increase the release of fluid from the body.
In these cases, the administration of thyroid hormones in physiological quantities does not lead to the desired effect, since they inhibit their own thyroid secretion by reducing adenopituitary and thyroid-stimulating secretion, and their concentration in the blood serum remains unchanged.
In order to achieve a therapeutic result, the dose of hormonal drugs must be slightly higher than the physiologically secreted amount.
The resulting mild hyperthyroxinemia can cause the desired deviation in the balance between liposynthetic and lipolytic processes and lead to increased mobilization of fat and water from subcutaneous tissues. When this effect is mild, it does not lead to any particular disturbances and, with sufficiently long-term use of the drugs, reduces weight and swelling.
It is not always possible to maintain the drug thyroid hormone concentration at the optimal level, either due to changes in the body’s needs, or due to an involuntary or voluntary overdose, dictated by the desire to achieve a faster therapeutic effect.
In such cases, relatively higher thyroxinemia will cause a varying degree of increase in basal metabolism, which will lead to symptoms of thyrotoxicosis: tachycardia, adynamia, increased sweating, nervousness, rapid weight loss, and others.
Such drug-induced thyrotoxicosis is not identical to diffuse toxic goiter, mainly because the patient’s thyroid gland is in complete functional rest. This is proven by the low absorption of 131I by the thyroid gland and its increase after stimulation of the TSH gland.
Due to a different pathogenetic mechanism, there are no pronounced eye symptoms, except for shine and mild retraction of the eyelids. The thyroid gland is not enlarged, and if there was a goiter before, then, as a rule, its volume decreases.
Features of the manifestation and treatment of tachycardia provoked by thyroid diseases
Heart rhythm disturbances can develop against the background of certain diseases of the thyroid gland, since it is involved in the activities of various body systems. The connection between these pathologies can be revealed through a comprehensive examination. Therapy must be prescribed based on its results.
Can thyroid disease provoke tachycardia?
Normal functioning of the thyroid gland is important for the functionality of various body systems. Organ dysfunction causes changes, including in the activity of the heart.
Heart rate is related to the condition of the thyroid gland. It synthesizes many hormones that regulate the functioning of the body and provide tissues with oxygen. Hormonal levels rise and heart rate increases. This often occurs against the background of neoplasms or an inflammatory process.
The development of tachycardia is due to the constant connection between the heart and the thyroid gland. An increase in hormonal levels is reflected in the sinus node, which is located in the right atrium.
It generates electrical impulses that cause myocardial contractions. At high hormonal levels, they reproduce chaotically, affecting the heart.
As a result, it contracts faster, the heartbeat quickens, and tachycardia occurs.
With thyroid diseases, metabolic processes can accelerate. This causes the heart muscle to contract intensely, creating chronic stress. Such changes can result in heart failure, which can be fatal.
Against the background of thyroid disease, tachycardia can be a reflex phenomenon. An increased heart rate in such cases is a reaction to an attack of severe pain.
Symptoms of tachycardia in diseases of the thyroid gland
If tachycardia is caused by disruptions in the functioning of the thyroid gland, disorders can be recognized by the following symptoms:
- heart rate exceeds normal (upper limit 90 beats) and may increase to 140 beats per minute;
- during physical and mental stress, heart contractions accelerate to 160 beats per minute and above, such indicators are a critical level;
- heart rate does not depend on body position and whether a person is sleeping or awake;
- there is pain in the chest;
- The heartbeat is felt by a person: it radiates to the neck, abdomen, head;
- dyspnea.
Such signs of tachycardia simultaneously overlap with symptoms indicating pathology of the thyroid gland. The patient can observe:
- sleep disorders;
- nervousness;
- weight loss;
- increased sweating;
- increased frequency of urination;
- diarrhea;
- menstrual irregularities.
The signs of thyroid disease are quite general, so pathology in this area can only be confirmed after a comprehensive examination. Tachycardia can be caused by various diseases of this organ, and each has its own specific symptoms.
