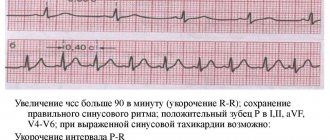
In medicine, antiarrhythmic drugs are used to normalize the rhythm of heart contractions. Such drugs are intended only to control the clinical symptoms of diseases in which the functioning of the heart muscle is impaired. Antiarrhythmics have no effect on life expectancy. Depending on the nature of changes in heart rhythm, antiarrhythmic drugs from different pharmacological groups and classes are prescribed. Their use should be long-term and under strict control of electrocardiography.
Types of drugs and their mechanism of action
Classification is carried out according to the pharmaceutical group. The mechanism of action will be different in each case.
Potassium channel blockers
The essence of the effect is to reduce the speed and intensity of potassium penetration through the heart wall into cardiomyocytes.
Thanks to such a planned disruption of the biochemical process, a partial decrease in the tone of the muscular organ is observed, while the contractility and pumping function as such does not decrease and remains at a normal, adequate level.
Attention:
Drugs of this type are not suitable for use in people with severe heart failure after a heart attack.
Their use in long courses is also not recommended, except in some cases.
Calcium channel blockers
They have an identical effect, only the rate of penetration through the cell membranes of cardiomyocytes is reduced not by potassium, but, as the name of the group suggests, by calcium.
These drugs are effective against sinus tachycardia and some supraventricular arrhythmias, but are completely unsuitable for stopping dangerous forms of the disorder: multiple extrasystoles, ventricular fibrillation.
In this case, there is a parallel drop in blood pressure, which can lead to collapse and death. This is the main disadvantage of calcium channel blockers in the context of combating arrhythmias.
The drugs in the previous group have zero ability to lower blood pressure, which gives them a strong advantage.
Beta blockers
They inhibit the sensitivity of special receptors located in the heart. For this reason, cardiac structures become less sensitive to the effects of adrenaline, which in some cases is the culprit in increasing the heart rate.
Concomitant use of beta blockers and other medications is possible.
Anesthetic drugs
Used to combat the most dangerous forms of cardiac activity disorders.
These antiarrhythmics reduce the sensitivity of the myocardium and disrupt the conduction of impulses from the sinus and atrioventricular nodes.
On the one hand, this allows you to achieve a high-quality effect. On the other hand, it makes it impossible to use with minimal disruption of the His bundle and other structures of the conduction system.
Mixed medications
There are other medications that cannot strictly be classified as antiarrhythmics, or they are of mixed origin.
These, for example, include herbal medicines (not to be confused with dietary supplements, which are not considered medicines at all) or cardiac glycosides, which simultaneously increase the pumping and contractile function of the myocardium and indirectly combat heart rate disorders.
Regardless of the situation, treatment is selected strictly by a cardiologist. This is his prerogative.
Attention:
Taking antiarrhythmics, especially cardiac glycosides, on your own is a huge risk to life. The probability of getting it right with the drug is slightly greater than winning the main prize in the lottery.
Drugs used for tachyarrhythmias and extrasystole
Drugs used for tachyarrhythmias and extrasystoles are divided into 4 main classes, differing in their mechanism of action:
I - sodium channel blockers;
II - β-blockers;
III - potassium channel blockers (drugs that increase the duration of the action potential);
IV - calcium channel blockers.
In addition, potassium preparations, cardiac glycosides, magnesium sulfate, adenosine, etc. are used as antiarrhythmic drugs for tachyarrhythmias and extrasystoles.
Basically, these drugs have an antiarrhythmic effect due to their effect on the phases of action potentials generated in various parts of the conduction system of the heart. Action potentials in different parts of the heart are formed by different ionic currents and differ in the duration and severity of the phases.
Action potentials generated by Purkinje fibers consist of the following phases (Fig. 19.2):
Phase 0 (“zero” phase) is the phase of rapid depolarization of the cell membrane caused by the incoming current of sodium ions through “fast” sodium channels.
The speed of the “zero” phase determines the conductivity of cardiomyocytes. The shorter the phase 0, the higher the speed of impulse propagation along the Purkinje fibers.
Phase 1 - the early repolarization phase is caused by the release of K+ ions from the cell along an electrochemical gradient through open potassium channels.
