Good day, dear readers!
In today's article we will look at tachycardia, as well as its symptoms, causes, types, diagnosis, treatment with conservative and folk remedies, prevention and other interesting information about this condition. So…
What is tachycardia?
Tachycardia is a special condition of the body in which the heart rate (HR) exceeds 90 beats per minute.
Tachycardia is a type of arrhythmia.
Doctors consider tachycardia as a symptom, which is most often caused by strong emotional experiences, increased physical activity of a person, the use of certain foods and medications, as well as a number of diseases of the cardiovascular, endocrine and other systems.
If we talk about the main symptoms that usually accompany an increased human heartbeat, then these are a feeling of palpitations, pulsation of the vessels of the cervical spine and dizziness. However, in some situations, tachycardia can lead to the development of life-threatening conditions such as myocardial infarction, acute heart failure and cardiac arrest.
It is important to note that tachycardia in children under 7 years of age is considered by most experts to be a normal condition of a healthy child.
In many cases, treatment of tachycardia comes down to removing from a person’s life the factor that caused the increased heart rate, for example, a ban on excessive coffee consumption, changing jobs with increased physical activity or frequent stress.
Development of tachycardia
The development of tachycardia is based on the activation of the sympathetic nervous system, which is part of the autonomic nervous system (ANS) located in the spine. Speaking in human language, the sympathetic nervous system is responsible for activating the work of one or another organ, but primarily the heart. There is also the parasympathetic nervous system, which is responsible for deactivating organ function. The vital activity of the organism, i.e. the functioning of human organs is regulated automatically, for example, a person’s inhalation is facilitated by the sympathetic nervous system, and exhalation by the parasympathetic.
If we translate this mechanism of the body’s vital activity into the plane of tachycardia, then we can draw the following picture: when the human body is exposed to any factor that is not characteristic of its normal state (stress, fear, overload, etc.), the sympathetic system increases the work of the heart - his sinus node, the heart rate increases. At the same time, if a person finds himself in a stressful situation, his production of adrenaline by neuroendocrine cells increases and its release into the blood, which is also the body’s protective function against possible danger. Adrenaline also increases your heart rate.
All this leads to the fact that the heart ventricles do not have time to fill with blood, which disrupts blood circulation throughout the body, lowers blood pressure, and the blood does not have time to fill with oxygen and deliver it in the required quantity to all organs.
That is why, with an increased heart rate, the patient experiences dizziness, up to loss of consciousness.
Tachycardia - ICD
ICD-10: I47-I49, R00.0; ICD-9: 427, 785.0.
Symptoms of tachycardia
The symptoms of tachycardia largely depend on the etiology of the rapid heartbeat, its severity and duration, as well as the general health of the person.
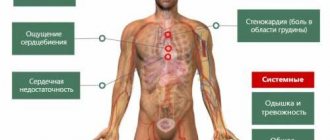
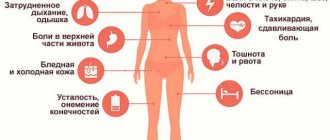
The main symptoms of tachycardia are:
- Feeling of strong heartbeat;
- Heaviness in the heart area, pain in the heart;
- Pulsation of neck vessels;
- Dizziness, up to loss of consciousness;
- Feeling short of air;
- Dyspnea;
- Arterial hypotension (low blood pressure).
Additional symptoms of tachycardia:
- Insomnia;
- General weakness, increased fatigue;
- Decreased appetite;
- Bad mood, increased irritability;
- Decreased diuresis;
- Body spasms.
Forecast
Sinus tachycardia in patients with heart disease is most often a manifestation of heart failure or left ventricular dysfunction. In these cases, the prognosis can be quite serious, since sinus tachycardia is a reflection of the reaction of the cardiovascular system to a decrease in ejection fraction and a disorder of intracardiac hemodynamics. In the case of physiological sinus tachycardia, even with pronounced subjective manifestations, the prognosis is usually satisfactory.
The prognosis for patients with ventricular tachycardia is unfavorable, since in most of them it is a manifestation of severe myocardial damage. Mortality is especially high among patients with acute myocardial infarction complicated by heart failure and hypotension.