When diagnosing tachycardia against the background of thyroid pathologies, signs of systolic hypertension are often detected.
In this case, an increase in pressure is observed only in the systolic parameter; in diastole, the indicators remain normal or change downward.
Systolic hypertension is triggered by an increase in cardiac output and stroke volume, to which the vascular system cannot adapt.
The severity of symptoms depends on the form of hyperthyroidism (hyperthyroidism):
- If it is mild, then the main manifestations are neurotic in nature. The heart rate in this case increases to a maximum of 100 beats per minute. Slight weight loss is possible.
- With moderate pathology, heart contractions can increase to 100 beats per minute. A person's body weight decreases noticeably. Weight loss in a month can be up to 10 kg.
- A severe form of hyperthyroidism is called visceropathic or arrowroot. The disease progresses to this stage in the absence of proper treatment. This form provokes persistent heart rhythm disturbances. Tachycardia can lead to atrial fibrillation and cause heart failure. This threatens accelerated breakdown of hormones and subsequent acute adrenal failure. In severe hyperthyroidism, weight loss is significant. Cachexia is possible when the body is extremely exhausted. This condition is accompanied by changes in a person’s mental state, the activity of physiological processes decreases sharply.
Source: https://baby-clinic-vozr.ru/narodnaya-medicina/tahikardiya-pri-tireotoksikoze-kak-lechit.html
Causes of thyrotoxic heart disease
The main causes of thyrotoxic heart disease are the following diseases and conditions:
- surgical interventions, operations on the thyroid gland;
- sepsis;
- radioactive iodine therapy;
- taking anticholinergic and adrenergic drugs, for example, pseudoephedrine, salicylates, non-steroidal anti-inflammatory drugs;
- chemotherapy;
- excessive use of thyroid hormones;
- diabetic ketoacidosis;
- direct trauma to the thyroid gland;
- too vigorous palpation of the thyroid gland, which can stimulate the production of hormones.
Additional factors contributing to the development of thyrotoxic heart disease:
- toxicosis of pregnancy;
- hydatidiform mole.
- placental transfer of maternal thyroid-stimulating immunoglobulin to the newborn;
- McCune-Albright syndrome with autonomous thyroid function;
- hyperfunction of the thyroid gland;
- multinodular goiter;
- tumors that promote the production of thyroid-stimulating hormone.
Autoimmune diseases can also contribute to thyrotoxic heart disease. Such diseases include:
- juvenile rheumatoid arthritis;
- Addison's disease;
- type I diabetes;
- myasthenia gravis;
- chronic lymphocytic thyroiditis (Hashimoto's);
- systemic lupus erythematosus;
- chronic active hepatitis;
- nephrotic syndrome.
Symptoms of thyrotoxic heart
The main symptoms of thyrotoxic heart disease are:
- heart failure (so-called congestive heart failure);
- a heart attack in which a blood clot blocks blood flow to the heart;
- stroke;
- peripheral arterial disease;
- sudden cardiac arrest;
- slow heart rate;
- arrhythmia.
Possible symptoms:
- high blood pressure;
- low heart rate (less than 60 beats per minute);
- increased rigidity of the walls of blood vessels;
- increased load on the heart;
- expansion of the heart muscle.
Heart problems can occur even with mild hypothyroidism (subclinical hypothyroidism).
To monitor possible symptoms, you should visit your doctor regularly and have your blood pressure checked. People with chronic diseases need to monitor cholesterol levels and blood tests. If you need to adjust your diet, you should consult a nutritionist.
Treatment of thyrotoxic heart
There are several effective treatments for thyrotoxicosis and thyrotoxic heart disease. These include:
1. Radioactive iodine.
Used as a dietary supplement. Radioactive iodine is absorbed by the thyroid gland, causing it to contract and eliminating the symptoms of thyrotoxicosis. The duration of treatment is at least 3-6 months. Since the activity of this type of iodine reduces the function of the thyroid gland, the patient must subsequently take medications that replace thyroxine.