Phase 2, the plateau phase, is associated with the slow entry of calcium ions into the cell, which during a certain period slows down the repolarization process. This phase ends with the closure of calcium channels.
Phase 3 is the phase of late repolarization caused by the release of K+ ions from the cell. During this phase, the cell membrane potential reaches its initial level - the resting potential (90 mV - in Purkinje fibers).
In the period between phase 0 and until the end of phase 2 and in the initial period of phase 3, cells do not respond to excitatory stimuli (absolute refractory period). During this period of time, even a fairly strong stimulus does not cause the spread of excitation. The period during which spreading excitation cannot be generated is defined as the effective refractory period (ERP). The magnitude of the effective refractory period depends on the duration of the action potential and is therefore determined by the speed of the 3rd phase (repolarization speed).
Phase 4 is the phase of slow diastolic depolarization. Pacemaker cells in this phase are characterized by slow spontaneous depolarization, which is caused by a slowly increasing incoming sodium current (and only to a small extent by incoming calcium current) and a gradual decrease in outgoing potassium current. As a result, the membrane potential of the wall
but reaches a threshold level. Automaticity depends on the speed of slow diastolic (spontaneous) depolarization (the higher the depolarization speed, the higher the automaticity).
There are distinct differences between the action potentials generated in the Purkinje fibers, sinoatrial node, and atrioventricular node.
In the sinoatrial node, membrane depolarization in phase 0 and phase 4 is associated with the entry of Ca2+ ions into cardiomyocytes. In the atrioventricular node, membrane depolarization in phase 0 and phase 4 of the action potential is caused by the entry of both Ca2+ and Na+ ions into the cell.
Class I - sodium channel blockers (membrane stabilizing agents)
Class I drugs are divided into three subgroups: IA, IB, 1C, differing in their effect on the phases of the action potential. Class IA drugs increase the duration of the action potential (prolong repolarization) and ERP, class IB drugs shorten the action potential and ERP, and 1C drugs have little effect on these parameters.
Class IA
Quinidine, procainamide chloride (Novocainamide), disopyramide (Ritmodan, Ritmilen).
Quinidine is an alkaloid from cinchona bark (a dextrorotatory isomer of quinine). Quinidine blocks fast sodium channels of the cell membrane and therefore reduces the rate of fast depolarization in phase 0, as a result of which it reduces the conductivity of Purkinje fibers, contractile myocardium and, to a lesser extent, atrioventricular conduction. By blocking sodium channels, quinidine slows the slow spontaneous depolarization in phase 4 and therefore reduces automaticity in Purkinje fibers.
Quinidine blocks potassium channels, as a result of which it slows down the repolarization process (the release of K+ ions from the cell) and increases the duration of the action potential. This leads to a lengthening of the effective refractory period.
Quinidine has virtually no direct effect on the sinoatrial node, in which depolarization in both phase 0 and phase 4 is determined by the entry of Ca2+ ions, but it inhibits the transmission of excitation from the vagus nerve to the heart (anti-cholinergic effect) and thus can cause an increase in automaticity of the sinoatrial node and moderate tachycardia. In therapeutic doses, quinidine only moderately reduces the speed of excitation through the atrioventricular node.
Quinidine reduces myocardial contractility and dilates peripheral vessels (blocks α-adrenergic receptors), resulting in a moderate decrease in blood pressure.
Quinidine is effective for both ventricular and supraventricular cardiac arrhythmias. It is prescribed orally for constant and paroxysmal
small forms of atrial fibrillation, paroxysmal tachycardia, extrasystole.
In medical practice, quinidine is used in the form of quinidine sulfate, prescribed orally. Quinidine is almost completely absorbed from the gastrointestinal tract. Bioavailability averages 70-80%. The maximum concentration in the blood plasma is achieved after 2-3 hours. Binding to blood plasma proteins is 60-80%. Metabolized in the liver, excreted by the kidneys (about 20% unchanged); t)/2 is 6-7 hours. Renal excretion of the drug increases when the urine reaction changes in the acidic direction.