Cardiac arrhythmia Bradycardia: symptoms and treatment Cardiac myocarditis Hypertension Rheumatism of the joints Angina pectoris - what should and should not be done at home?
Causes of tachycardia
There are a very large number of causes of rapid heartbeat, but all of them can be divided into 2 main groups - intracardiac and extracardiac factors. Let's look at them in more detail...
Internal (intracardial, or cardiac) causes of tachycardia:
Diseases and pathological conditions of the cardiovascular system: heart failure, myocardial infarction, coronary heart disease (CHD), severe angina, heart disease, left ventricular dysfunction, myocarditis, cardiosclerosis, cardiomyopathies, bacterial endocarditis, pericarditis, congenital long QT syndrome , mitral valve prolapse syndrome, arterial hypertension (hypertension), anemia (anemia), hypoxemia, acute vascular insufficiency (with loss of a large amount of blood, shock, collapse or fainting).
Read also Keratitis - symptoms, causes, types and treatment of keratitis
External (extracardiac, or extracardiac) causes of tachycardia
- Increased physical stress on the body, or prolonged stay in a position that is uncomfortable for the body, for example, when bending over (working in the garden, etc.);
- A sharp change in body position, for example, from a horizontal to a vertical position;
- Strong feelings, stress, fears, neuroses;
- Disruption of the normal functioning of the cerebral cortex and subcortical nodes;
- Disorders of the autonomic nervous system (ANS), including vegetative-vascular dystonia (VSD);
- Mental system disorders;
- The presence of infectious diseases: sepsis, sore throat, pneumonia, tuberculosis and other diseases that are accompanied by elevated and high body temperature - each additional 1°C of body temperature increases heart rate by 8 beats/minute (adults) and by 10-15 beats/minute (children );
- Endocrine system disorders: thyrotoxicosis (hyperthyroidism), pheochromocytoma
- The use of certain medications: sympathomimetics, or drugs that actively activate the sympathetic nervous system (drugs of adrenaline and norepinephrine), hormonal drugs (corticosteroids, thyroid-stimulating hormones), vagolytics (atropine), antihypertensive drugs (lowering blood pressure), diuretics (diuretics), psychotropic drugs (phenothiazides), some anesthetics, aminophylline, intoxication with cardiac glycosides and other drugs;
- Ingestion of certain harmful substances into the body: alcoholic beverages, nicotine, nitrates (poison that can be found in food);
- Drinking coffee and caffeinated drinks, strong tea;
- Dehydration of the body;
- Congenital pathologies;
- Severe painful attacks (colic and others);
- Bites of some representatives of the animal world - snakes, spiders, wasps or bees;
- There is also tachycardia of unknown etiology, which is classified as idiopathic tachycardia. This may include a rapid heartbeat as a result of the influence of spiritual forces on a person, but of course, official medicine usually does not recognize spiritual factors.
Surgery
Surgical treatment of paroxysmal tachycardia is used quite rarely and only in the absence of a stable effect from drug therapy. If the patient does not respond to conservative treatment, it is possible to ensure a normal rhythm and propagation of the impulse through the heart muscle through surgery.
The idea is that small electrodes are implanted into various parts of the heart, which take on the role of pacemakers. They regularly produce bioelectric impulses, suppressing the rhythm of other nodes. The most modern models even independently regulate the operating mode, based on blood pressure and normal filling of the ventricles with blood. In recent years, the installation of such a device is carried out using a minimally invasive method through the main (large) vessels.
Another treatment option is radiofrequency catheter ablation. Through the femoral vein, the doctor inserts special catheters into the heart, takes an ECG and determines pathological pacemakers. After this, the detected area is exposed to radio frequency radiation. In most cases, this suppresses cell activity and eliminates the cause of the arrhythmia. This treatment method is used for Wolff-Parkinson-White syndrome and other structural disorders.