2. Antithyroid drugs.
These medications gradually relieve the symptoms of hyperthyroidism by preventing excess hormone production. These include propylthiouracil and methimazole (Tapazole). Symptoms usually go away after 6-12 weeks of use, but treatment should last at least a year, and sometimes longer.
3. Beta blockers.
These drugs are commonly used to treat high blood pressure. They will not lower your thyroid levels, but they may reduce heart palpitations and help prevent tachycardia. Possible side effects: fatigue, headache, upset stomach, constipation, diarrhea and dizziness.
4. Surgical treatment (thyroidectomy).
Indicated during pregnancy, when you cannot take drugs that suppress the activity of the thyroid gland. In a thyroidectomy, the doctor removes most of the thyroid gland. If the parathyroid glands are also removed, treatment is needed to maintain normal blood calcium levels.
The Hormone Health Network. © 1998-2016 Mayo Foundation for Medical Education and Research. ©1996-2016 MedicineNet, Inc.
Madhusmita Misra, MD, MPH; Chief Editor: Stephen Kemp, MD, PhD.
How can 5 seconds improve your health and your life in general?
What to do if news about coronavirus keeps you awake?
How to force yourself not to touch your face often?
4 items in the supermarket that harbor the most germs
https://www.youtube.com/watch?v=5hGwrYUfaYI
How to quickly cope with stress?
How to protect yourself during a pandemic: advice from academician Boris Bolotov
Coronavirus is coming, but we are actively defending ourselves
How a smell we can't hear influences our choice of sexual partner
How does thyrotoxicosis affect the heart?
In thyrotoxicosis, there is an excess of thyroid hormones in the blood. The target organ for them is the heart. Its defeat is manifested by acceleration of the rhythm, overload of the volume of circulating blood and degenerative processes in the myocardium. Treatment should be aimed at normalizing hormonal levels, only after which cardiac medications can be used.
How does thyrotoxicosis and the heart combine?
Thyroid hormones can directly act on the myocardium, increasing the number and sensitivity of receptors for adrenaline and cortisol. As a result, a thyrotoxic heart is formed. The main disorders in this pathology are:
- high oxygen demand of the heart muscle;
- persistent increase in heart rate;
- short recovery period between contractions;
- decreased energy production by myocardial cells;
- increased pressure in the pulmonary artery system;
- minute and stroke volume are higher than normal;
- increase in systolic pressure while diastolic pressure remains unchanged;
- greater load due to an increase in the volume of circulating blood and red blood cells in it.
We recommend reading the article about dysmetabolic myocardial dystrophy. From it you will learn about the causes of the pathology and the mechanism of its development, symptoms, diagnosis and treatment.
And here is more information about atrial fibrillation.
Possible myocardial damage
The main cardiac manifestations of thyrotoxicosis are tachycardia, fibrillation of atrial muscle fibers, cardiac failure, angina pectoris against the background of metabolic disorders in the myocardium.
An excess of thyroid hormones is especially dangerous if the patient has hypertension or coronary artery disease or heart defects, since in these conditions there is a rapid progression of circulatory decompensation.
Thyroid heart palpitations or tachycardia
A frequent and full pulse is one of the characteristic signs of increased thyroid function. Sinus tachycardia is usually diagnosed. Its distinctive property is its persistence; at rest and during sleep it does not disappear completely.
At the slightest excitement, patients complain of intense heartbeat. And physical activity does not significantly change the rhythm, since the main factor in tachycardia is high sensitivity to stress hormones.
Thyrotoxic cardiomyopathy
The cause of malnutrition of the heart muscle is energy deficiency due to the increased need of myocardial cells under high load. Thyroid hormones lead to loss of ATP reserves, accumulation of fat in cardiomyocytes with loss of their contractility. Atrophic processes are accompanied by increased synthesis of connective tissue.