Side effects of quinidine include decreased myocardial contractility, arterial hypotension, intracardiac block; nausea, vomiting, diarrhea, dizziness, ringing in the ears, hearing impairment, vision impairment; thrombocytopenia. In some patients (on average 5%), quinidine, like many other antiarrhythmic drugs, has an arrhythmogenic effect (ventricular disturbances are possible).
Procainamide has a similar effect on electrophysiological parameters of the heart as quinidine. Unlike quinidine, it reduces myocardial contractility less, has less pronounced anticholinergic properties, does not block α-adrenergic receptors, but has a moderate ganglion-blocking effect. Just like quinidine, procainamide is used for ventricular and supraventricular tachyarrhythmias, extrasystole. The drug is prescribed not only orally, but also intravenously (if necessary to quickly achieve an effect).
When taken orally, procainamide is absorbed more rapidly than quinidine. Bioavailability - 75-95%, slightly binds to blood plasma proteins (15-20%). Metabolized in the liver to form an active metabolite - N-acetylprocainamide. Based on the rate of metabolism of procainamide, there are slow and fast “acetylators”, which significantly differ in the duration of action of the drug. Procainamide is excreted by the kidneys unchanged and in the form of metabolites. The active metabolite is excreted more slowly than procainamide; if renal function is impaired, it can accumulate in the body.
Side effects - decrease
blood pressure (due to ganglionic blocking effect), conduction disturbances; nausea, vomiting, diarrhea, convulsions, allergic reactions manifested in the form of fever, joint and muscle pain, skin rash and, less commonly, a syndrome similar to systemic lupus erythematosus, agranulocytosis; neuropsychic disorders are possible.
Disopyramide has a pronounced antiarrhythmic effect, its properties are similar to quinidine. Reduces myocardial contractility and has pronounced m-anticholinergic properties.
Indications for use are the same as for quinidine; the drug is administered orally. Well absorbed from the intestines (bioavailability of about 80%), binds to blood plasma proteins, and is metabolized in the liver. Excreted mainly by the kidneys (t1/2 6-8 hours).
Side effects - a significant decrease in myocardial contractility, atrioventricular block, arrhythmogenic effect. Due to the pronounced m-cholinergic blocking activity, side effects such as dry mouth, accommodation paralysis, constipation, and urinary retention occur.
Class IB
Lidoc aina hydrochloride (Xycaine, Xylocaine), mexiletine (Mexitil), phenytoin (Difenin).
Class IB drugs reduce conductivity to a lesser extent compared to Class IA drugs; they reduce the duration of the action potential, as a result of which the effective refractory period is shortened.
Lidocaine is used as a local anesthetic and antiarrhythmic agent. Both effects are associated with blockade of sodium channels in cell membranes. Lidocaine reduces conductivity in Purkinje fibers and reduces the automaticity of Purkinje fibers and working myocardium. Suppresses ectopic foci of excitation. Unlike quinidine, lidocaine does not lengthen, but shortens the action potential and the effective refractory period. Lidocaine is prescribed only for ventricular arrhythmias (tachyarrhythmias, extrasystoles). It is the drug of choice for ventricular arrhythmias associated with myocardial infarction. Since lidocaine has low bioavailability when administered orally, it is administered intravenously (drip). Binds to plasma proteins (50-80%), metabolized mainly in the liver. Quickly disappears from blood plasma; t—
about 2 hours. With liver pathology, the rate of lidocaine metabolism decreases.
Lidocaine is well tolerated, but side effects are possible: central nervous system disorders (drowsiness, confusion, convulsive reactions), arterial hypotension, decreased atrioventricular conduction.
Mexiletine is a structural analogue of lidocaine, effective when taken orally. Mexiletine is effective when taken orally (bioavailability is 90-100%) and has a long-lasting effect. The drug can also be administered intravenously. Used for ventricular arrhythmias. Side effects - bradycardia, arterial hypotension, impaired atrioventricular conduction, possible arrhythmias, nausea, vomiting, neurological disorders.
Phenytoin was synthesized as an anticonvulsant (anti-epileptic) drug. Then the drug was found to have antiarrhythmic activity, similar in electrophysiological characteristics to the activity of lidocaine. Phenytoin is used for ventricular arrhythmias, including those caused by cardiac glycosides. Phenytoin is administered orally and intravenously (in the form of sodium salt).