Types of tachycardia
The classification of tachycardia includes the following types of this condition:
By etiology:
Physiological tachycardia. The heart rate (HR) increases due to the influence of a certain factor on the body. It is an adequate reaction of the body to a stimulus (fear, stress, taking certain substances, exposure of the body to certain climatic conditions, etc.);
Pathological tachycardia. The main reason for heart rate is the presence of acquired or hereditary pathology of the heart and other organs while the body is at rest. It is a dangerous condition, a long stay in which contributes to the development of heart diseases such as coronary heart disease (CHD) or myocardial infarction. Pathological tachycardia is accompanied by a decrease in the filling of the ventricles with blood, which leads to insufficient blood supply to all organs and, accordingly, their nutrition. At the same time, a person’s blood pressure drops, and a long period of this pathological condition leads to the development of hypoxia and arrhythmogenic cardiopathy, in which the efficiency of the heart is significantly reduced. The longer a person remains in this state, the worse the prognosis for full recovery.
Idiopathic tachycardia. The cause of palpitations among medical workers cannot be identified.
According to the source generating electrical impulses in the heart:
Sinus tachycardia - develops as a result of an increase in the activity of the sinus, or sinoatrial node, which is actually the main source of electrical impulses that sets the rhythm of the heart (HR) at rest. It is characterized by a gradual onset, heart rate up to 120–220 beats/minute and regular heartbeat rhythm.
Ectopic (paroxysmal) tachycardia - the source of electrical impulses originates in the atria (supraventricular) or ventricles (ventricular). It is characterized by a paroxysmal course, which both appear suddenly and disappear, but their duration can range from several minutes to several tens of hours, during which the heart rate remains consistently high - from 140 to 250 beats/minute, with the correct heartbeat rhythm. Such attacks are called paroxysms.
Paroxysmal tachycardia includes 3 forms:
- Atrial (supraventricular, or supraventricular) tachycardia - most often, the cause of rapid heartbeat is the activation of the sympathetic nervous system, which usually occurs during fear, stress, shock, etc.;
- Ventricular tachycardia (VT) - the most common cause is dystrophic changes in the heart muscle, for example - about 85-95% of this form of heart rate is observed in patients with coronary heart disease or myocarditis;
- Nodal tachycardia.
Read also Malignant tumor (Cancer) - causes, symptoms, types and treatment of cancer
Ventricular fibrillation (VF). It is often a complication of extensive transmural myocardial infarction or a continuation of the development of paroxysmal ventricular tachycardia, although some scientists consider ventricular fibrillation and ventricular tachycardia as one phenomenon. It is characterized by chaotic and irregular contraction of the heart muscle at a level of 250 to 600 beats per minute, which in some cases leads to complete cardiac arrest. In addition, after 15-20 seconds the patient may experience severe dizziness and lose consciousness, and after 40 seconds he may experience a single tonic spasm of skeletal muscles, accompanied by involuntary urination and defecation. At the same time, the victim’s pupils increase in size, which after one and a half to two minutes are dilated to the maximum level. The patient begins to breathe quickly, but then breathing slows down, and after 2 minutes clinical death occurs.
In the medical world, ventricular fibrillation is conventionally divided into 3 types:
Primary VF. Development occurs in the first 4-48 hours from the onset of myocardial infarction, but before the onset of left ventricular failure and other complications of the attack. Characterized by high mortality of patients.
Secondary VF. Development occurs in patients with a heart attack against the background of insufficient blood circulation in the left ventricle and cardiogenic shock.
Late VF. Development occurs 48 hours later (in most cases 2-6 weeks) from the onset of myocardial infarction and is characterized by 40-60% of deaths.
First aid for a person during an attack, what to do
First aid is based on a specific algorithm of actions aimed at eliminating the attack and restoring sinus rhythm:
- Place the patient on the bed with a pillow under the head. A strong bend in the neck should not be allowed, otherwise the arteries will be compressed and blood circulation will worsen.
- During an attack, the patient experiences a lack of air, so you need to open all the windows in the room.
- Moisten the patient's face with cold water or place a gauze bandage on the forehead. This will lead to a reflexive decrease in heart rate.
- Remove the victim from his belt or tie to ensure proper breathing.
- Drop Corvalol into a glass of water according to the instructions.
- Ask the patient to close his eyes and gently press his fingers on the eyeballs (10 seconds). This will also slow down your heart rate at the reflex level.
- If the symptoms of tachycardia do not subside, then you need to ask the victim to take a deep breath, hold his breath and push hard with his mouth open, and at the end cough loudly.
During these activities, you must call an ambulance.