Cardiosclerosis in thyrotoxicosis is characterized by the rapid formation of circulatory failure, especially in elderly patients, which occurs predominantly in the right ventricular type with edema, enlarged liver and pain in the heart.
Cardiomyopathy in thyrotoxicosis
Arrhythmia in the thyroid gland
Atrial forms are typical for thyrotoxic arrhythmia, since it is in this area that most of the adrenergic receptors of the heart are concentrated. Ventricular variants of dysrhythmia develop in the later stages of the disease or with concomitant cardiac pathologies.
Initially, the manifestations are episodic, paroxysmal in nature; as it progresses, atrial fibrillation becomes recurrent or permanent. After successful treatment of the thyroid gland in young patients, sinus rhythm is completely restored without additional treatment.
Arrhythmia in thyrotoxicosis
Angina pectoris with thyrotoxicosis
An interesting feature of heart damage due to hyperfunction of the thyroid gland is the absence of atherosclerotic changes in the vessels.
This is due to the fact that thyroid hormones reduce cholesterol in the blood and the ability to form plaques on the walls of blood vessels.
Ischemic disease in such patients can occur only before the onset of thyrotoxicosis, which increases the severity of its course.
Source: https://med-perevozka.ru/narodnaya-medicina/tahikardiya-pri-tireotoksikoze-kak-lechit.html
Diagnosis of heart lesions
To establish the cause of irregular contractions or hemodynamic overload of the heart muscle, as well as confirm their connection with thyrotoxicosis, pay attention to the following signs:
- Complaints of weight loss due to increased appetite, irritability, weakness, sleep disturbance, pulse beating in the neck and abdomen, increased thirst, unstable stool.
- Appearance: shaking and sweating of the hands, shiny eyes, shifted forward (protruding), pink and moist skin, swelling of the legs and eyelids.
- When listening to the heart, the sounds are loud, 1 tone is increased, especially at the apex, and a murmur is heard during systole.
- Blood test for thyroid-stimulating hormones - increased concentrations of T3 and T4.
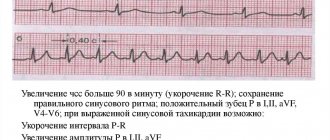
- ECG: tall and pointed P and T waves, tachycardia, atrial fibrillation, decreased ST with negative T may be observed.
- X-ray: an increase in the size of the heart due to both ventricles and protrusion of the pulmonary trunk.
- EchoCG: myocardial hypertrophy, increased diastolic volume, there may be mitral valve prolapse due to the accumulation of abnormal protein structures in its leaflets.
- Scintigraphy - a decrease in metabolic processes in the heart muscle as a manifestation of dystrophy.
ECG for thyrotoxicosis
Types of arrhythmia
| View | What's happening? |
| Ciliated | Occurs with moderate thyrotoxicosis, when the level of the hormone thyroxine increases. Heart rate reaches 100-120 beats per minute. Pathological changes in heart rate do not depend on the patient’s posture (sitting, standing or lying), physical activity (arrhythmia is stable at complete rest). This type of arrhythmia provokes heart failure. At the beginning of the disease, interruptions in heart contractions manifest themselves in attacks, then become chronic. |
| Tachycardia | Occurs in thyrotoxicosis due to increased production of catecholamine hormones. Heart rate - 90-100 beats per minute. Physical activity or rest do not affect heart rate; the increase in heart rate is stable. Due to the influence of catecholamines, cardiac impulses increase, which lead to tachycardia. |
| Bradycardia | With this rhythm disorder, the heart rate is below 60 beats per minute. The condition occurs with hypothyroidism - a decrease in the production of the hormones triiodothyronine and thyroxine. One of the functions of these hormones is to regulate the functioning of the heart. Hypothyroidism occurs due to a lack of iodine in the body. Bradycardia initially has a paroxysmal character, then becomes chronic. |
Sinus arrhythmia hypothyroidism – Hypothyroidism
Our readers successfully use ReCardio to treat hypertension. Seeing how popular this product is, we decided to bring it to your attention. Read more here...