Phenytoin is absorbed slowly from the gastrointestinal tract and binds to plasma proteins in the blood (80-96%); metabolized in the liver, metabolites are mainly excreted by the kidneys. Due to delayed excretion from the body (X
- more than 24 hours) cumulation is possible.
With intravenous administration of phenytoin, acute reactions in the form of hypotension and arrhythmias are possible. With prolonged oral administration, side effects occur on the part of the central nervous system (ataxia, nystagmus, confusion), hematopoietic organs, and gastrointestinal tract. The drug causes gum hyperplasia.
Class 1C
Propafenone (Ritmonorm), flecainide, moracisine hydrochloride (Ethmosin), etacizine.
Drugs of this class reduce the rate of depolarization in phase 0 and phase 4 due to inhibition of sodium ion transport and have little effect on the duration of the action potential and the effective refractory period.
Since these drugs have pronounced arrhythmogenic properties (arrhythmias occur in 10-15% of patients), they are used mainly for rhythm disturbances that are refractory to the action of other antiarrhythmic drugs.
Propafenone is a typical class 1C antiarrhythmic drug; in addition to pronounced blockade of sodium channels, it has some β-adrenergic blocking activity and weakly blocks calcium channels. It is used for both ventricular and supraventricular arrhythmias when other antiarrhythmic drugs are ineffective. Administered orally and intravenously.
When administered orally, propafenone is well absorbed from the intestine, but undergoes extensive metabolism during the first passage through the liver (bioavailability varies from 4 to 40%). More than 90% of patients belong to the phenotype of rapid metabolism of propafenone, and about 10% - to the phenotype of slow metabolism. Differences in metabolic rate are associated with genetic factors. During the metabolism process, 2 pharmacologically active substances are formed.
Side effects include: nausea, vomiting, constipation, dry mouth, sleep disturbance, bradycardia, bronchospasm. The drug has pronounced arrhythmogenic properties, and therefore it is used in case of ineffectiveness or intolerance of other antiarrhythmic drugs.
Flecainide, due to the blockade of sodium channels, reduces the rate of rapid depolarization (phase 0), as a result of which it slows down conduction in the Purkinje fibers, in the atrioventricular node, and the His bundle. It has little effect on the rate of repolarization and slightly reduces myocardial contractility. Used in the form of flecainide acetate for ventricular arrhythmias in case of ineffectiveness of other antiarrhythmic drugs. Administered orally, sometimes intravenously. Side effects include nausea, headache, dizziness, and blurred vision. The arrhythmogenic effect of the drug was noted in 5-15% of cases.
Moracizine is a phenothiazine derivative, a drug of mixed type of action, exhibiting the properties of sodium channel blockers of three classes 1C, IB, 1A. Moracizine inhibits conduction in the atrioventricular node, His bundle and Purkinje fibers, and has virtually no effect on the rate of repolarization. Myocardial contractility does not change significantly. Moracizin is effective for both ventricular and supraventricular arrhythmias; due to its arrhythmogenic properties, it is used for arrhythmias refractory to other antiarrhythmic drugs. The drug can be administered orally and intravenously.
Side effects: arrhythmogenic effect, palpitations, headache, increased fatigue and weakness, diarrhea, etc.
Ethacizine is close in chemical structure to moracizine and blocks not only sodium but also calcium channels. Indications for use are the same as for moracizine. The drug is prescribed orally and intravenously. Side effects
the effects are more pronounced and occur more often than with moracizine (especially when administered intravenously).
Class II - β-blockers
For the treatment of arrhythmias, both non-selective β1, β2-blockers (propranolol, nadolol, etc.) and cardioselective β1-blockers (metoprolol, atenolol, etc.) are used (see section 9.2.1. Blockers). β-Adrenergic blockers eliminate the influence of sympathetic innervation and adrenaline circulating in the blood on the heart, as a result of which they reduce:
- automaticity of the sinoatrial node and heart rate;
- automaticity and conductivity of the atrioventricular node;
— automaticity and conductivity of Purkinje fibers. β-Adrenergic blockers are used for supraventricular tachyarrhythmias and ex-
racism, they are effective for ventricular extrasystoles associated with increased automaticity. When using β-blockers, undesirable effects occur such as decreased myocardial contractility, bradycardia, increased bronchial and peripheral vascular tone, and increased fatigue.