Diagnosis of tachycardia
Diagnosis of tachycardia includes the following types of examination:
- Anamnesis;
- Electrocardiography (ECG), as well as daily Holter ECG monitoring;
- Echocardiography (EchoCG);
- Magnetic resonance imaging (MRI) of the heart;
- Electrophysiological study (EPS) of the heart.
Additional examination methods:
- General blood analysis;
- Electroencephalography (EEG) of the brain.
Treatment of tachycardia with folk remedies
Important!
Before using folk remedies against tachycardia, be sure to consult your doctor! Herbs, fruits, lemon and honey. Peel 4 lemons and squeeze out the juice, which should be mixed with 250 g of honey. Next, grind 16 leaves of indoor geranium (kalachik) and 18 almonds through a meat grinder, then mix this mixture with 10 g of valerian tincture and 10 g of hawthorn tincture. Mix all the prepared ingredients thoroughly and add 6 whole camphor grains to the mixture. The resulting folk remedy for tachycardia should be taken 1 tbsp. spoon in the morning, on an empty stomach, 30 minutes before meals, and store in the refrigerator.
Garlic and lemon. Add 10 medium chopped garlic cloves, juice from 10 lemons and 1 liter of honey to a 3-liter jar. Mix all the ingredients thoroughly, cover the jar tightly with plastic and set aside to infuse for 7 days. You need to take the resulting product 2 tbsp. spoons, 1 time per day, until complete recovery.
Adonis. Boil 250 ml of water in a small saucepan, then turn the heat to low and add 1 teaspoon of adonis herb to the water. Boil the product for no more than 3 minutes, then remove from heat, cover with a lid and set aside to infuse for 30 minutes. Next, you need to strain the broth and take 1 tbsp. spoon 3 times a day.
To achieve the maximum effect from Adonis, take the following remedy throughout the day: peel and cut 500 g of lemons, to which add a couple of tablespoons of honey and 20 crushed apricot kernels. Mix the weight thoroughly and take this mixture 1 tbsp. spoon morning and evening. By the way, apricot kernels contain vitamin B17, which also has an antitumor effect.
Adonis. Pour 1 teaspoon of adonis herb with a glass of boiling water and put the product on low heat for 5 minutes, then remove it from the heat, cover and let it brew for 2 hours. Next, you need to strain the product and take 1 tbsp. spoon 3 times a day, 30 minutes before meals.
Hawthorn. Pour 1 tbsp. spoon of hawthorn flowers with a glass of boiling water, cover the product with a lid, let it brew for about 30 minutes, then strain and take the prepared remedy for tachycardia, 100 ml 3 times a day, 30 minutes before meals. The course of treatment is until complete recovery.
Prevention of tachycardia
Prevention of tachycardia includes compliance with the following recommendations:
- Minimize the consumption of coffee, strong tea, alcohol, chocolate;
- Avoid overeating, try to give preference to vegetables and fruits that contain large amounts of vitamins and microelements, especially pay attention to replenishing the body with magnesium and potassium;
- Maintain a work/rest/sleep schedule;
- Avoid working with a lot of stress;
- Avoid taking medications without consulting your doctor;
- Try to move more, but at the same time do not overstrain your body with excessive physical activity;
- Spend more time in nature.
What else is worth knowing?
Doctors recommend patients with tachycardia not only drug treatment. To normalize your heart rate, it is very important to adhere to a healthy lifestyle and eliminate all possible factors that could cause a new attack of tachycardia. To do this, you should follow simple recommendations.
- The first step is to eliminate negative irritants - alcohol, smoking, caffeine. They accelerate the heart rate and can cause sudden attacks of tachycardia.
- Avoid excessive physical activity.
- Normalize your sleep schedule and try not to overstrain your nervous system.
- Avoid noisy places, try not to be in a crowd.
- Establish a clear daily routine - start the morning with therapeutic exercises, introduce a diet.
- Eat exclusively healthy foods, avoid fatty foods and fast foods.
- It is important to learn how to relax after a working day - for this you can do yoga, listen to relaxing music or walk in the fresh air.
- You should regularly visit a cardiologist to prevent attacks of tachycardia.
With repeated attacks of tachycardia against the background of the development of other symptoms, it is a reason to consult a doctor. It should be remembered that tachycardia is a symptom of many serious diseases.