It is known that blood pressure can increase or decrease due to the level of hormones produced by the thyroid gland.
Thus, unstable hormonal levels contribute to changes in the strength of heart contractions and vascular tone.
When the functioning of the thyroid gland malfunctions, the patient develops hypothyroidism or hyperthyroidism. Moreover, this condition is often accompanied by hypertension or hypotension.
If the hormone is produced in excessive quantities or in deficiency, then the patient’s well-being will always be unsatisfactory and many complications associated with internal organs will appear.
In addition, such patients have a reduced life expectancy. But with normalization of thyroid function, the patient’s condition improves and blood pressure normalizes.
What effect does the thyroid gland have on blood pressure?
The thyroid gland is a component of the endocrine system, the organs of which must work in harmony. Therefore, changes in the functioning of even one organ affect the rest.
It is worth noting that it is the endocrine system that coordinates pressure. Within its limits, the thyroid gland interacts with:
- pituitary gland, hypothalamus and pineal gland;
- parathyroid glands;
- adrenal glands;
- pancreas;
- ovaries and testicles;
- apudocytes scattered throughout the body.
Apudocytes are cells that regulate hormonal levels at the local level. They are present in every organ, including those that are not related to the endocrine system (lungs).
In addition, the thyroid gland is interconnected with the immune system. Therefore, changes that occur in its activity are reflected first on the adrenal glands, and then on the thymus gland.
The coordination of all glands is carried out through rapid chemical reactions. The thyroid gland is a glandular tissue; its cells can synthesize substances that have strong chemical activity.
Thyroid hormone is released into the bloodstream, and then, along with the bloodstream, is distributed throughout the body. In addition, the thyroid gland has an extensive network of lymphatic and blood vessels, so hormonal concentrations change very quickly.
Each cell in the body has specific receptors that respond to a specific hormone. Consequently, when hormonal levels change, certain physiological processes are triggered.
Follicular cells of the thyroid gland produce two types of chemically active elements:
- T3 – triiodothyronine;
- T4 – thyroxine.
T3 and T4 are substances that help adapt to unfavorable environmental conditions. When the hormone thyroxine or triiodothyronine is normal, it maintains homeostasis.
However, with diseases of the thyroid gland, their concentration greatly increases or decreases. In this case, he cannot adapt, as a result of which he is faced with various concomitant diseases. It is worth noting that for those who refuse therapy, the prognosis for recovery becomes unfavorable.
In addition, with hormonal imbalance, hypotension or hypertension can develop. Subsequently, a thyrotoxic crisis often appears against their background, which can result in death or fatal myxedematous coma.
What hormone increases blood pressure?
According to approximate data, arterial hypertension occurs in 20-30% of adults. And chronic hypertension is diagnosed in 60% of the elderly population. Of all cases of such a disease, in approximately 0.3% of patients it is caused by a malfunction of the thyroid gland.
When the hormone thyroxine and triiodothyronine are normal, its content increases only under stress, low temperature and physical activity. And if the thyroid gland produces excessive amounts of T4 and T3 for no apparent reason, then this condition is called hyperthyroidism.
Thyroid hormone can have both negative and beneficial effects on the body. Thus, it increases blood pressure due to the fact that the heart begins to contract more intensely, the lumen of the arteries narrows, and the vessels become toned.
Coordination of the functioning of the cardiovascular system and the thyroid gland is necessary in order to quickly pay attention to malfunctions in their work and provide adequate treatment. Thus, an excess of hormones increases blood pressure, provoking the development of hypertension and tachycardia.
With this condition, the following symptoms are noted:
- fainting;
- discomfort in the heart area;
- malaise;
- dizziness.
At the same time, the patient suffers from severe headaches. Taking a constant migraine often leads to complete loss of performance.
In addition, when the thyroid hormone predominates, blood rushes to the body, as a result of which its temperature increases to 36.8 ° C. Thermoregulation is necessary when the ambient temperature is low, for example in winter. It is noteworthy that during hyperthyroidism, low-grade fever is always noted.