Class III - drugs that slow down repolarization (potassium channel blockers)
Amiodarone (Cardiodarone, Cordarone), bretylium tosylate (Ornid), sotal o l (Loritmic, Darob, Sotalex).
Amiodarone is an analogue of thyroid hormones (acts on receptors for thyroid hormones) and contains iodine in its structure. Amiodarone is a drug of mixed type of action: it blocks potassium, as well as sodium and calcium channels, in addition, it has non-competitive β-adrenergic blocking activity. By blocking potassium channels, amiodarone reduces the rate of repolarization of cardiomyocyte membranes both in the conduction system of the heart and in the working myocardium, as a result of which it prolongs the action potential and the effective refractory period of the atria, atrioventricular node and ventricles. Of great importance in the antiarrhythmic effect of amiodarone is the reduction in automaticity, excitability and conductivity of the sinoatrial and atrioventricular nodes.
Amiodarone is effective in almost all forms of tachyarrhythmias and extrasystole. In addition, it reduces myocardial oxygen demand (due to blockade of β1-adrenergic receptors of the heart) and dilates coronary vessels (due to blockade of α-adrenergic receptors and calcium channels), and therefore has an antianginal effect in angina pectoris. The drug is administered orally and, if necessary, intravenously.
When taken orally, the drug is absorbed slowly and incompletely. The degree of absorption varies from 20 to 50%. Binds to plasma proteins by 96%. The therapeutic effect develops slowly (several weeks are required to achieve maximum effect). When administered intravenously, the effect is immediate
It works quickly - within 1-2 hours. The drug accumulates in the tissues. Metabolized in the liver to form an active metabolite - N-desethylamiodarone. It is excreted slowly, mainly by the intestines: t1/2 is biphasic: the initial phase is about 10 days, the terminal phase can be up to 100 days or more. Amiodarone inhibits microsomal enzymes in the liver that metabolize many drugs, so the doses of drugs such as quinidine, procainamide, digoxin, warfarin should be reduced.
Side effects of amiodarone: sinus bradycardia, decreased myocardial contractility, arrhythmogenic effect, difficulty in atrioventricular conduction, neurological symptoms (tremor, ataxia, paresthesia), dysfunction of the thyroid gland (hypo- or hyperthyroidism), fibrotic changes in the lungs (possibly fatal), liver dysfunction, lipofuscin deposits in the cornea of the eye, in the skin (skin coloration in a gray-blue color; skin photosensitivity (sunlight should be avoided), etc.
Sotalol is a racemic mixture of two stereoisomers (L- and D-). Both isomers block potassium channels, slow down the repolarization of the cell membrane and increase the duration of the action potential and, as a result, the effective refractory period in all parts of the heart. In addition, sotalol non-selectively blocks β-adrenergic receptors. Sotalol is classified as a drug of mixed action ( Class II/IH). Due to the blockade of β-adrenergic receptors, sotalol inhibits the automaticity of the sinoatrial node, reduces the automaticity and conductivity in the atrioventricular node and other parts of the conduction system of the heart. Used for ventricular and supraventricular arrhythmias, administered orally and intravenously.
It is well absorbed from the gastrointestinal tract (bioavailability is 90-100%). Taking the drug together with dairy products leads to a decrease in its bioavailability. Not bound by blood plasma proteins. Excreted unchanged by the kidneys. t1/2 - 7-12 hours. When taken orally, the drug begins to act after 1 hour, the duration of the effect is 24 hours.
Side effects are associated with non-selective (β-adrenergic blocking activity (see section 9.2.1. “Adrenergic blockers”).
Bretylium is a quaternary ammonium compound, increases the duration of the action potential and lengthens the effective refractory period, has sympatholytic properties (impairs the reuptake of norepinephrine by adrenergic nerve endings). Used for ventricular arrhythmias refractory to other antiarrhythmic drugs in the form of bretylium tosylate. Since the drug is poorly absorbed from the gastrointestinal tract, it is administered intravenously or intramuscularly. It is excreted mainly by the kidneys unchanged. t1/2 - 6-10 hours. Due to the sympatholytic effect, it causes arterial hypotension (orthostatic hypotension is possible).