In addition, thyroid hormone increases blood pressure, helping to activate blood supply to the brain, so it works intensively. At the same time, reactions, attention and memory are sharpened, mental processes proceed quickly, and the level of wakefulness increases.
These changes are useful when you need to respond to a conflict, stimulus, or environmental threat. However, in the case of a constant excess of hormones, such negative reactions may occur as:
- inappropriate behavior;
- irritability;
- emotional lability;
- anxiety.
Panic attacks may also appear.
Thyroid hormone also increases muscle tone, lowering the threshold for convulsive readiness. Thus, at low ambient temperatures, muscle tremors help to warm up.
If stress rather than hypothermia contributed to the increase in the concentration of T4 or T3, then the rush of blood to the muscles gives greater physical strength, for example, for running.
However, in the presence of hyperthyroidism, this mechanism leads to the development of unpleasant consequences:
- indigestion;
- myalgia;
- psychomotor overexcitement;
- convulsions.
In addition, thyroid hormone increases appetite. When metabolic processes are accelerated, a person needs to eat more food. So, after increased physical activity or hypothermia, saturating the body with food helps to restore strength, but in the presence of hyperthyroidism this does not lead to good health.
When overeating, the patient's weight does not increase, but a number of adverse reactions occur: vomiting, nausea and heartburn. Thus, if the diet is not followed, excessive food consumption along with a malfunction in lipid metabolism can lead to the appearance of atherosclerosis. In addition, the abuse of sweets in case of impaired carbohydrate metabolism contributes to the development of diabetes mellitus.
Thyroid hormones greatly influence metabolism. Failures in metabolic processes lead to early wear of the myocardium, making the walls of blood vessels more fragile.
It is worth noting that with hyperthyroidism, the likelihood of developing a heart attack, heart failure and stroke increases significantly. Therefore, to avoid death, it is necessary to carry out timely treatment of the disease.
Hormones that lower blood pressure
In some cases, in order to normalize your health, you need to lower your body temperature and blood pressure. The following factors require some adaptation:
- lack of water or food;
- heat;
- weakness after illness;
- lack of oxygen, for example, in high mountain areas;
- severe intoxication;
- great blood loss.
In such cases, the level of production of T3 and T4 decreases. Normally, this condition does not last long, so it does not harm the body.
However, with chronic hypothyroidism, the patient's health suffers significantly. Its blood pressure level decreases, vascular tone decreases, and the heart begins to work more slowly, resulting in oxygen starvation in the tissues. In the presence of hypothyroidism, a number of unpleasant complications develop - vegetative-vascular dystonia, bradycardia, angina pectoris and arrhythmia.
First of all, the brain suffers from a lack of nutrients and oxygen. At the same time, cognitive abilities and memory deteriorate.
Hypothyroidism makes a person distracted and lethargic, his performance decreases, drowsiness and weakness appear. A depressive state also occurs, which over time develops into a more significant complication - clinical depression. The most negative consequence of this condition is suicide.
In addition, untreated hyperthyroidism can lead to myxedematous coma. In its chronic course, this disease is accompanied by symptoms such as fainting, headache, dizziness and malaise. And in severe cases of the disease, disability is assigned.
Slow metabolism contributes to loss of appetite and digestive disorders. Stagnation occurs in tissues and organs, resulting in nausea, vomiting and swelling.
During hypothyroidism, body weight increases, resulting in obesity, which affects the functioning of blood vessels and the heart.
It is worth noting that with a severe form of the disease, body temperature drops to 36.4 to 34.2°C. It is this indicator that indicates hormonal imbalances, which requires immediate contact with an endocrinologist. A cardiologist should be involved in protecting the cardiovascular system.
Tachycardia (concomitant thyroid disease)
Sometimes, with excitement or slight physical activity, strong heart palpitations suddenly occur. They can occur without any reason when a person is calm. The cause of such phenomena is overexertion, stress is the first bell warning that the body is working to the limit and needs rest. But exactly the same phenomena can be a sign of a serious illness.
What is tachycardia and the causes of its occurrence
Tachycardia is an increase in heart rate under the influence of any influence in children over 7 years of age and adults at rest over 90 beats per minute. There are physiological and pathological tachycardia (under the influence of pathogenic factors).
Physiological tachycardia occurs during physical exertion, anxiety, anger, fear, at high ambient temperatures, with a lack of oxygen in the air, during a sharp transition from a horizontal to a vertical position, under the influence of certain medications, etc.
The cause of pathological tachycardia can be both heart disease and diseases of other organs. Thus, various infectious and inflammatory diseases that occur with an increase in temperature can cause increased heart rate. Tachycardia can occur reflexively with increased thyroid function, during attacks of severe pain (in any area), etc.
But most often, tachycardia occurs with various lesions of the cardiovascular system. This could be rheumatism, myocarditis, heart defects, myocardial infarction, etc.
Types of tachycardia
There are sinus tachycardia, caused by increased activity of the nervous sinus node (the main source of electrical impulses that form the normal heart rhythm), and ectopic (the source of the rhythm is located outside the sinus node in the atria or ventricles) tachycardia. Ectopic tachycardia usually occurs in the form of attacks (paroxysms) and is called paroxysmal tachycardia. If the source of the ectopic rhythm is in the atrium, then such tachycardia is called supraventricular, and if in the ventricle - ventricular.
Paroxysmal tachycardia
Manifestations of paroxysmal tachycardia depend on the duration of the attack, the location of the ectopic focus and the disease against which the attack developed.
During attacks of paroxysmal tachycardia, heart contractions are rhythmic, their frequency reaches 120-220 beats per minute. The attack begins suddenly and can last from a few seconds to several days, and sometimes weeks, and the heart rate does not change. Immediately before the attack, the patient experiences a feeling of “interruptions”, “fading” of the heart.
During prolonged attacks, patients experience general anxiety, fear and sometimes dizziness. If the heart rate is very high, fainting may occur.
Supraventricular paroxysmal tachycardia often occurs against the background of vegetative-vascular dystonia and is accompanied by such manifestations as body trembling, sweating, frequent excessive urination, etc. The heart rate with supraventricular tachycardia is higher (140-220 beats/min) than with ventricular tachycardia (130-170 beats/min). Ventricular tachycardia is most often a sign of heart disease and is more severe.
Complications of paroxysmal tachycardia
A prolonged attack of paroxysmal tachycardia can cause severe complications in the form of cardiogenic shock (a severe disorder with impaired consciousness and a sharp disruption of blood circulation in the tissues) or acute heart failure with pulmonary edema (the heart does not have time to pump blood and it stagnates in the lungs, the liquid part of the blood leaks through the walls of blood vessels, flooding the lungs). At the same time, the magnitude of cardiac output is significantly reduced, which leads to a decrease in coronary blood flow (arteries supplying blood to the heart muscle), this can lead to attacks of angina pectoris (acute short-term pain in the heart).
Treatment of tachycardia
During an attack of tachycardia, the main thing is physical and mental rest. An attack of supraventricular tachycardia can be relieved by reflex methods by irritating the vagus nerve: straining, squeezing the abdominals, holding your breath, pressing on the eyeballs, inducing gagging. If ineffective, various medications are used (for example, obzidan). In severe cases, reducing atrial stimulation is performed to restore the correct rhythm.
For ventricular tachycardia, lidocaine is most often administered. If drug therapy does not help, then electropulse therapy is performed.
Prevention of paroxysmal tachycardia
Prevention of attacks of paroxysmal tachycardia should be carried out taking into account its form, frequency and cause of occurrence. In case of rare attacks (one in several months or years), the patient is recommended to lead a healthy lifestyle (without smoking and alcohol) with the exception of physical and mental stress. For frequent attacks, sedatives and medications that eliminate irregular rhythms are used to prevent them.