Potassium channel blockers
They disrupt the conduction of ions of the same substance in the heart. Due to this, a drop in heart rate is observed, excitation processes in the cardiac structures are inhibited, and impulse conduction is disrupted, which is especially important when used in patients with an excessive increase in cardiac activity.
At the same time, this limits the scope of use of such medications and requires careful attention to the physiological indicators of the patient’s body.
An important difference between potassium channel blockers is their lack of ability to affect blood pressure.
Almost the only medicine in this group is Amiodarone.
It is used in the vast majority of cases, as part of the routine treatment of chronic pathologies that are accompanied by disturbances in heart rate and in emergency conditions within the framework of resuscitation.
Has wide variability in the speed of the effect:
- When administered by injection, it acts quickly and is eliminated just as quickly, which makes it an ideal option for relieving acute conditions.
- In tablet form, the effect begins later, but the medication also works longer.
Amiodarone has minimal side effects and is relatively well tolerated. Long-term use is possible, but with great caution.
Because cardiovascular pathologies tend to constantly progress. At a certain point, taking it can become dangerous. Then the therapy is reconsidered.
An additional beneficial effect is the ability to reduce myocardial oxygen demand.
Among the indications for use:
- ventricular and supraventricular tachycardia;
- prevention of ventricular fibrillation (including after cardioversion),
- supraventricular arrhythmias with ineffectiveness or impossibility of other therapy, especially associated with WPW (Wolff-Parkinson-White) syndrome;
- atrial fibrillation and atrial flutter;
- atrial and ventricular extrasystole.
There are several trade names: Aritmil, Cordarone.
There are no fundamental differences between them: the form and concentration of the active substance are identical. Is that the number of tablets in the package is not the same. The selection of medication is carried out by the doctor at his own discretion.
Prompt solution to the problem
In some cases, atrial fibrillation can be treated with surgery. This intervention is safe and less traumatic. It is carried out in specialized cardiology centers.
If maintaining sinus rhythm is ineffective or it is impossible to slow down the rhythm with persistent atrial fibrillation, radiofrequency ablation (RFA) of the atrioventricular junction is performed. Through this node, irregular signals are transmitted from the atria to the ventricles in the heart. After it is “cauterized” using a catheter inserted through a vein, the flow of impulses stops.
In order for the chambers of the heart to contract normally, the patient is immediately fitted with a pacemaker - a miniature device that sets the rhythm of heart contractions. This is a very effective way to treat atrial fibrillation.
Radiofrequency ablation (RFA) for atrial fibrillation
In addition, modern research centers are developing catheter and surgical ablation techniques that destroy foci of chaotic excitation in the atria. In this case, installation of a pacemaker is not required.
Calcium channel blockers
Antiarrhythmic drugs of this group affect the heart rate indirectly.
The penetration of ions of the same substance into cardiomyocyte cells is disrupted, which contributes to a decrease in excitation and a decrease in the intensity of impulse conduction.
At the same time, some of the drugs in this group also effectively suppress the penetration of calcium ions through the vascular wall, which leads to a decrease in blood pressure (tonometer reading).
Attention:
The antihypertensive effect is inherent to one degree or another in all calcium channel blockers. This result should be taken into account when prescribing therapy.
Today, there are 4 generations of medications, if we consider specific names that could be effective.
Verapamil
It is considered an ideal option for the treatment of supraventricular forms of arrhythmia, especially complicated by elevated blood pressure.
It is not used to eliminate other types of disorders due to the lack of beneficial effects.
Indications for use:
- paroxysmal supraventricular tachycardia;
- chronic form of atrial flutter and fibrillation;
- supraventricular extrasystole.
Verapamil is available in injection and tablet forms, the effectiveness of each depends on the specific clinical case.
Parenteral (intravenous) administration is practiced in emergency situations to quickly achieve results.
There are several analogues of the drug. They are identical in pharmacological properties, therefore interchangeable. For example, "Phenoptin".
Diltiazem
If Verapamil has a rather narrow focus and is used primarily for the treatment of heart pathologies and relief of arrhythmias, then Diltiazem is considered a universal, intermediate remedy.
Therefore, it can have unpredictable consequences if used incorrectly. A clear selection of dosage and regimen is necessary so as not to cause harm.
This means that patients with arrhythmias are recommended to stay in the hospital for surgical correction of therapy or regularly visit a cardiologist, which is less preferable.
Diltiazem effectively treats supraventricular arrhythmias. It is mainly prescribed for systematic treatment, because it has a relatively mild effect.
- Phenylalkylamines (Verapapil) are most often used in the treatment of cardiac pathologies.
- Representatives of benzodiazepines (which includes the already mentioned Diltiazem) are prescribed less frequently.
It makes no sense at all to use dihydropyridines (Amlodipine and analogues) as antiarrhythmics.
They act primarily on blood vessels; their main area of application is the treatment of arterial hypertension.
Beta blockers
The basis of the pharmaceutical effect is the ability to reduce the sensitivity of cardiac structures to adrenaline.
This is a temporary effect, but in many cases even with drugs of this group it is possible to interrupt an episode of abnormal heart rate.
Medicines for arrhythmia are represented by urgent-acting drugs and medications for long-term use as part of ongoing therapy.
The first ones include the following names:
Metoprolol
Suitable for cupping in emergency cases. The antiarrhythmic effect is achieved approximately half an hour after administration.
The active substance is somewhat less active when compared with Amiodarone, but has additional effects, such as reducing blood pressure and restoring coronary blood flow by dilating the arteries of the same name.
Parallel use with potassium channel blockers is possible.
Anaprilin
It is used as widely both for continuous use and as part of the relief of arrhythmia attacks.
The drug has a particularly strong antiarrhythmic effect in the fight against supraventricular forms of the disorder.
The restoration of normal cardiac activity occurs quickly, in about 40-50 minutes, which makes Anaprilin an ideal option for eliminating many forms of arrhythmias.
The drug has especially proven itself in relieving attacks of sinus tachycardia.
Long-acting drugs:
Bisoprolol and its analogues
Unlike the previous two, it does not give a rapid effect. It acts gently, comprehensively, affects both adrenaline-sensitive receptors and the tone of the coronary arteries, normalizes nutrition and oxygen exchange in the myocardium.
The maximum antiarrhythmic effect is achieved 12 hours after taking the tablets and lasts for quite a long time.
There is a cumulative effect when the active substance accumulates, enhancing the therapeutic qualities of the drug.
Bisoprolol is used in the long-term treatment of cardiovascular pathologies. As a rule, in a system with drugs from other groups.
It prevents attacks of arrhythmias and reduces the risks of emergency conditions. Available in the form of tablets, there are several names - Biprolol, Concor.
Attention:
All beta blockers, without exception, have a negative property - they cannot be used for severe pulmonary and cardiac pathologies, because they increase the risk of death of the patient from complications.
Lipid-lowering drugs
These medications for coronary heart disease normalize cholesterol levels in the blood. They are prescribed along with a diet, the effect is achieved with constant use.
Often during ischemia, the coronary vessels are affected by atherosclerosis.
When the level of basic cholesterol and low-density cholesterol in the blood increases, the likelihood of atherosclerosis progression increases.
Lipid-lowering drugs restore normal cholesterol levels in the blood. Lipid-lowering drugs include:
- statins;
- fibrates.
Statins are more often prescribed and have fewer side effects. Do not use for a long time, because cholelithiasis may develop.
To achieve normal cholesterol levels, patients are prescribed medications from the group of statins (Atorvastatin, Fluvastatin, Lovastatin, Rosuvastatin), fibrates (Lipanor, Trilipix, Exlip, Bezalip), preparations of omega-3 polyunsaturated acids (Simvastatin, Colesevelam), nicotinic acid.
Nicotinic acid should not be prescribed to patients with liver pathologies.
Anesthetics
They have the potential to block excessive activity of cardiac structures and suppress myocardial contractility. For this reason, they act simultaneously on all chambers of the heart.
They are used in the treatment of dangerous types of ventricular arrhythmias (fibrillations, extrasytoles).
This is the main indication, because in other cases the risks are too high, there is no need to use anesthetics. These medications are produced in the form of an injection solution.
There are two main drugs:
- Novocainamide. It has a less pronounced effect, therefore it is not so dangerous.