The mechanism of tachycardia and other symptoms
Contractions of the heart occur due to the work of the sinus node, localized in the region of the right atrium. These impulses set the rhythm for the myocardium. In goiter, when the level of thyroxine is elevated, the frequency and order of generation of cardiac impulses is disrupted and becomes faster. With hypothyroidism, changes in heart rate are directly proportional: it can decrease to 40-50 beats per minute. This condition is called bradycardia. With tachycardia, there is a high pulse, reaching 120-130 beats per minute, long-term attacks of rapid heartbeat at night, preventing a person from falling asleep. This type of disease is difficult to treat with glycosides.
Irritability is common in people suffering from hyperthyroidism.
- slowing down or speeding up metabolism;
- arrhythmias;
- CHF (chronic heart failure);
- sweating;
- deterioration of hair and skin condition;
- diarrhea;
- vomit;
- improved appetite;
- muscle aches;
- disturbances in the functioning of the genital organs;
- irritability.
Read also: List of medications for cardiac tachycardia
Hypothyroidism is characterized by a relatively smaller list of manifestations: bradycardia, arterial hypertension and a decrease in the strength of heart contractions.
Prevention of myocardial damage
To prevent complications on the cardiovascular system due to hyperfunction of the thyroid gland, it is necessary to stabilize the secretion of thyroid hormones. If this cannot be achieved with medications, then surgery is indicated. Patients need to avoid physical and emotional overload, regularly undergo a full examination by a cardiologist and preventive courses of cardiac therapy at least 2 times a year.
Read also: Relief of supraventricular tachycardia
We recommend reading the article about ventricular extrasystole. From it you will learn about the pathology and the reasons for its development, signs and symptoms of the disease, methods of diagnosis and treatment.
And here is more information about atrial fibrillation.
Thyrotoxicosis is manifested by tachycardia, atrial fibrillation, cardiomyopathy and myocardial ischemia. This is due to increased activity of the sympathetic system and an enhanced reaction of the myocardium to its influence. The heart works under constant overload, so if treatment is ineffective, the disease is complicated by circulatory failure.
For treatment, thyreostatic drugs are used, as well as means to normalize rhythm and metabolic processes.
If arrhythmia is suspected, tests will help make an accurate diagnosis. What tests need to be taken to determine the diagnosis, besides blood?
Blockers are prescribed for arrhythmia to relieve an attack, as well as on an ongoing basis. Beta blockers are selected individually in each case; self-medication can be dangerous.
Everyone can hear the diagnosis of dysmetabolic myocardial dystrophy. Its genesis has been clearly established by doctors. If treatment is started in a timely manner, the process will be reversible.
The drug Egilok is prescribed for palpitations, for prevention after a heart attack and for many other reasons. However, compatibility is not allowed with all medications. The dosage is selected purely individually, starting with 25 mg. There are side effects.
Supraventricular and ventricular extrasystole is a heart rhythm disturbance. There are several variants of manifestation and forms: common, rare, bigeminy, polytopic, monomorphic, polymorphic, idiopathic. What are the signs of illness? How is the treatment carried out?
There are heart hormones. They influence the functioning of the organ - enhancing, slowing down. These can be hormones of the adrenal glands, thyroid gland and others.
Supraventricular tachycardia occurs in adults and children. Symptoms include sudden rapid heartbeat, dizziness, and others. ECG readings will not always reflect the problem. Relief of attacks of paroxysmal NT can be done independently, but treatment cannot be avoided in the future.
Ischemic cardiomyopathy can occur with severe heart damage. The reasons lie in lack of blood circulation. Diagnosis and treatment must be timely, otherwise the patient will die.
An adrenal tumor or pheochromocytoma has symptoms similar to other diseases. Only tests and instrumental diagnostics can accurately detect pheochromocytoma, including hypertensive crisis. The drugs are ineffective; treatment involves surgery.