- Lidocaine. It has no selectivity or selectivity of influence. Used less frequently, in extreme cases.
Both drugs give a rapid but short-term effect. They often provoke adverse reactions, which must be taken into account when using.
Drugs that do not belong to any class
There are relatively few of them.
Cardiac glycosides
The basis of the pharmaceutical effect of these drugs is the ability to enhance the pumping and contractile function of the heart and stimulate the functioning of cardiac structures.
With the paradoxical development of arrhythmia, when there is an increase in the frequency of beats, unevenness against the background of a reduced intensity of blood ejection, the use of glycosides is completely justified.
The main remedies are Digoxin and tincture of lily of the valley.
Attention:
The medications are not suitable for long-term use and require constant monitoring of objective indicators: blood pressure and heart rate.
Potassium-based products
Used to maintain normal myocardial contractility. This is especially true during long-term treatment with glucocorticoids and bronchodilators, which wash away potassium.
The classic and most accessible drug is Asparkam.
Drugs for sinus arrhythmia
For respiratory sinus arrhythmia, specific drugs are not prescribed, since such a heart rhythm is considered a normal variant. Most often, children who are diagnosed with respiratory or sinus arrhythmia outgrow this condition over time.
Severe sinus arrhythmia can accompany various acute conditions such as myocardial infarction, fever, anemia, etc. In such cases, the patient’s condition against the background of cardiac arrhythmia can significantly worsen, so the following are used:
- Beta blockers, which slow the heartbeat, but most patients are usually already taking drugs from this group as the main treatment for AMI.
Video: Adrenergic blockers. Anaprilin, Bisoprolol, Metoprolol, Nebivolol, Sermion, Phentolamine
Herbal antiarrhythmic
Represented by the key name - Quinidine. In terms of pharmaceutical properties it is close to Amidarone and is often compared with it. Can be used as an analogue.
The number of side effects is approximately at the same level. But it acts more roughly and intensely, and therefore the list of contraindications is somewhat wider.
At the same time, Quinidine can be prescribed to patients with ventricular forms of arrhythmias and is suitable for long-term use.
General principles of treatment
Treatment of arrhythmia begins after determining the cause that caused it. The patient is prescribed therapy only after a complete examination. In addition to antiarrhythmic drugs, a patient who has been diagnosed with psychosomatic disorders may be prescribed sedative medications. Taking tranquilizers is allowed. They are auxiliary and should be used in combination with medications against arrhythmia. All medications used for arrhythmia are taken at a certain time, usually after meals. They are allowed to be used only as prescribed by a doctor. Such medications are selected taking into account the form of arrhythmia, the severity of the disease and the age of the patient. Therefore, you cannot choose them yourself.
Arrhythmia can be triggered by taking certain medications. In this case, reduce their dosage or replace the medicine with an analogue.
Contraindications
Medicines for arrhythmia have various reasons for refusal of use. If you imagine an average list, it will look like this.
- Severe heart failure. Including after the condition has stabilized.
- Recent heart attack. Necrosis of heart tissue. The process of rehabilitation after a heart attack is described in this article, primary and secondary prevention are here.
- Disturbances in the conduction system of a muscular organ (heart block).
- Respiratory failure (in some cases).
- Individual intolerance to substances contained in the medicine. Allergy.
- Polyvalent immune reaction to medications. It is extremely rare and is not an absolute contraindication, but requires attention and caution.
- Pregnancy, breastfeeding period (also not always).
Side effects
The list of drugs is wide, each name has its own negative effects, so you need to consider a specific drug. In general, there are many of them, if you believe the instructions.
In fact, most of the medications described above are well tolerated, but individual characteristics must be taken into account.
If persistent adverse events develop, the drug is discontinued and a similar one is prescribed.
- Headache.
- Confusion.
- Disorientation in space.
- Noise in ears.
- Decrease in visual acuity.
- Allergic reactions.
- Fatigue, general asthenia (loss of strength).
- Diarrhea, vomiting, nausea, constipation, heartburn, belching are dyspeptic symptoms.
Tablets for cardiac arrhythmia and injection solutions are selected based on the specific case. It is impossible to name the best drug, there is simply no such thing. Self-prescription is excluded, it is dangerous.